Abstract
Introduction
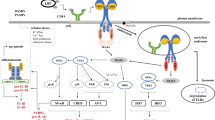
We aimed to investigate the involvement of surface TLRs and endosomal TLRs in the regulation of SARM expression by TLR2 ligands (Pam2CSK4 and Pam3CSK4).
Materials and methods
Mouse macrophage cell line (RAW264.7) was treated with either Pam2CSK4 or Pam3CSK4 (TLR2 ligands) at a concentration of 100 ng/ml. At indicated time points, the treated cells were lysed. The gene and protein expression of SARM were determined by RT-PCR and immunoblotting, respectively. For silencing of TLR9 function, the cells were transfected with TLR9 siRNAs before stimulation by these two TLR2 ligands
Results
The SARM expression was upregulated at both transcriptional and translational levels in time-dependent manner during activation of Pam2CSK4 and Pam3CSK4 in mouse macrophages. Blocking of ligand internalization by cytochalasin D showed interference effect with SARM expression. Moreover, our results also demonstrated that endosomal acidification and TLR9 were required for SARM expression suggesting the essential role of endosomal compartment acidification and TLR9 in regulating SARM expression.
Conclusion
Our findings suggested the collaboration of TLR2–TLR9 at least in the regulation of SARM expression. However, the underlying mechanism that participated in these two TLRs cooperation is underinvestigated.





Similar content being viewed by others
References
Akira S. TLR signaling. Curr Top Microbiol Immunol. 2006;311:1–16.
Sassai M, Yamamoto M. Pathogen recognition receptors: ligands and signaling pathways by Toll-like receptors. Int Rev Immunol. 2013;32:116–33.
Kawai T, Akira S. The roles of TLRs, RLRs and NLRs in pathogen recognition. Int Immunol. 2009;21:317–37.
Takeuchi O, Akira S. Pattern recognition receptors and inflammation. Cell. 2010;140:805–20.
Kondo T, Kawai T, Akira S. Dissecting negative regulation of Toll-like receptor signaling. Trends Immunol. 2012;33:449–58.
Liew FY, Xu D, Brint EK, O’Neill LA. Negative regulation of toll-like receptor-mediated immune responses. Nat Rev Immunol. 2005;5:446–58.
Carty M, Goodbody R, Schroder M, Stack J, Moynagh PN, Bowie AG. The human adaptor SARM negatively regulates adaptor protein TRIF-dependent Toll-like receptor signaling. Nat Immunol. 2006;7:1074–81.
Pudla M, Limposuwan K, Utaisincharoen P. Burkholderia pseudomallei-induced expression of a negative regulator, sterile-alpha and Armadillo motif-containing protein, in mouse macrophages: a possible mechanism for suppression of the MyD88-independent pathway. Infect Immun. 2011;79:2921–7.
Utaisincharoen P, Anuntagool N, Chaisuriya P, Pichyangkul S, Sirisinha S. CpG ODN activates NO and iNOS production in mouse macrophage cell line (RAW264.7). Clin Exp Immunol. 2002;128:467–73.
Akira S, Uematsu S, Takeuchi O. Pathogen recognition and innate immunity. Cell. 2006;124:783–801.
O’Neill LA, Bowie AG. The family of five: TIR-domain-containing adaptors in Toll-like receptor signalling. Nat Rev Immunol. 2007;7:353–64.
Gleeson PA. The role of endosomes in innate and adaptive immunity. Semin Cell Dev Biol. 2014;31:64–72.
Clague MJ, Urbe S, Aniento F, Gruenberg J. Vacuolar ATPase activity is required for endosomal carrier vesicle formation. J Biol Chem. 1994;269:21–4.
Marshansky V, Futai M. The V-type H+-ATPase in vesicular trafficking: targeting, regulation and function. Curr Opin Cell Biol. 2008;20:415–26.
Dietrich N, Lienenklaus S, Weiss S, Gekara NO. Murine toll-like receptor 2 activation induces type I interferon responses from endolysosomal compartments. PLoS One. 2010;5:e10250.
Stack J, Doyle SL, Connolly DJ, Reinert LS, O’Keeffe KM, McLoughlin RM, et al. TRAM is required for TLR2 endosomal signaling to type I IFN induction. J Immunol. 2014;193:6090–102.
Bauer S. Toll-like receptor 9 processing: the key event in Toll-like receptor 9 activation? Immunol Lett. 2013;149:85–7.
Brencicova E, Diebold SS. Front cellular infect microbiol nucleic acids and endosomal pattern recognition: how to tell friend from foe? Front Cell Infect Microbiol. 2013;3:1–14.
Kawai T, Akira S. The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors. Nat Immunol. 2010;11:373–84.
Lee BL, Moon JE, Shu JH, Yuan L, Newman ZR, Schekman R, et al. UNC93B1 mediates differential trafficking of endosomal TLRs. eLife. 2013;2:e00291.
Macedo GC, Magnani DM, Carvalho NB, Bruna-Romero O, Gazzinelli RT, Oliveira SC. Central role of MyD88-dependent dendritic cell maturation and proinflammatory cytokine production to control Brucella abortus infection. J Immunol. 2008;180:1080–7.
Zhan R, Han Q, Zhang C, Tian Z, Zhang J. Toll-Like Receptor 2 (TLR2) and TLR9 play opposing roles in host innate immunity against Salmonella enterica serovar Typhimurium infection. Infect Immun. 2015;83:1641–9.
Lee KS, Jeong ES, Heo SH, Seo JH, Jeong DG, Choi YK. IL-10 suppresses bactericidal response of macrophages against Salmonella typhimurium. J Microbiol. 2011;49:1050–3.
Acknowledgements
Matsayapan Pudla acknowledges support from the Talent Management Program of Mahidol University. Panthong Kulsantiwong was supported by the Udon Thani Rajabhat University scholarship for development of educational personnel. This research was supported by a research grant from Thailand Research Fund (Grant number BRG5980004 and MRG5980057) and Mahidol University.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by: John Di Battista.
Rights and permissions
About this article
Cite this article
Pudla, M., Kulsantiwong, P., Srisaowakarn, C. et al. Regulation of sterile α- and armadillo motif (SARM) containing protein expression in Pam2CSK4- and Pam3CSK4-activated mouse macrophage cell line (RAW264.7) requires TLR9. Inflamm. Res. 66, 1099–1105 (2017). https://doi.org/10.1007/s00011-017-1090-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-017-1090-y