Abstract
Objective
It is unknown whether the effect of diabetes on patients with unprotected left main coronary artery (LMCA) disease differs according to the different revascularization strategies. This study was conducted to evaluate the impact of diabetes on patients with unprotected LMCA disease treated with either percutaneous coronary intervention (PCI) or coronary artery bypass grafting (CABG).
Patients and methods
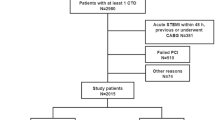
We prospectively enrolled 823 consecutive patients with unprotected LMCA disease who had drug-eluting stent (DES; n = 331) implantation or underwent CABG (n = 492) in the study. We compared the effects of diabetes on clinical outcomes according to different revascularization strategies.
Results
Among 823 eligible patients enrolled, 226 had diabetes. In the DES population, no significant differences were observed in occurrences of death, cardiac death, repeat revascularization, stroke, and major adverse cardiac and cerebrovascular events. However, the risks of the composite of death/myocardial infarction (MI)/stroke (21.5 % DM vs. 7.2 % non-DM; p = 0.001) and MI (15.4 % DM vs. 1.6 % non-DM; p = 0.000) were significantly higher in the diabetic patients than those without diabetes. In the CABG population, similar rates of all clinical endpoints were observed between the diabetic and nondiabetic group.
Conclusion
Diabetes was associated with worse outcome in patients undergoing DES implantation for the treatment of unprotected LMCA disease. However, its negative prognostic impact was not found among patients undergoing CABG.
Zusammenfassung
Ziel
Ob sich die Auswirkungen eines Diabetes mellitus auf Patienten mit koronarer Herzkrankheit (KHK) des ungeschützten Hauptstamms (LMCA) bei verschiedenen Revaskularisierungsstrategien unterscheiden, ist nicht bekannt. Die vorliegende Studie wurde durchgeführt, um den Einfluss eines Diabetes auf Patienten mit KHK des ungeschützten LMCA zu untersuchen, die entweder mittels perkutaner Koronarintervention (PCI) oder mit einem Koronarbypass (CABG) behandelt wurden.
Methoden
An der Studie nahmen 823 konsekutive Patienten mit KHK des ungeschützten LMCA teil, bei denen die Versorgung mit der Implantation von medikamentenfreisetzenden Stents (DES, n = 331) oder einem CABG (n = 492) erfolgte. Es wurden die Auswirkungen eines Diabetes auf klinische Ergebnisse in Abhängigkeit von den verschiedenen Revaskularisierungsstrategien verglichen.
Ergebnisse
Von 823 für die Studie geeigneten Patienten wiesen 226 einen Diabetes mellitus (DM) auf. In der DES-Gruppe wurden keine signifikanten Unterschiede hinsichtlich des Auftretens von Todesfällen, Herztod, wiederholter Revaskularisierung, Schlaganfall und schweren unerwünschten kardialen und zerebrovaskulären Ereignissen (MACCE) beobachtet. Allerdings war das Risiko für den zusammengesetzten Endpunkt aus Tod/Herzinfarkt/Schlaganfall (21,5 % DM vs. 7,2 % ohne DM; p = 0,001) und Herzinfarkt (15,4 % DM vs. 1,6 % ohne DM; p = 0,000) bei Patienten mit Diabetes signifikant höher als bei Patienten ohne. In der CABG-Gruppe wurden ähnliche Raten aller klinischen Endpunkte für die Gruppen mit und ohne Diabetes beobachtet.
Schlussfolgerung
Ein Diabetes mellitus stand mit einem schlechteren Ergebnis bei Patienten mit DES-Implantation zur Therapie einer KHK des ungeschützten LMCA in Zusammenhang. Jedoch war der negative prognostische Einfluss des Diabetes nicht bei Patienten mit CABG festzustellen.


