Abstract
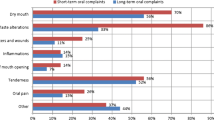
AIM: Presenting features associated with orofacial granulomatosis (OFG) and oral Crohn’s disease (OCD) are varied, making successful diagnosis and management difficult. The aim of this service evaluation was to establish a profile of patients with these conditions attending a paediatric oral medicine clinic and to determine their overall satisfaction with the care received. STUDY DESIGN: A retrospective case note analysis to establish the patient profile and a postal patient satisfaction questionnaire for service evaluation. METHODS: All patients with OFG and OCD who had attended the joint paediatric dentistry/oral medicine clinic at Charles Clifford Dental Hospital, Sheffield in the previous 14 years were included in the study. Hospital case notes were retrospectively reviewed and patient demographics, clinical features, investigations, diagnosis, treatment and outcomes of treatment were recorded. An anonymous patient satisfaction questionnaire using the Healthcare Satisfaction Generic Module of the Paediatric Quality of Life Inventory (PedsQLTM) was distributed to all patients by mail. RESULTS: A total of 24 patients (13 females and 11 males) were identified. Median age at presentation was 11 years (SD ± 3.79, range 2–15). Fifteen patients (63%) were diagnosed with OCD, and 9 (37%) with OFG. Overall, the most common orofacial feature was oral ulceration (75%) followed by lip/facial swelling (71%), angular cheilitis (67%) and mucosal cobblestoning (67%). Differences in presentation were seen between the two conditions with oral ulceration (87%) and mucosal cobblestoning (80%) being the most frequently observed features of OCD and lip swelling (78%) and angular cheilitis (67%) being the most common features of OFG. 58% of patients reported relief of symptoms through treatment. Thirteen patient satisfaction questionnaires were completed (54%). 85% (n=11) felt the overall care received in the clinic was ‘excellent’. CONCLUSIONS: This service evaluation highlights the variety of presenting features of OFG and OCD. Despite only a moderate response to treatment, patient satisfaction with the service was high, emphasising the importance of good communication when managing children with chronic, debilitating conditions.
Similar content being viewed by others
References
Al-Johani K, Moles DR, Hodgson T et al. Onset and progression of clinical manifestations of orofacial granulomatosis. Oral Dis 2009;15:214–219.
Al-Johani KA, Moles DR, Hodgson TA, et al. Orofacial granulomatosis: clinical features and long-term outcome of therapy. J Am Acad Dermatol 2010; 62:611–620.
Bradley PJ, Ferlito A, Devaney KO, et al. Crohn’s disease manifesting in the head and neck. Acta Otolaryngol 2004; 124:237–241.
Campbell H, Escudier M, Patel P, et al. Distinguishing orofacial granulomatosis from crohn’s disease: two separate disease entities? Inflamm Bowel Dis 2011; 17:2109–2115.
Challacombe SJ. Oro-facial granulomatosis and oral Crohns disease: are they specific diseases and do they predict systemic Crohns disease? Oral Dis 1997; 3:127–129.
Cohen G. Age and health status in a patient satisfaction survey. Soc Sci Med 1996; 42:1085–93.
Department for Education and Skills UK. Every Child Matters. The Stationary Office 2003. www.education.gov.uk/consultations/downloadableDocs/Every-ChildMatters.pdf
Department of Health UK. Getting the right start: National Service Framework for Children, Young People and Maternity Services: Standard for Hospital Services. The Stationary Office 2003. www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_4006182
Elliott T, Campbell H, Escudier M, et al. Experience with anti-TNF-α therapy for orofacial granulomatosis. J Oral Pathol Med 2011; 40:14–19.
Endo H, Rees TD. Cinnamon products as a possible etiologic factor in orofacial granulomatosis. Med Oral Patol Oral Cir Bucal 2007; 12:E440–444.
Ghandour K, Issa M. Oral Crohn’s disease with late intestinal manifestations. Oral Surg Oral Med Oral Pathol 1991; 72:565–567.
