Abstract
Background
Gamma-glutamyltransferase (γ-GT) is used as a marker of alcohol-related pathology, while γ-GT is recently considered to be an oxidative stress marker.
Aim
The present study aimed to investigate the correlation between the oxidative status and γ-GT levels, in association with menopausal stages.
Methods
In total, 252 women, who were subjectively healthy, were divided into three groups: premenopausal, perimenopausal, and postmenopausal. The circulating oxidative status was evaluated by the diacron-reactive oxygen metabolite (d-ROM) test. In addition to serum γ-GT, routine blood investigations, including lipid, glucose, and inflammatory parameters, were performed.
Results
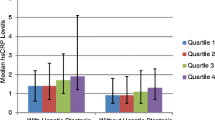
The median γ-GT level was 17 U/L and the mean d-ROM level was 335 Carr U in all subjects. On multiple regression analysis, independent significant positive correlations were observed between d-ROM and high-sensitivity CRP levels in three groups, while there was a significant positive correlation between d-ROM and γ-GT levels only in the premenopausal group but not in the perimenopausal and postmenopausal groups.
Discussion
The significant relationship between d-ROM and γ-GT at active estrogen stage may indicate a different oxidative stress condition by memopausal stage. The reasons of this relationship should be further explored.
Conclusion
A positive relationship between d-ROM and γ-GT levels, both as known as oxidative stress-related markers, could exist in premenopausal women.
Similar content being viewed by others
References
Harlow SD, Gass M, Hall JE et al (2012) Executive summary of the Stages of Reproductive Aging Workshop +10: addressing the unfinished agenda of staging reproductive aging. J Clin Endocrinol Metab 97:1159–1168
Chiang K, Parthasarathy S, Santanam N (2004) Estrogen, neutrophils and oxidation. Life Sci 75:2425–2438
White RE, Gerrity R, Barman SA et al (2010) Estrogen and oxidative stress: a novel mechanism that may increase the risk for cardiovascular disease in women. Steroids 75:788–793
Massafra C, Gioia D, De Felice C et al (2000) Effects of estrogens and androgens on erythrocyte antioxidant superoxide dismutase, catalase and glutathione per-oxidase activities during the menstrual cycle. J Endocrinol 167:447–452
Bednarek-Tupikowska G, Bohdanowicz-Pawlak A, Bidzińska B et al (2001) Serum lipid peroxide levels and erythrocyte glutathione peroxidase and superoxide dismutase activity in premenopausal and postmenopausal women. Gynecol Endocrinol 15:298–303
Stice JP, Eiserich JP, Knowlton AA (2009) Role of aging vs the loss of estrogens in the reduction in vascular function in female rats. Endocrinology 150:212–219
Serviddio G, Loverro G, Vicino M et al (2002) Modulation of endometrial redox balance during the menstrual cycle: relation with sex hormones. J Clin Endocrinol Metab 87:2843–2848
Bellanti F, Matteo M, Rollo T et al (2013) Sex hormones modulate circulating antioxidant enzymes: impact of estrogen therapy. Redox Biol 1:340–346
Whitfield JB (2001) Gamma glutamyl transferase. Crit Rev Clin Lab Sci 38:263–355
Lee DS, Evans JC, Robins SJ et al (2007) Gamma glutamyl transferase and metabolic syndrome, cardiovascular disease, and mortality risk: the Framingham Heart Study. Arterioscler Thromb Vasc Biol 27:127–133
Lee DH, Ha MH, Kim JR et al (2002) Gamma-glutamyltransferase, alcohol, and blood pressure. A four year follow-up study. Ann Epidemiol 12:90–96
Lee DH, Ha MH, Kim JH et al (2003) Gammaglutamyltransferase and diabetes—a 4 year follow-up study. Diabetologia 46:359–364
Turgut O, Yilmaz A, Yalta K et al (2006) Gamma-glutamyltransferase is a promising biomarker for cardiovascular risk. Med Hypotheses 67:1060–1064
Emdin M, Pompella A, Paolicchi A (2005) Gamma-glutamyltransferase, atherosclerosis, and cardiovascular disease: triggering oxidative stress within the plaque. Circulation 112:2078–2080
Lee DH, Blomhoff R, Jacobs DR Jr (2004) Is serum gamma glutamyltransferase a marker of oxidative stress? Free Radic Res 38:535–539
Nilssen O, Førde OH (1994) Seven-year longitudinal population study of change in gamma-glutamyltransferase: the Tromsø Study. Am J Epidemiol 139:787–792
Trotti R, Carratelli M, Barbieri M et al (2001) Oxidative stress and a thrombophilic condition in alcoholics without severe liver disease. Haematologica 86:85–91
Gerardi G, Usberti M, Martini G et al (2002) Plasma total antioxidant capacity in hemodialyzed patients and its relationships to other biomarkers of oxidative stress and lipid peroxidation. Clin Chem Lab Med 40:104–110
Kotani K, Sakane N (2011) Association between lipoprotein(a) and oxygen reactive metabolite in asymptomatic subjects. Pol Arch Med Wewn 121:247–252
