Abstract
Purpose
Intestinal obstruction is a leading cause of patient mortality and the most common reason for emergent operation in colorectal surgery. The influence of inter-hospital transfer on patients’ outcomes varies greatly in different diseases. We aimed to compare the surgical outcomes and medical costs between transferred and directly admitted patients diagnosed with intestinal obstruction in an American tertiary referral center.
Methods
All intestinal obstruction patients operated in Cleveland Clinic from Jan 2012 to Dec 2016 were collected from a prospectively maintained database. Preoperative characteristics; surgical outcomes, including intraoperative complication, postoperative complication, readmission, reoperation, and postoperative 30-day mortality; and medical cost were collected. All parameters were compared between two groups before and after propensity score match. Multivariate logistic analysis was used to explore risk factors of surgical outcomes.
Results
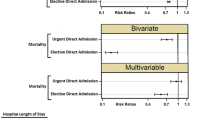
A total of 576 patients were included, with 75 in the transferred group and 501 in the directly admitted group. Before match, the transferred patients had longer waiting interval from admission to surgery (p < 0.001), more contaminated or infected wounds (p = 0.02), different surgical procedures (p = 0.02), and similar surgical outcomes and total medical cost (all p > 0.05), compared with the directly admitted group. Multivariate analysis showed that inter-hospital transfer was not an independent predictor of any surgical outcome. After matching to balance the preoperative characteristics between two groups, no significant differences were identified in all surgical outcomes and total medical cost between two groups (all p > 0.05).
Conclusions
Compared with directly admitted patients, transferred intestinal obstruction patients are associated with similar surgical outcomes and similar medical costs.

Similar content being viewed by others
References
Miller G, Boman J, Shrier I, Gordon PH (2000) Etiology of small bowel obstruction. Am J Surg 180(1):33–36
Hayanga AJ, Bass-Wilkins K, Bulkley GB (2005) Current management of small-bowel obstruction. Adv Surg 39:1–33
Zielinski MD, Bannon MP (2011) Current management of small bowel obstruction. Adv Surg 45:1–29
Catena F, Di Saverio S, Coccolini F, Ansaloni L, De Simone B, Sartelli M, Van Goor H (2016) Adhesive small bowel adhesions obstruction: evolutions in diagnosis, management and prevention. World J Gastrointest Surg 8(3):222–231. https://doi.org/10.4240/wjgs.v8.i3.222
Bizer LS, Liebling RW, Delany HM, Gliedman ML (1981) Small bowel obstruction: the role of nonoperative treatment in simple intestinal obstruction and predictive criteria for strangulation obstruction. Surgery 89(4):407–413
Schraufnagel D, Rajaee S, Millham FH (2013) How many sunsets? Timing of surgery in adhesive small bowel obstruction: a study of the nationwide inpatient sample. J Trauma Acute Care Surg 74(1):181–187; discussion 187-189. https://doi.org/10.1097/TA.0b013e31827891a1
Colonna AL, Byrge NR, Nelson SD, Nelson RE, Hunter MC, Nirula R (2016) Nonoperative management of adhesive small bowel obstruction: what is the break point? Am J Surg 212(6):1214–1221. https://doi.org/10.1016/j.amjsurg.2016.09.037
Teixeira PG, Karamanos E, Talving P, Inaba K, Lam L, Demetriades D (2013) Early operation is associated with a survival benefit for patients with adhesive bowel obstruction. Ann Surg 258(3):459–465. https://doi.org/10.1097/SLA.0b013e3182a1b100
Malangoni MA, Times ML, Kozik D, Merlino JI (2001) Admitting service influences the outcomes of patients with small bowel obstruction. Surgery 130(4):706–711; discussion 711-703. https://doi.org/10.1067/msy.2001.116918
Garwe T, Cowan LD, Neas B, Cathey T, Danford BC, Greenawalt P (2010) Survival benefit of transfer to tertiary trauma centers for major trauma patients initially presenting to nontertiary trauma centers. Acad Emerg Med Off J Soc Acad Emerg Med 17(11):1223–1232. https://doi.org/10.1111/j.1553-2712.2010.00918.x
Cassidy TJ, Edgar DW, Phillips M, Cameron P, Cleland H, Wood FM, Steering Committee of the ABRoA, New Z (2015) Transfer time to a specialist burn service and influence on burn mortality in Australia and New Zealand: a multi-centre, hospital based retrospective cohort study. Burns 41(4):735–741. https://doi.org/10.1016/j.burns.2015.01.016
