Abstract
Purpose
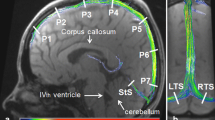
Susceptibility-weighted imaging (SWI) visualizes small cerebral veins with high sensitivity and could, thus, enable quantification of hemodynamics of deep medullary veins. We aimed to evaluate volume changes of deep medullary veins in patients with acute cerebral venous sinus thrombosis (CVST) over time in comparison to healthy controls.
Methods
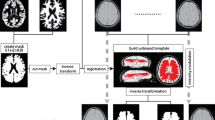
All magnetic resonance imaging (MRI) experiments were executed at 3 T using a 32-channel head coil. Based on SWI and semiautomatic postprocessing (statistical parametric mapping [SPM8] and ANTs), the volume of deep medullary veins was quantified in 14 patients with acute CVST at baseline and the 6‑month follow-up, as well as in 13 healthy controls undergoing repeated MRI examination with an interscan interval of at least 1 month.
Results
Deep medullary venous volume change over time was significantly different between healthy controls and patient groups (p < 0.001). Patients with superior sagittal sinus thrombosis (SSST) showed a significant decline from baseline to follow-up measurements (9.8 ± 4.9 ml versus 7.5 ± 4.2 ml; p = 0.02), whereas in patients with transverse sinus thrombosis (TST) and healthy controls no significant volume changes were observable.
Conclusions
Venous volume quantification was feasible and reproducible both in healthy volunteers and in patients. The decrease of venous volume in patients over time represents improvement of venous drainage, reduction of congestion, and normalization of microcirculation due to treatment. Thus, quantification of venous microcirculation could be valuable for estimation of prognosis and guidance of CVST therapy in the future.



Similar content being viewed by others
References
Reichenbach JR, Venkatesan R, Schillinger DJ, Kido DK, Haacke EM. Small vessels in the human brain: MR venography with deoxyhemoglobin as an intrinsic contrast agent. Radiology. 1997;204:272–7.
Sehgal V, Delproposto Z, Haacke EM, Tong KA, Wycliffe N, Kido DK, Xu Y, Neelavalli J, Haddar D, Reichenbach JR. Clinical applications of neuroimaging with susceptibility-weighted imaging. J Magn Reson Imaging. 2005;22:439–50.
Ogawa S, Lee TM, Kay AR, Tank DW. Brain magnetic resonance imaging with contrast dependent on blood oxygenation. Proc Natl Acad Sci USA. 1990;87:9868–72.
Hermier M, Nighoghossian N. Contribution of susceptibility-weighted imaging to acute stroke assessment. Stroke. 2004;35:1989–94.
Mahvash M, Pechlivanis I, Charalampaki P, Jansen O, Mehdorn HM. Visualization of small veins with susceptibility-weighted imaging for stereotactic trajectory planning in deep brain stimulation. Clin Neurol Neurosurg. 2014;124:151–5.
Xia X, Tan C. A quantitative study of magnetic susceptibility-weighted imaging of deep cerebral veins. J Neuroradiol. 2013;40:355–9.
Bousser M, Ferro JM. Cerebral venous thrombosis: An update. Lancet Neurol. 2007;6:162–70.
Coutinho JM, Zuurbier SM, Stam J. Declining mortality in cerebral venous thrombosis: a systematic review. Stroke. 2014;45:1338–41.
Canhão P, Ferro JM, Lindgren AG, Bousser M, Stam J, Barinagarrementeria F. Causes and predictors of death in cerebral venous thrombosis. Stroke. 2005;36:1720–5.
Agid R, Shelef I, Scott JN, Farb RI. Imaging of the intracranial venous system. Neurologist. 2008;14:12–22.
Idbaih A, Boukobza M, Crassard I, Porcher R, Bousser M, Chabriat H. MRI of clot in cerebral venous thrombosis: high diagnostic value of susceptibility-weighted images. Stroke. 2006;37:991–5.
Kawabori M, Kuroda S, Kudo K, Terae S, Kaneda M, Nakayama N, Iwasaki Y. Susceptibility-weighted magnetic resonance imaging detects impaired cerebral hemodynamics in the superior sagittal sinus thrombosis – case report. Neurol Med Chir (Tokyo). 2009;49:248–51.
Selim M, Fink J, Linfante I, Kumar S, Schlaug G, Caplan LR. Diagnosis of cerebral venous thrombosis with echo-planar T2*-weighted magnetic resonance imaging. Arch Neurol. 2002;59:1021.
Egger K, Dempfle AK, Yang S, Schwarzwald R, Harloff A, Urbach H. Reliability of cerebral vein volume quantification based on susceptibility-weighted imaging. Neuroradiology. 2016;58(9):937–42.
Tustison NJ, Avants BB, Cook PA, Zheng Y, Egan A, Yushkevich PA, Gee JC. N4ITK: improved N3 bias correction. IEEE Trans Med Imaging. 2010;29:1310–20.
