Abstract
Purpose
We investigated the role of adjuvant concurrent chemoradiation therapy (CCRT) in patients with a microscopically positive resection margin (R1) after curative resection for extrahepatic cholangiocarcinoma (EHCC).
Methods/patients
A total of 84 patients treated with curative resection for EHCC were included. Fifty-two patients with negative resection margins did not receive any adjuvant treatments (R0 + S group). The remaining 32 patients with microscopically positive resection margins received either adjuvant CCRT (R1 + CCRT group, n = 19) or adjuvant radiation therapy (RT) alone (R1 + RT group, n = 13).
Results
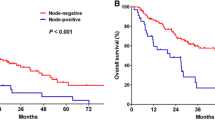
During the median follow-up period of 26 months, the 2-year locoregional recurrence-free survival (LRRFS), disease-free survival (DFS), and overall survival rates (OS) were: 81.8, 62.6, and 61.5% for R0 + S group; 71.8, 57.8, and 57.9% for R1 + CCRT group; and 16.8, 9.6, and 15.4% for R1 + RT group, respectively. Multivariate analysis revealed that the R1 + CCRT group did not show any significant difference in survival rates compared with the R0 + S group. The R1 + RT group had lower LRRFS [hazard ratio (HR) 3.008; p = 0.044], DFS (HR 2.364; p = 0.022), and OS (HR 2.417; p = 0.011) when compared with the R0 + S and R1 + CCRT group.
Conclusions
A lack of significant survival difference between R0 + S group and R1 + CCRT group suggests that adjuvant CCRT ameliorates the negative effect of microscopic positive resection margin. In contrast, adjuvant RT alone is appeared to be inadequate for controlling microscopically residual tumor.


Similar content being viewed by others
References
Jarnagin WR, Ruo L, Little SA, Klimstra D, D’Angelica M, DeMatteo RP, et al. Patterns of initial disease recurrence after resection of gallbladder carcinoma and hilar cholangiocarcinoma: implications for adjuvant therapeutic strategies. Cancer. 2003;98(8):1689–700. https://doi.org/10.1002/cncr.11699.
Wakai T, Shirai Y, Moroda T, Yokoyama N, Hatakeyama K. Impact of ductal resection margin status on long-term survival in patients undergoing resection for extrahepatic cholangiocarcinoma. Cancer. 2005;103(6):1210–6. https://doi.org/10.1002/cncr.20906.
Murakami Y, Uemura K, Hayashidani Y, Sudo T, Hashimoto Y, Ohge H, et al. Prognostic significance of lymph node metastasis and surgical margin status for distal cholangiocarcinoma. J Surg Oncol. 2007;95(3):207–12. https://doi.org/10.1002/jso.20668.
Sasaki R, Takeda Y, Funato O, Nitta H, Kawamura H, Uesugi N, et al. Significance of ductal margin status in patients undergoing surgical resection for extrahepatic cholangiocarcinoma. World J Surg. 2007;31(9):1788–96. https://doi.org/10.1007/s00268-007-9102-7.
Konishi M, Iwasaki M, Ochiai A, Hasebe T, Ojima H, Yanagisawa A. Clinical impact of intraoperative histological examination of the ductal resection margin in extrahepatic cholangiocarcinoma. Br J Surg. 2010;97(9):1363–8. https://doi.org/10.1002/bjs.7122.
Ribero D, Amisano M, Lo Tesoriere R, Rosso S, Ferrero A, Capussotti L. Additional resection of an intraoperative margin-positive proximal bile duct improves survival in patients with hilar cholangiocarcinoma. Ann Surg. 2011;254(5):776–81. https://doi.org/10.1097/SLA.0b013e3182368f85 (discussion 81-3).
Groot Koerkamp B, Wiggers JK, Allen PJ, Besselink MG, Blumgart LH, Busch OR, et al. Recurrence rate and pattern of perihilar cholangiocarcinoma after curative intent resection. J Am Coll Surg. 2015;221(6):1041–9. https://doi.org/10.1016/j.jamcollsurg.2015.09.005.
Tsukahara T, Ebata T, Shimoyama Y, Yokoyama Y, Igami T, Sugawara G, et al. Residual carcinoma in situ at the ductal stump has a negative survival effect: an analysis of early-stage cholangiocarcinomas. Ann Surg. 2016;. https://doi.org/10.1097/SLA.0000000000001944.
Jarnagin WR, Shoup M. Surgical management of cholangiocarcinoma. Semin Liver Dis. 2004;24(2):189–99. https://doi.org/10.1055/s-2004-828895.
Ito F, Agni R, Rettammel RJ, Been MJ, Cho CS, Mahvi DM, et al. Resection of hilar cholangiocarcinoma: concomitant liver resection decreases hepatic recurrence. Ann Surg. 2008;248(2):273–9. https://doi.org/10.1097/SLA.0b013e31817f2bfd.
van Gulik TM, Kloek JJ, Ruys AT, Busch OR, van Tienhoven GJ, Lameris JS, et al. Multidisciplinary management of hilar cholangiocarcinoma (Klatskin tumor): extended resection is associated with improved survival. Eur J Surg Oncol. 2011;37(1):65–71. https://doi.org/10.1016/j.ejso.2010.11.008.
