Abstract
Objective
The aim of this study was to explore the difference of long-term prognosis of different treatment regimens in patients with stage IB2, IIA2 cervical cancer.
Methods
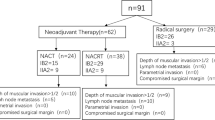
From August 1995 to September 2005, radical hysterectomy was chosen as primary treatment regimen for 122 patients (group A), 85 patients underwent radical hysterectomy after effective neoadjuvant therapy (group B), and 98 patients received surgery after ineffective preoperative therapy (group C). All patients received postoperative therapy.
Results
A total of 305 patients were analyzed. The maximum diameter of tumor was largest in group B, while the pathological risk factors (cervical infiltration, positive surgical margins) were in the lowest proportion. The 5-year mortality rate and relapse rate of group B were the highest, and the overall survival (OS) and progression-free survival (PFS) were the shortest (P < 0.05). No significant difference of long-term survival was found in group C and group A. No difference was found in the surgical of three groups. Large tumor more than 5.5 cm had higher effective ratio of treatment than those 5.5 cm or less. Patients received effective preoperative radiotherapy had better long-term prognosis than those received chemotherapy or radiochemotherapy.
Conclusion
neoadjuvant treatment using for patients with IB2, IIA2 cervical cancer is effective in reducing risk factors of pathological, but it could not improve the long-term survival. The indications of adjuvant therapy after surgery should be reconsidered. Those tumors of diameter 5.5 cm or less response poor to neoadjuvant treatment, and no improvement of survival was found, so direct surgical treatment is suggested for these patients. Radiotherapy is a better choice of preoperative treatment.
Similar content being viewed by others
References
Buda A, Fossati R, Colombo N, et al. Randomized trial of neoadjuvant chemotherapy comparing paclitaxel, ifosfamide, and cisplatin wIth ifosfamide and cisplatin followed by radical surgery in patients with locally advanced squamous cell cervical carcinoma: the SNAP01 (Srudio Neo-Adjuvante Portio) Italian Collaborative Study. J Clin Oncol, 2005, 23: 4137–4145.
Eddy GL, Bundy BN, Creasman WT, et al. Treatment of (“bulky”) stage IB cervical cancer with or without neoadjuvant vincristine and cisplatin prior to radical hysterectomy and pelvic/para-aortic lymphadenectomy: a phase III trial of the gynecologic oncology group. Gynecol Oncol, 2007, 106: 362–369.
Tanaka T, Kokawa K, Umesaki N. Preoperative chemotherapy with irinotecan and mitomycin for FIGO stage IIIB cervical squamous cell carcinoma: a pilot study. Eur J Gynaecol Oncol, 2005, 26: 605–607.
Termrungruanglert W, Tresukosol D, Vasuratna A, et al. Neoadjuvant gemcitabine and cisplatin followed by radical surgery in (bulky) squamous cell carcinoma of cervix stage IB2. Gynecol Oncol, 2005, 97: 576–581.
Neoadjuvant Chemotherapy for Locally Advanced Cervical Cancer Meta-analysis Collaboration. Neoadjuvant chemotherapy for locally advanced cervical cancer: a systematic review and meta-analysis of individual patient data from 21 randomised trials. Eur J Cancer, 2003, 39: 2470–2486.
Dueñas-Gonzalez A, López-Graniel C, González-Enciso A, et al. A phase II study of multimodality treatment for locally advanced cervical cancer: neoadjuvant carboplatin and paclitaxel followed by radical hysterectomy and adjuvant cisplatin chemoradiation. Ann Oncol, 2003, 14: 1278–1284.
Wu Q, Zhang Y. Neoadjuvant intra-arterial infusion chemotherapy followed by surgery in patients with locally advanced cervical cancer. Chinese-German J Clin Oncol, 2009, 8: 537–540.
Choi YS, Sin JI, Kim JH, et al. Survival benefits of neoadjuvant chemotherapy followed by radical surgery versus radiotherapy in locally advanced chemoresistant cervical cancer. J Korean Med Sci, 2006, 21: 683–689.
Cheng XD, Lv WG, Ye F, et al. Evaluation of neoadjyvant chemotherapy for locally advanced cervical cancinoma. Chin J Obstet Gynecol (Chinese), 2006, 41: 95–98.
Lissoni AA, Colombo N, Pellegrino A, et al. A phase II, randomized trial of neo-adjuvant chemotherapy comparing a three-drug combination of paclitaxel, ifosfamide, and cispltin (TIP) versus paclitaxel and cispltin (TP) followed by radical surgery in patients with locally advanced squamous cell cervical carcinoma: the Snap-02 Italian Collaborative Study. Annals of Oncology, 2009, 20: 660–665.
Cho YH, Kim DY, Kim JH, et al. Comparative study of neoadjuvant chemotherapy before radical hysterectomy and radical surgery alone in stage IB2-IIA bulky cervical cancer. J Gynecol Onocol, 2009, 20: 22–27.
Long HJ 3rd, Laack NN, Gostout BS, et al. Gostout. Prevention, diagnosis, and treatment of cervical cancer. Mayo Clin Proc, 2007, 82: 1566–1574.
Btady PC, Chen X, Burke WM, et al. Detection and significance of parametrial micrometastases in early-stage cervical cancer. Anticancer Res, 2011, 31: 243–247
Zand B, Euscher ED, Soliman PT, et al. Rate of para-aortic lymph node micrometastasis in patients with locally advanced cervical cancer. Gynecol Oncol, 2010, 119: 422–425.
Cândido EB, Silva-Filho AL, Triginelli SA, et al. Histopathological and immunohistochemical (cytokeratins AE1/AE3) study of the parametrium of patients with early stage cervical cancer. Eur J Obstet Gynecol Reprod Biol, 2008, 141: 58–63.
Lentz SE, Muderspach LI, Felix JC, et al. Identification of micrometastases in histologically negative lymph nodes of early-stage cervical cancer patients. Obstet Gynecol, 2004, 103: 1204–1210.
Zhong X, Zhong S, Yang L, et al. Combination of subradical external radiation and brachytherapy plus radical operation in the treatment of carcinoma of uterine cervix. Chin J Oncol (Chinese), 2002, 24: 291–293.
Zhong XP, Tong XK, Yang, LF et al. Clinical study on radiotherapy combined with surgical treatment of 162 patients with cervical cancer. Chinese-German J Clin Oncol, 2008, 7: 484–486.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liang, D., Zhang, Y., Sun, X. et al. Comparison of different treatment regimens for IB2 and IIA2 cervical cancer. Chin. -Ger. J. Clin. Oncol. 11, 37–42 (2012). https://doi.org/10.1007/s10330-011-0889-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10330-011-0889-1