Avants BB, Tustison NJ, Song G, Cook PA, Klein A, Gee JC. A reproducible evaluation of ANTs similarity metric performance in brain image registration. Neuroimage. 2011;54:2033–44.
Yushkevich PA, Avants BB, Das SR, Pluta J, Altinay M, Craige C. Bias in estimation of hippocampal atrophy using deformation-based morphometry arises from asymmetric global normalization: an illustration in ADNI 3 T MRI data. Neuroimage. 2010;50:434–45.
Reuter M, Rosas HD, Fischl B. Highly accurate inverse consistent registration: a robust approach. Neuroimage. 2010;53:1181–96.
Reuter M, Fischl B. Avoiding asymmetry-induced bias in longitudinal image processing. Neuroimage. 2011;57:19–21.
Avants BB, Epstein CL, Grossman M, Gee JC. Symmetric diffeomorphic image registration with cross-correlation: evaluating automated labeling of elderly and neurodegenerative brain. Med Image Anal. 2008;12:26–41.
R Development Core Team. R: A language and environment for statistical computing. Vienna: R Foundation for Statistical Computing; 2008.
Bates D, Mächler M, Bolker B, Walker S. Fitting linear mixed-effects models using lme4. J Stat Softw. 2015;67:1–48.
Nowinski WL, Puspitasari F, Volkau I, Orrison WW, Knopp MV. Quantification of the human cerebrovasculature: a 7T and 320-row CT in vivo study. J Comput Assist Tomogr. 2013;37:117–22.
Nowinski WL, Chua BC, Marchenko Y, Puspitsari F, Volkau I, Knopp MV. Three-dimensional reference and stereotactic atlas of human cerebrovasculature from 7T. Neuroimage. 2011;55:986–98.
Einhäupl K, Stam J, Bousser M, De Bruijn SFTM, Ferro JM, Martinelli I, Masuhr F. EFNS guideline on the treatment of cerebral venous and sinus thrombosis in adult patients. Eur J Neurol. 2010;17:1229–35.
Herweh C, Griebe M, Geisbüsch C, Szabo K, Neumaier-Probst E, Hennerici MG, Bendszus M, Ringleb PA, Nagel S. Frequency and temporal profile of recanalization after cerebral vein and sinus thrombosis. Eur J Neurol. 2016;23:681–7.
Baumgartner RW. Recanalisation of cerebral venous thrombosis. J Neurol Neurosurg Psychiatry. 2003;74:459–61.
Bauerle J, Egger K, Harloff A. Idiopathische intrakranielle Hypertension. Nervenarzt. 2017;88:191–200.
Ferro JM, Canhão P, Stam J, Bousser M, Barinagarrementeria F. Prognosis of cerebral vein and dural sinus thrombosis: results of the International Study on Cerebral Vein and Dural Sinus Thrombosis (ISCVT). Stroke. 2004;35:664–70.
Stolz E, Kaps M, Kern A, Babacan SS, Dorndorf W. Transcranial color-coded duplex sonography of intracranial veins and sinuses in adults. Reference data from 130 volunteers. Stroke. 1999;30:1070–5.
Valdueza JM, Schmierer K, Mehraein S, Einhaupl KM. Assessment of normal flow velocity in basal cerebral veins: a transcranial doppler ultrasound study. Stroke. 1996;27:1221–5.
Tong KA, Ashwal S, Obenaus A, Nickerson JP, Kido D, Haacke EM. Susceptibility-weighted MR imaging: a review of clinical applications in children. AJNR Am J Neuroradiol. 2008;29:9–17.
Schaller B. Physiology of cerebral venous blood flow: from experimental data in animals to normal function in humans. Brain Res Brain Res Rev. 2004;46:243–60.
Mittal S, Wu Z, Neelavalli J, Haacke EM. Susceptibility-weighted imaging: technical aspects and clinical applications, part 2. AJNR Am J Neuroradiol. 2009;30:232–52.
Acknowledgements
We thank Hansjörg Mast for performing MRI examinations.
Funding
Prof. Dr. A. Harloff has received funding from Deutsche Forschungsgemeinschaft (DFG), Bonn, Germany, grant #HA5399/3-1.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A. K. Dempfle, A. Harloff, F. Schuchardt, J. Bäuerle, S. Yang, H. Urbach and K. Egger declare that they have no competing interests.
Additional information
A. K. Dempfle and A. Harloff contributed equally to this work.
Rights and permissions
About this article
Cite this article
Dempfle, A.K., Harloff, A., Schuchardt, F. et al. Longitudinal Volume Quantification of Deep Medullary Veins in Patients with Cerebral Venous Sinus Thrombosis. Clin Neuroradiol 28, 493–499 (2018). https://doi.org/10.1007/s00062-017-0602-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-017-0602-z