Grave B, McCullough M, Wiesenfeld D. Orofacial granulomatosis—a 20-year review. Oral Dis 2009; 15:46–51.
Harty S, Fleming P, Rowland M, et al. A prospective study of the oral manifestations of Crohn’s disease. Clin Gastroenterol Hepatol 2005; 3:886–891.
Hegarty A, Hodgson T, Porter S. Thalidomide for the treatment of recalcitrant oral Crohn’s disease and orofacial granulomatosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2003; 95;576–585.
Hildebrand H, Finkel Y, Grahnquist L, et al. Changing pattern of paediatric inflammatory bowel disease in northern Stockholm 1990–2001. Gut 2003; 52:1432–1434.
Kolho KL, Heiskanen K, Verkasalo M, et al. Orofacial granulomatosis in children-a challenge for diagnosis and treatment. Int J Pediatr Otorhinolaryngol 2011; 75:864–867.
Kramer IR, Pindborg JJ, Bezroukov V, et al. Guide to epidemiology and diagnosis of oral mucosal diseases and conditions. World Health Organization. Community Dent Oral Epidemiol 1980; 8:1–26.
Leao JC, Hodgson T, Scully C, et al. Review article: orofacial granulomatosis. Aliment Pharmacol Ther 2004; 20:1019–1027.
McCartan BE, Healy CM, McCreary CE, et al. Characteristics of patients with orofacial granulomatosis. Oral Dis 2011; 17:696–704.
Mignogna MD, Fedele S, Lo Russo L, et al. The multiform and variable patterns of onset of orofacial granulomatosis. J Oral Pathol Med 2003; 32:200–205.
National Research Ethics Service Consultation E-Group. Differentiating audit, service evaluation and research, 2006. www.nres.npsa.nhs.uk
Patton D, Ferguson M, Forsyth A, et al. Oro-facial granulomatosis: a possible allergic basis. Br J Oral Maxillofac Surg 1985; 23:235–242.
Pittock S, Drumm B, Fleming P, et al. The oral cavity in Crohn’s disease. J Pediatr 2001; 138:767–771.
Rampton DS. Management of Crohn’s disease. BMJ 1999; 319:1480–1485.
Riordain RN, McCreary C. Validity and reliability of a newly developed quality of life questionnaire for patients with chronic oral mucosal diseases. J Oral Pathol Med 2011; 40:604–609.
Riordain RN, Meaney S, McCreary C. Impact of chronic oral mucosal disease on daily life: preliminary observations from a qualitative study. Oral Dis 2011; 17:265–269.
Saalman R, Mattsson U, Jontell M. Orofacial granulomatosis in childhood — a clinical entity that may indicate Crohn’s disease as well as food allergy. Acta Paediatr 2009; 98:1162–1167.
Sanderson J, Nunes C, Escudier M, et al. Oro-facial granulomatosis: Crohn’s disease or a new inflammatory bowel disease? Inflamm Bowel Dis 2005; 11:840–846.
Tilakaratne WM, Freysdottir J, Fortune F. Orofacial granulomatosis: review on aetiology and pathogenesis. J Oral Pathol Med 2008; 37:191–195.
White A, Nunes C, Escudier M, et al. Improvement in orofacial granulomatosis on a cinnamon- and benzoate-free diet. Inflamm Bowel Dis 2006; 12:508–514.
Wiesenfeld D, Ferguson MM, Mitchell DN et al. Oro-facial granulomatosis — a clinical and pathological analysis. Q J Med 1985; 54:101–113.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Howell, J.L., Bussell, R.M., Hegarty, A.M. et al. Service evaluation of patients with orofacial granulomatosis and patients with oral Crohn’s disease attending a paediatric oral medicine clinic. Eur Arch Paediatr Dent 13, 191–196 (2012). https://doi.org/10.1007/BF03262869
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03262869