Abstract
Objective
To investigate the safety and efficacy of a dose-escalation regimen of trimethoprim–sulfamethoxazole (TMP/SMX) for prophylaxis against Pneumocystis jiroveci pneumonia (PCP) in rheumatic diseases.
Methods
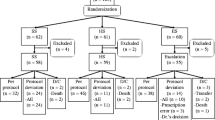
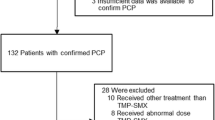
Data from 41 patients, who received glucocorticoids with or without immunosuppressive agents and prophylactic use of TMP/SMX, were retrospectively analyzed. Thirteen patients were started on a daily dose of 10 % of single-strength (SS) TMP/SMX, which was increased gradually (dose-escalation group), while 28 patients were started on 1 SS tablet daily (routine group).
Results
In the dose-escalation group, the retention rate was 100 % at 6 months. In the routine group, 5 patients discontinued TMP/SMX; the retention rate was 82.1 %. Moreover, the retention rate when taking a daily dose of 50 % or more of SS TMP/SMX, or 1 SS tablet thrice-weekly, was significantly higher in the dose-escalation group (100 versus 71.4 %, P = 0.032). No PCP was observed in the dose-escalation group; however, 1 patient in the routine group, who had discontinued TMP/SMX, developed PCP. The rate of adverse effects was less, although nonsignificant, in the dose-escalation group (30.8 versus 46.4 %, P = 0.344).
Conclusions
In rheumatic diseases, a dose-escalation regimen of TMP/SMX resulted in a higher retention rate and was safer than the routine regimen.
Similar content being viewed by others
References
Godeau B, Coutant-Perronne V, Le Thi Huong D, Guillevin L, Magadur G, De Bandt M, et al. Pneumocystis carinii pneumonia in the course of connective tissue disease: report of 34 cases. J Rheumatol. 1994;21:246–51.
Li J, Huang XM, Fang WG, Zeng XJ. Pneumocystis carinii pneumonia in patients with connective tissue disease. J Clin Rheumatol. 2006;12:114–7.
Hugle B, Solomon M, Harvey E, James A, Wadhwa A, Amin R, et al. Pneumocystis jiroveci pneumonia following rituximab treatment in Wegener’s granulomatosis. Arthritis Care Res (Hoboken). 2010;62:1661–4.
Phair J, Munoz A, Detels R, Kaslow R, Rinaldo C, Saah A. The risk of Pneumocystis carinii pneumonia among men infected with human immunodeficiency virus type 1. Multicenter AIDS Cohort Study Group. N Engl J Med. 1990;322:161–5.
Yale SH, Limper AH. Pneumocystis carinii pneumonia in patients without acquired immunodeficiency syndrome: associated illness and prior corticosteroid therapy. Mayo Clin Proc. 1996;71:5–13.
Kulke MH, Vance EA. Pneumocystis carinii pneumonia in patients receiving chemotherapy for breast cancer. Clin Infect Dis. 1997;25:215–8.
Hughes WT, Feldman S, Aur RJ, Verzosa MS, Hustu HO, Simone JV. Intensity of immunosuppressive therapy and the incidence of Pneumocystis carinii pneumonitis. Cancer. 1975;36:2004–9.
Ognibene FP, Shelhamer JH, Hoffman GS, Kerr GS, Reda D, Fauci AS, et al. Pneumocystis carinii pneumonia: a major complication of immunosuppressive therapy in patients with Wegener’s granulomatosis. Am J Respir Crit Care Med. 1995;151:795–9.
Kermani TA, Ytterberg SR, Warrington KJ. Pneumocystis jiroveci pneumonia in giant cell arteritis: a case series. Arthritis Care Res (Hoboken). 2011;63:761–5.
Ward MM, Donald F. Pneumocystis carinii pneumonia in patients with connective tissue diseases: the role of hospital experience in diagnosis and mortality. Arthritis Rheum. 1999;42:780–9.
Tokuda H, Sakai F, Yamada H, Johkoh T, Imamura A, Dohi M, et al. Clinical and radiological features of Pneumocystis pneumonia in patients with rheumatoid arthritis, in comparison with methotrexate pneumonitis and Pneumocystis pneumonia in acquired immunodeficiency syndrome: a multicenter study. Intern Med. 2008;47:915–23.
Monnet X, Vidal-Petiot E, Osman D, Hamzaoui O, Durrbach A, Goujard C, et al. Critical care management and outcome of severe Pneumocystis pneumonia in patients with and without HIV infection. Crit Care. 2008;12:R28.
Enomoto T, Azuma A, Kohno A, Kaneko K, Saito H, Kametaka M, et al. Differences in the clinical characteristics of Pneumocystis jiroveci pneumonia in immunocompromised patients with and without HIV infection. Respirology. 2010;15:126–31.