Oh D, Lim DH, Heo JS, Choi SH, Choi DW, Ahn YC, et al. The role of adjuvant radiotherapy in microscopic tumor control after extrahepatic bile duct cancer surgery. Am J Clin Oncol. 2007;30(1):21–5. https://doi.org/10.1097/01.coc.0000245467.97180.78.
Matsuda T, Fujita H, Harada N, Kunimoto Y, Tanaka T, Kimura T, et al. Impact of adjuvant radiation therapy for microscopic residual tumor after resection of extrahepatic bile duct cancer. Am J Clin Oncol. 2013;36(5):461–5. https://doi.org/10.1097/COC.0b013e31825494ab.
Kim S, Kim SW, Bang YJ, Heo DS, Ha SW. Role of postoperative radiotherapy in the management of extrahepatic bile duct cancer. Int J Radiat Oncol Biol Phys. 2002;54(2):414–9.
Borghero Y, Crane CH, Szklaruk J, Oyarzo M, Curley S, Pisters PW, et al. Extrahepatic bile duct adenocarcinoma: patients at high-risk for local recurrence treated with surgery and adjuvant chemoradiation have an equivalent overall survival to patients with standard-risk treated with surgery alone. Ann Surg Oncol. 2008;15(11):3147–56. https://doi.org/10.1245/s10434-008-9998-7.
Park JH, Choi EK, Ahn SD, Lee SW, Song SY, Yoon SM, et al. Postoperative chemoradiotherapy for extrahepatic bile duct cancer. Int J Radiat Oncol Biol Phys. 2011;79(3):696–704. https://doi.org/10.1016/j.ijrobp.2009.12.031.
Kim K, Chie EK, Jang JY, Kim SW, Han SW, Oh DY, et al. Adjuvant chemoradiotherapy after curative resection for extrahepatic bile duct cancer: a long-term single center experience. Am J Clin Oncol. 2012;35(2):136–40. https://doi.org/10.1097/COC.0b013e318209aa29.
Kim MY, Kim JH, Kim Y, Byun SJ. Postoperative radiotherapy appeared to improve the disease free survival rate of patients with extrahepatic bile duct cancer at high risk of loco-regional recurrence. Radiat Oncol J. 2016;34(4):297–304. https://doi.org/10.3857/roj.2016.01879.
Committee AJC. AJCC cancer staging manual. Chicago: AJCC; 2010.
Gonzalez Gonzalez D, Gouma DJ, Rauws EA, van Gulik TM, Bosma A, Koedooder C. Role of radiotherapy, in particular intraluminal brachytherapy, in the treatment of proximal bile duct carcinoma. Ann Oncol. 1999;10(Suppl 4):215–20.
Nakano K, Chijiiwa K, Toyonaga T, Ueda J, Takamatsu Y, Kimura M, et al. Combination therapy of resection and intraoperative radiation for patients with carcinomas of extrahepatic bile duct and ampulla of Vater: prognostic advantage over resection alone? Hepatogastroenterology. 2003;50(52):928–33.
Horgan AM, Amir E, Walter T, Knox JJ. Adjuvant therapy in the treatment of biliary tract cancer: a systematic review and meta-analysis. J Clin Oncol. 2012;30(16):1934–40. https://doi.org/10.1200/JCO.2011.40.5381.
Lim KH, Oh DY, Chie EK, Jang JY, Im SA, Kim TY, et al. Adjuvant concurrent chemoradiation therapy (CCRT) alone versus CCRT followed by adjuvant chemotherapy: which is better in patients with radically resected extrahepatic biliary tract cancer?: a non-randomized, single center study. BMC Cancer. 2009;9:345. https://doi.org/10.1186/1471-2407-9-345.
Kim SW, Noh OK, Kim JH, Chun M, Oh YT, Kang SY, et al. Adjuvant concurrent chemoradiotherapy with low-dose daily cisplatin for extrahepatic bile duct cancer. Cancer Chemother Pharmacol. 2017;79(6):1161–7. https://doi.org/10.1007/s00280-017-3312-y.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declared that they have no conflicts of interest.
Informed consent
For this type of study, formal consent is not required.
Research involving human participants and/or animals
This article does not contain any studies with human participants and/or animals performed by any of authors.
Rights and permissions
About this article
Cite this article
Lee, J., Kang, S.H., Noh, O.K. et al. Adjuvant concurrent chemoradiation therapy in patients with microscopic residual tumor after curative resection for extrahepatic cholangiocarcinoma. Clin Transl Oncol 20, 1011–1017 (2018). https://doi.org/10.1007/s12094-017-1815-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-017-1815-y