Abstract
Purpose
The incidence and duration of apnea during sevoflurane anesthesia have not been fully characterized. We hypothesized that sevoflurane at slowly increasing concentrations reduces incidence and shortens the duration of apnea compared to administration of a highly concentrated anesthetic mixture.
Methods
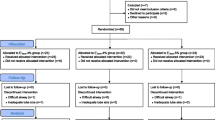
131 women were randomly assigned to receive 35% oxygen in air and sevoflurane at: incremental concentrations of 1%, from 1% to 8% (group 1–8%,n = 42); decremental-incremental concentrations of 2%, from 8% to 4% and then from 4% to 8% (group 8–4-8%,n = 36); or fixed concentrations of 8% for induction of anesthesia (group 8%,n = 53). A blinded investigator observed whether and for how long patients stopped breathing. Results: All groups reached 2.5 minimum alveolar concentration of end-tidal sevoflurane. Although apnea was observed in all groups, it was more frequent in the 8% group than in 1 to 8% (68%vs 21%,P < 0.05) or 8 to 4 to 8% groups (68%vs 20%,P < 0.05). Duration of apnea was also more pronounced in the 8% group than in 1 to 8% and 8 to 4 to 8% groups ( 58 ± 25 svs 32 ± 18 sec,P < 0.05 andvs 35 ± 16 sec,P < 0.05, respectively).
Conclusions
Sevoflurane induces apnea more frequently and for longer duration at a fixed high concentration compared to incremental or decremental-incremental concentrations. Decrementalincremental concentrations offer the additional advantage of a speed of induction similar to that elicited by the 8% concentration.
Résumé
Objectif
L’incidence et la durée de l’apnée pendant l’anesthésie au sévoflurane n’ont pas été entièrement définies. Nous avons cru que le sévoflurane administré en concentrations lentement progressives réduisait l’incidence et la durée de l’apnée comparativement à un mélange anesthésique très concentré.
Méthode
Nous avons réparti au hasard 131 femmes qui ont reçu un mélange de 35 % d’oxygène dans de l’air et du sévoflurane : en concentrations incrémentielles de 1 %, de 1 % à 8 % (groupe 1–8 %, n = 42); en concentrations décrémentielles-incrémentielles de 2 %, de 8 % à 4 %, puis de 4 % à 8 % (groupe 8–4–8 %, n = 36) ou en concentrations fixes de 8 %, pour l’induction de l’anesthésie (groupe 8 %, n = 53). Un chercheur impartial a vérifié la présence et le temps d’apnée.
Résultats
Une concentration alvéolaire minimale de 2,5 de sévoflurane télé-expiratoire a été atteinte chez toutes les patients. L’apnée a été observée dans tous les groupes, mais était plus fréquente dans le groupe de 8 % que dans celui de 1 à 8 % (68 % vs 21 %,P < 0,05) ou de 8–4–8 % (68 % vs 20 %,P < 0,05). La durée de l’apnée a été aussi plus prononcée dans le groupe de 8 % que dans ceux de 1 à 8 % et de 8–4–8 % ( 58 ± 25 s vs 32 ± 18 s,P < 0,05 et vs 35 ± 16 s,P < 0,05, respectivement).
Conclusion
L’apnée est plus fréquente et dure plus longtemps avec de fortes concentrations fixes de sévoflurane qu’avec des concentrations incrémentielles ou décrémentielles-incrémentielles. Ces dernières concentrations ont un avantage supplémentaire, celui de permettre une induction aussi rapide qu’une concentration à 8 %.
Article PDF
Similar content being viewed by others
References
Muzi M, Robinson BJ, Ebert TJ, O’Brien TJ. Induction of anesthesia and tracheal intubation with sevoflurane in adults. Anesthesiology 1996; 85:536–43.
Scheller MS, Nakakimura K, Fleischer JE, Zornow MH. Cerebral effects of sevoflurane in the dog: comparison with isoflurane and enflurane. Br J Anaesth 1990; 65:388–92.
Scheller MS, Tateishi A, Drummond JC, Zornow MH. The effects of sevoflurane on cerebral blood flow, cerebral metabolic rate for oxygen, intracranial pressure, and the electroencephalogram are similar to those of isoflurane in the rabbit. Anesthesiology 1988; 68:548–51.
Mutoh T, Nishimura R, Kim HY, Matsunaga S, Sasaki N. Cardiopulmonary effects of sevoflurane, compared with halothane, enflurane, and isoflurane, in dogs. Am J Vet Res 1997; 58:885–90.
Green WB Jr. The ventilatory effects of sevoflurane. Anesth Analg 1995; 81:S23–6.
Smith I, Ding Y, White PF. Comparison of induction, maintenance, and recovery characteristics of sevoflurane-N2O and propofol-sevoflurane-N2O with propofol-isoflurane- N2O anesthesia. Anesth Analg 1992; 74:253–9.
Fredman B, Nathanson MH, Smith I, Wang J, Klein K, White PF. Sevoflurane for outpatient anesthesia: a comparison with propofol. Anesth Analg 1995; 81:823–8.
Doi M, Ikeda K. Respiratory effects of sevoflurane. Anesth Analg 1987; 66:24–4.
Peacock JE, Lewis RP, Reilly CS, Nimmo WS. Effects of different rates of infusion of propofol for induction of anaesthesia in elderly patients. Br J Anaesth 1990; 65:346–52.
Stucke AG, Stuth EA, Tonkovic-Capin V, et al. Effects of sevoflurane on excitatory neurotransmission to medullary expiratory neurons and on phrenic nerve activity in a decerebrate dog model. Anesthesiology 2001; 95:485–91.
Thwaites A, Edmends S, Smith I. Inhalation induction with sevoflurane: a double-blind comparison with propofol. Br J Anaesth 1997; 78:356–61.
Ti LK, Chow MY, Lee TL. Comparison of sevoflurane with propofol for laryngeal mask airway insertion in adults. Anesth Analg 1999; 88:908–12.
Guracha Boru K, Drummond GB. Comparison of breathing methods for inhalation induction of anaesthesia. Br J Anaesth 1999; 83:650–3.
Anonymous. Practice guidelines for management of the difficult airway. An updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology 2003; 98: 1269–77.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study has been supported by departmental funds from the University of Perugia.
This report was presented at the annual meeting of the American Society of Anesthesiologists, New Orleans, Louisiana, October 16, 2001.
Rights and permissions
About this article
Cite this article
Pancaro, C., Giovannoni, S., Toscano, A. et al. Apnea during induction of anesthesia with sevoflurane is related to its mode of administration. Can J Anesth 52, 591–594 (2005). https://doi.org/10.1007/BF03015767
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03015767