Barbagallo CM, Polizzi F, Severino M et al (2002) Distribution of risk factors, plasma lipids, lipoproteins and dyslipidemias in a small Mediterranean island: the Ustica Project. Nutr Metab Cardiovasc Dis 12:267–274
Kearney PM, Whelton M, Reynolds K et al (2005) Global burden of hypertension: analysis of worldwide data. Lancet 365:217–223
No authors (2010) Summary of revisions for the 2010 Clinical Practice Recommendations. Diabetes Care 33:S3
Chen JT, Kotani K (2011) The pattern of correlation between cardiometabolic and oxidative stress-related markers in premenopausal and postmenopausal subjects. J Jpn Soc Menopause Womens Health 19:221–226 (in Japanese with English Abstract)
Victorino VJ, Panis C, Campos FC et al (2013) Decreased oxidant profile and increased antioxidant capacity in naturally postmenopausal women. Age (Dordr) 35:1411–1421
Cornelli U, Belcaro G, Cesarone MR et al (2013) Analysis of oxidative stress during the menstrual cycle. Reprod Biol Endocrinol 11:74
Sakane N, Fujiwara S, Sano Y et al (2008) Oxidative stress, inflammation, and atherosclerotic changes in retinal arteries in the Japanese population; results from the Mima study. Endocr J 55:485–488
Hirose H, Kawabe H, Komiya N et al (2009) Relations between serum reactive oxygen metabolites (ROMs) and various inflammatory and metabolic parameters in a Japanese population. J Atheroscler Thromb 16:77–82
Gaskins AJ, Wilchesky M, Mumford SL et al (2012) Endogenous reproductive hormones and C-reactive protein across the menstrual cycle: the BioCycle Study. Am J Epidemiol 175:423–431
Mukamal KJ, Muller JE, Maclure M et al (2002) Variation in the risk of onset of acute myocardial infarction during the menstrual cycle. Am J Cardiol 90:49–51
Prior JC (2005) Ovarian aging and the perimenopausal transition: the paradox of endogenous ovarian hyperstimulation. Endocrine 26:297–300
Hale GE, Zhao X, Hughes CL et al (2007) Endocrine features of menstrual cycles in middle and late reproductive age and the menopausal transition classified according to the Staging of Reproductive Aging Workshop (STRAW) staging system. J Clin Endocrinol Metab 92:3060–3067
MacNaughton J, Banah M, McCloud P et al (1992) Age related changes in follicle stimulating hormone, luteinizing hormone, oestradiol and immunoreactive inhibin in women of reproductive age. Clin Endocrinol (Oxf) 36:339–345
Burger HG, Hale GE, Dennerstein L et al (2008) Cycle and hormone changes during perimenopause: the key role of ovarian function. Menopause 15:603–612
Burger H (2008) The menopausal transition-endocrinology. J Sex Med 5:2266–2273
Denti L, Marchini L, Pasolini G et al (1995) Lipoprotein Lp(a) and cerebrovascular disease in the elderly: correlations with the severity of extracranial carotid atherosclerosis assessed by ultrasonography. Acta Biomed Ateneo Parm 66:175–183
Schindhelm RK, Dekker JM, Nijpels G et al (2006) Alanine aminotransferase predicts coronary heart disease events: a 10-year follow-up of the Hoorn Study. Atherosclerosis 191:391–396
Diamanti-Kandarakis E, Piperi C, Kalofoutis A et al (2005) Increased levels of serum advanced glycation end-products in women with polycystic ovary syndrome. Clin Endocrinol (Oxf) 62:37–43
Economou F, Xyrafis X, Livadas S et al (2009) In overweight/obese but not in normal-weight women, polycystic ovary syndrome is associated with elevated liver enzymes compared to controls. Hormones (Athens) 8:199–206
Bosy-Westphal A, Geisler C, Onur S et al (2006) Value of body fat mass vs anthropometric obesity indices in the assessment of metabolic risk factors. Int J Obes (Lond) 30:475–483
Ryan MC, Fenster Farin HM, Abbasi F et al (2008) Comparison of waist circumference versus body mass index in diagnosing metabolic syndrome and identifying apparently healthy subjects at increased risk of cardiovascular disease. Am J Cardiol 102:40–46
van Dis I, Kromhout D, Geleijnse JM et al (2009) Body mass index and waist circumference predict both 10-year nonfatal and fatal cardiovascular disease risk: study conducted in 20,000 Dutch men and women aged 20–65 years. Eur J Cardiovasc Prev Rehabil 16:729–734
Tison GH, Blaha MJ, Nasir K et al (2015) Relation of anthropometric obesity and computed tomography measured nonalcoholic fatty liver disease (from the Multiethnic Study of Atherosclerosis). Am J Cardiol 116:541–546
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest. The authors are solely responsible for the content and writing of this paper.
Human and Animal Rights
The study was approved by the institutional ethics committee.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Chen, JT., Kotani, K. Serum γ-glutamyltranspeptidase and oxidative stress in subjectively healthy women: an association with menopausal stages. Aging Clin Exp Res 28, 619–624 (2016). https://doi.org/10.1007/s40520-015-0460-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-015-0460-y