Abstract
Purpose
To determine the incidence and duration of ECG abnormalities in healthy adults during short duration outpatient surgery and their relationship to important clinical events.
Method
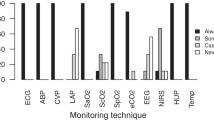
In 381, ASA Class I, day surgery patients undergoing short surgical procedures the ECG was monitored prospectively for evidence of abnormalities. The attending anaesthetist administered the anaesthetic and made all clinical decisions while relying on routine monitors (ECG, oximeter, BR capnometer, oxygen analyser, low pressure alarm and anaesthetic gas monitors). Intra-operative events of clinical significance (e.g., light anaesthesia, regurgitation, coughing, hypotension, arterial desaturation, hiccoughs etc), ECG abnormalities and their duration were documented.
Results
Electrocardiographic abnormalities were detected in 21 % of patients as follows: sinus tachycardia (11 %), artifacts (7%), premature atrial contractions (1.6%), lead disconnects (1%), sinus bradycardia (0.5%) and premature ventricular contractions (0.3%). All abnormalities resolved spontaneously within three minutes. Intra-operative incidents of consequence occurred in only 2.6%: light anaesthesia (5), arterial desaturation > 5% (2), hypotension (1), hiccough (1) and régurgitation (1). All incidents were detected clinically and by pulse oximetry. The ECG did not detect any of the incidents and was normal during the events.
Conclusion
Routine ECG monitoring did not detect intra-operative incidents in healthy adults during short outpatient procedures. Detected ECG abnormalities were benign and resolved spontaneously within three minutes. Firm conclusions as to the safety implications of withdrawing ECG monitoring cannot be drawn from this study. Guidelines may need to be reviewed to determine whether ECG monitoring in such cases should be optional rather than mandatory.
Résumé
Objectif
Déterminer l’incidence et la durée des anomalies de l’ECG chez des adultes en bonne santé durant des chirurgies ambulatoires de courte durée, et la relation entre ces anomalies et des événements cliniques importants.
Méthode
Chez 381 patients de chirurgie ambulatoire, de classe I de l’ASA, subissant des procédures chirurgicales courtes, l’ECG a été monitoré de façon prospective à la recherche d’anomalies. L’anesthésiste responsable du patient administrait l’anesthésie et prenait toutes les décisions cliniques selon les informations fournies par les moniteurs usuels, soit l’ECG, le saturomètre, la mesure de la pression artérielle, le capnomètre, l’oxymètre, l’analyseur de gaz anesthésiques et le système d’alarme de basse pression. On a documenté les anomalies à l’ECG et leur durée, de même que les événements peropératoires ayant une signification clinique (vg anesthésie légère, régurgitation, toux, hypotension, désaturation, hoquet, etc.)
Résultats
Des anomalies électrocadiographiques ont été détectées chez 21 % des patients: tachycardie sinusale 11%, artefacts 7%, extrasystoles auriculaires 1.6%, déconnection des électrodes 1%, bradycardie sinusale 0.5% et extrasystoles ventriculaires 0.3%. Toutes les anomalies se sont corrigées spontanément en moins de trois minutes. Des incidents peropératoires significatifs sont survenus dans 2.6% des cas seulement: anesthésie légère 5 patients, désaturation de ≥ 5% 2 patients, hypotension I patient, hoquet I patient et régurgitation I patient. Tous les incidents ont été détectés diniquement et par le saturomètre. L’ECG est demeuré normal durant tous ces incidents et n’a pas permis d’en détecter un seul.
Conclusion
Le mon’rtorage de routine de l’ECG n’a pas permis de détecter d’incidents peropératoires chez des adultes en bonne santé opérés en chirurgie ambulatoire pour des procédures courtes. Les anomalies détectées étaient bénignes et se sont toutes résolues en deçà de 3 minutes. Des conclusions définitives concernant les implications quant à la sécurité de cesser le monitorage de l’ECG ne peuvent être tirées de cette étude. Les lignes de conduite pourraient être revues et, dans ces cas, l’ECG pourrait devenir facultatif plutôt qu’essentiel.
Article PDF
Similar content being viewed by others
References
Guidelines to the practice of anaesthesia. Can J Anaesth 1996; 43(Suppl): 1–9.
Kroll DA, Cheney FW. Medicolegal aspects of anesthesia practice.In: Barash PG, Cullen BF, Stoelting RK (Eds.). Clinical Anesthesia, 2nd ed. Philadelphia: J.B. Iippincott Company, 1992: 115–25.
Fragen RJ, Avram MJ. Nonopioid intravenous anesthetics.In: Barash PG, Cullen BF, Stoelting RK (Eds.). Clinical Anesthesia, 2nd ed. Philadelphia: J.B. Iippincott Company, 1992: 385–412.
Ludbrook GL, Russel WJ, Webb RK, Klepper ID, Currie M. The Australian Incident Monitoring Study. The electrocardiograph: applications and limitations — an analysis of 2000 incident reports. Anaesth Intensive Care 1993; 21: 558–64.
Russell PH, Coakley CS. Electrocardiographic observation in the operating room. Anesth Analg 1969; 48: 784–8.
Knill RL, Gelb AW. Peripheral chemoreceptors during anesthesia. Are the watchdogs sleeping? (Editorial) Anesthesiology 1982; 57: 151–2.
Smith J, Calahan M, Benefiel D, et al. Intra operative detection of myocardial ischaemia at high risk patients: electro cardiographic versus two-dimensional transosophageal echocardiography. Circulation 1985; 72: 1015–19.
Hur D, Gravenstein JS. Is ECG monitoring in the operating room cost effective? Biotelemetry Patient Monitg 1979; 6: 200–6.
Southall DP, Johnston F, Shinebourne EA, Johnstone PG. A 24-hour electro cardiographic study of heart rate and rhythm patterns in population of healthy children. Br Heart J 1981; 45: 281–9.
Brodsky M, Wu D, Denes P, Kanakis C, Rosen KM. Arrhythmias documented by 24 hour continuous electrocardiographic monitoring in 50 male medical students without apparent heart disease. Am J Cardiol 1977; 39: 390–8.
Tyers MR, Russell WJ, Runciman WB. Electrocardiographic: monitoring in anaesthesia. Anesth Intensive Care 1988; 16: 66–9.
Chung F, Mezei G. Intraoperative adverse events during ambulatory surgical procedures. Can J Anaesth 1997; 44: A70-A.
Webb RK, Van der Walt JH, Runciman WB, et al. Which monitor? An analysis of 2000 incident reports. Anaesth Intensive Care 1993; 21: 529–42.
Pearsall FJ, Davidson JA, Asbury AJ. Attitudes to the Association of Anaesthetists recommendations for standards of monitoring during anaesthesia and recovery. Anaesthesia 1995; 50: 649–53.
Australian and New Zealand College of Anaesthetists. Monitoring during anaesthesia. 1995(Oct); Policy document No P 18.
Shomaker TS. Practice policies in anesthesia: a foretaste of practice in the 21st century. Anesth Analg 1995; 80: 388–403.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zabani, I., Vaghadia, H., Chilvers, C.R. et al. Electrocardiographic monitoring in healthy young adult outpatients: mandatory or optional?. Can J Anaesth 45, 424–428 (1998). https://doi.org/10.1007/BF03012577
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03012577