Similar content being viewed by others
References
Levine GN, Bates ER, Blankenship JC et al (2011) 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. Circulation 124(23):e574–e651
Morice MC, Serruys PW, Kappetein AP et al (2010) Outcomes in patients with de novo left main disease treated with either percutaneous coronary intervention using paclitaxel-eluting stents or coronary artery bypass graft treatment in the synergy between percutaneous coronary intervention with TAXUS and cardiac surgery (SYNTAX) trial. Circulation 121:2645–2653
Chakravarty T, Buch MH, Naik H et al (2011) Predictive accuracy of SYNTAX score for predicting long-term outcomes of unprotected left main coronary artery revascularization. Am J Cardiol 107:360–366
Kim YH, Park DW, Kim WJ et al (2010) Validation of SYNTAX (synergy between PCI with TAXUS and cardiac surgery) score for prediction of outcomes after unprotected left main coronary revascularization. J Am Coll Cardiol Intv 3:612–623
Buszman PE, Kiesz SR, Bochenek A et al (2008) Acute and late outcomes of unprotected left main stenting in comparison with surgical revascularization. J Am Coll Cardiol 51:538–545
Capodanno D, Miano M, Cincotta G et al (2010) EuroSCORE refines the predictive ability of SYNTAX score in patients undergoing left main percutaneous coronary intervention. Am Heart J 159:103–109
Serrão M, Pereira A, Santos N et al (2009) Clinical and angiographic profile of the diabetic patient: one-year follow-up. Rev Port Cardiol 28:417–423
Van Werkhoven JM, Cademartiri F, Seitun S et al (2010) Diabetes: prognostic value of CT coronary angiography-comparison with a nondiabetic population. Radiology 256:83–92
Lenzen M, Ryden L, Ohrvik J et al (2006) Diabetes known or newly detected, but not impaired glucose regulation, has a negative influence on 1-year outcome in patients with coronary artery disease: a report from the Euro Heart Survey on diabetes and the heart. Eur Heart J 27:2969–2974
Thygesen K, Alpert JS, White HD, on behalf of the Joint ESC/ACCF/AHA/WHF Task Force for the Redefinition of Myocardial Infarction (2007) Universal definition of myocardial infarction. Eur Heart J 28:2525–2538
PocockSJ, HendersonRA, RickardsAF et al (2005) Meta-analysis of randomized trials comparing coronary angioplasty with bypass surgery. Lancet 346:1184–1189
Aggarwal A, Schneider DJ, Sobel BE, Dauerman HL (2003) Comparison of inflammatory markers in patients with diabetes mellitus versus those without before and after coronary arterial stenting. Am J Cardiol 92:924–929
Sobel BE (2001) Acceleration of restenosis by diabetes: pathogenetic implications. Circulation 103:1185–1187
Hong SJ, Kim MH, Ahn TH et al (2006) Multiple predictors of coronary restenosis after drug-eluting stent implantation in patients with diabetes. Heart 92:1119–1124
Kumar R, Lee TT, Jeremias A et al (2007) Comparison of outcomes using sirolimus-eluting stenting in diabetic versus nondiabetic patients with comparison of insulin versus non-insulin therapy in the diabetic patients. Am J Cardiol 100:1187–1191
Stettler C, Allemann S, Wandel S et al (2008) Drug eluting and bare metal stents in people with and without diabetes: collaborative network meta-analysis. BMJ 337:a1331
Iijima R, Ndrepepa G, Mehilli J et al (2007) Impact of diabetes mellitus on long-term outcomes in the drug-eluting stent era. Am Heart J 154:688–693
Carson JL, Scholz PM, Chen AY et al (2002) Diabetes mellitus increases short-term mortality and morbidity in patients undergoing coronary artery bypass graft surgery. J Am Coll Cardiol 40:418–423
Sabik JF III, Blackstone EH, Gillinov AM et al (2006) Occurrence and risk factors for reintervention after coronary artery bypass grafting. Circulation 114:I-454–I-460
Slaughter MS, Olson MM, Lee JTJ, Ward HB (1993) A fifteen-year wound surveillance study after coronary artery bypass. Ann Thorac Surg 56:1063–1068
Mohammadi S, Dagenais F, Mathieu P et al (2007) Long-term impact of diabetes and its comorbidities in patients undergoing isolated primary coronary artery bypass graft surgery. Circulation 116:I-220–I-225
Leavitt BJ, Sheppard L, Maloney C et al (2004) Effect of diabetes and associated conditions on long-term survival after coronary artery bypass graft surgery. Circulation 110:II-41–II-44
Compliance with ethical guidelines
Conflict of interest. X. Yu, Y. Luo, J. He, Y. Gao, Y. Zhang, X. Zhang, C. Wu, X. Ren, S. Lv and F. Chen state that there are no conflicts of interest. All studies on humans described in the present manuscript were carried out with the approval of the responsible ethics committee and in accordance with national law and the Helsinki Declaration of 1975 (in its current, revised form). Informed consent was obtained from all patients included in studies.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Yu, X., Luo, Y., He, J. et al. Unprotected left main coronary artery disease after revascularization. Herz 40, 116–122 (2015). https://doi.org/10.1007/s00059-013-3959-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-013-3959-z
Keywords
- Left main coronary artery disease
- Percutaneous coronary intervention
- Drug-eluting stent
- Coronary artery bypass grafting
- Diabetes mellitus