Green H, Paul M, Vidal L, Leibovici L. Prophylaxis of Pneumocystis pneumonia in immunocompromised non-HIV-infected patients: systematic review and meta-analysis of randomized controlled trials. Mayo Clin Proc. 2007;82:1052–9.
Ogawa J, Harigai M, Nagasaka K, Nakamura T, Miyasaka N. Prediction of and prophylaxis against Pneumocystis pneumonia in patients with connective tissue diseases undergoing medium- or high-dose corticosteroid therapy. Mod Rheumatol. 2005;15:91–6.
Chung JB, Armstrong K, Schwartz JS, Albert D. Cost-effectiveness of prophylaxis against Pneumocystis carinii pneumonia in patients with Wegner’s granulomatosis undergoing immunosuppressive therapy. Arthritis Rheum. 2000;43:1841–8.
Yamazaki H, Nanki T, Miyasaka N, Harigai M. Methotrexate and trimethoprim-sulfamethoxazole for Pneumocystis pneumonia prophylaxis. J Rheumatol 2011;38:777; author reply 778.
Milstone AM, Balakrishnan SL, Foster CB, Chen A. Failure of intravenous pentamidine prophylaxis to prevent pneumocystis pneumonia in a pediatric hematopoietic stem cell transplant (HSCT) patient. Pediatr Blood Cancer. 2006;47:859–60.
Para MF, Finkelstein D, Becker S, Dohn M, Walawander A, Black JR. Reduced toxicity with gradual initiation of trimethoprim–sulfamethoxazole as primary prophylaxis for Pneumocystis carinii pneumonia: AIDS Clinical Trials Group 268. J Acquir Immune Defic Syndr. 2000;24:337–43.
Bozzette SA, Finkelstein DM, Spector SA, Frame P, Powderly WG, He W, et al. A randomized trial of three antipneumocystis agents in patients with advanced human immunodeficiency virus infection. NIAID AIDS Clinical Trials Group. N Engl J Med. 1995;332:693–9.
Komano Y, Harigai M, Koike R, Sugiyama H, Ogawa J, Saito K, et al. Pneumocystis jiroveci pneumonia in patients with rheumatoid arthritis treated with infliximab: a retrospective review and case–control study of 21 patients. Arthritis Rheum. 2009;61:305–12.
Leoung GS, Stanford JF, Giordano MF, Stein A, Torres RA, Giffen CA, et al. Trimethoprim–sulfamethoxazole (TMP–SMZ) dose escalation versus direct rechallenge for Pneumocystis carinii pneumonia prophylaxis in human immunodeficiency virus-infected patients with previous adverse reaction to TMP–SMZ. J Infect Dis. 2001;184:992–7.
Soffritti S, Ricci G, Prete A, Rondelli R, Menna G, Pession A. Successful desensitization to trimethoprim-–sulfamethoxazole after allogeneic haematopoietic stem cell transplantation: preliminary observations. Med Pediatr Oncol. 2003;40:271–2.
Koopmans PP, Burger DM. Managing drug reactions to sulfonamides and other drugs in HIV infection: desensitization rather than rechallenge? Pharm World Sci. 1998;20:253–7.
Caumes E, Guermonprez G, Winter C, Katlama C, Bricaire F. A life-threatening adverse reaction during trimethoprim–sulfamethoxazole desensitization in a previously hypersensitive patient infected with human immunodeficiency virus. Clin Infect Dis. 1996;23:1313–4.
Smith CL, Brown I, Torraca BM. Acetylator status and tolerance of high-dose trimethoprim–sulfamethoxazole therapy among patients infected with human immunodeficiency virus. Clin Infect Dis. 1997;25:1477–8.
Pope J, Jerome D, Fenlon D, Krizova A, Ouimet J. Frequency of adverse drug reactions in patients with systemic lupus erythematosus. J Rheumatol. 2003;30:480–4.
Jeffries M, Bruner G, Glenn S, Sadanandan P, Carson CW, Harley JB, et al. Sulpha allergy in lupus patients: a clinical perspective. Lupus. 2008;17:202–5.
Fisher RG, Nageswaran S, Valentine ME, McKinney RE Jr. Successful prophylaxis against Pneumocystis carinii pneumonia in HIV-infected children using smaller than recommended dosages of trimethoprim–sulfamethoxazole. AIDS Patient Care STDS. 2001;15:263–9.
Acknowledgments
The authors gratefully acknowledge the support of Hiroshi Takayama, Chugai Pharmaceutical Co., Ltd., for statistical advice.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Takenaka, K., Komiya, Y., Ota, M. et al. A dose-escalation regimen of trimethoprim–sulfamethoxazole is tolerable for prophylaxis against Pneumocystis jiroveci pneumonia in rheumatic diseases. Mod Rheumatol 23, 752–758 (2013). https://doi.org/10.1007/s10165-012-0730-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10165-012-0730-x