Ilonzo N, Egorova NN, Nowygrod R (2016) Interhospital transfer for intact abdominal aortic aneurysm repair. J Vasc Surg 63(4):859–865. https://doi.org/10.1016/j.jvs.2015.10.068
Mell MW, Wang NE, Morrison DE, Hernandez-Boussard T (2014) Interfacility transfer and mortality for patients with ruptured abdominal aortic aneurysm. J Vasc Surg 60(3):553–557. https://doi.org/10.1016/j.jvs.2014.02.061
Rosenberg AL, Hofer TP, Strachan C, Watts CM, Hayward RA (2003) Accepting critically ill transfer patients: adverse effect on a referral center's outcome and benchmark measures. Ann Intern Med 138(11):882–890
Gordon HS, Rosenthal GE (1996) Impact of interhospital transfers on outcomes in an academic medical center. Implications for profiling hospital quality. Med Care 34(4):295–309
Sheridan R, Weber J, Prelack K, Petras L, Lydon M, Tompkins R (1999) Early burn center transfer shortens the length of hospitalization and reduces complications in children with serious burn injuries. J Burn Care Rehab 20(5):347–350
Alberts MJ, Wechsler LR, Jensen ME, Latchaw RE, Crocco TJ, George MG, Baranski J, Bass RR, Ruff RL, Huang J, Mancini B, Gregory T, Gress D, Emr M, Warren M, Walker MD (2013) Formation and function of acute stroke-ready hospitals within a stroke system of care recommendations from the brain attack coalition. Stroke 44(12):3382–3393. https://doi.org/10.1161/STROKEAHA.113.002285
Holmes JH (2008) Critical issues in burn care. J Burn Care Res 29(6 Suppl 2):S180–S187. https://doi.org/10.1097/BCR.0b013e31818cf8b8
Chow CJ, Gaertner WB, Jensen CC, Sklow B, Madoff RD, Kwaan MR (2017) Does hospital transfer impact outcomes after colorectal surgery? Dis Colon Rectum 60(2):194–201. https://doi.org/10.1097/DCR.0000000000000765
Rosenbaum BP, Lorenz RR, Luther RB, Knowles-Ward L, Kelly DL, Weil RJ (2014) Improving and measuring inpatient documentation of medical care within the MS-DRG system: education, monitoring, and normalized case mix index. Perspect Health Inf Manag 11:1c
Kulshrestha A, Singh J (2016) Inter-hospital and intra-hospital patient transfer: recent concepts. Indian J Anaesth 60(7):451–457. https://doi.org/10.4103/0019-5049.186012
Farto e Abreu P, Thomas B, Loureiro J, Roquette J, Ferreira R (2002) Inter-hospital transfer of critically-ill patients for urgent cardiac surgery after placement of an intra-aortic balloon pump. Rev Port Cardiol 21(10):1115–1123
Lucas DJ, Ejaz A, Haut ER, Spolverato G, Haider AH, Pawlik TM (2014) Interhospital transfer and adverse outcomes after general surgery: implications for pay for performance. J Am Coll Surg 218(3):393–400. https://doi.org/10.1016/j.jamcollsurg.2013.11.024
Seror D, Feigin E, Szold A, Allweis TM, Carmon M, Nissan S, Freund HR (1993) How conservatively can postoperative small bowel obstruction be treated? Am J Surg 165(1):121–125
Bickell NA, Federman AD, Aufses AH Jr (2005) Influence of time on risk of bowel resection in complete small bowel obstruction. J Am Coll Surg 201(6):847–854. https://doi.org/10.1016/j.jamcollsurg.2005.07.005
Kothari AN, Liles JL, Holmes CJ, Zapf MA, Blackwell RH, Kliethermes S, Kuo PC, Luchette FA (2015) “Right place at the right time” impacts outcomes for acute intestinal obstruction. Surgery 158(4):1116–1125. https://doi.org/10.1016/j.surg.2015.06.032
Funding
This study is funded in part by grants from the National Natural Science Foundation of China (#81572332).
Author information
Authors and Affiliations
Contributions
Xian Hua Gao: data gathering and entry, statistical analysis, and manuscript preparation; Hanumant Chouhan: data gathering and manuscript preparation; Emre Gorgun and Luca Stocchi: critical review of manuscript; Gokhan Ozuner: concept, general supervision, and manuscript revisions.
Corresponding author
Ethics declarations
This study was approved by the Institutional Review Board of Cleveland Clinic.
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Gao, X.H., Chouhan, H., Gorgun, E. et al. Comparisons of the surgical outcomes and medical costs between transferred and directly admitted patients diagnosed with intestinal obstruction in an American tertiary referral center. Int J Colorectal Dis 33, 1617–1625 (2018). https://doi.org/10.1007/s00384-018-3052-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-018-3052-4