Abstract
Purpose
To correlate prostate-specific antigen (PSA), free to total PSA percentage (fPSA%) and prostatic acid phosphatase (PAP) levels from peripheral and pelvic venous samples with prostatectomy specimens in patients with prostate adenocarcinoma and borderline elevation of PSA.
Materials and Methods
In this prospective institutional review board approved study, 7 patients with biopsy proven prostate cancer had a venous sampling procedure prior to prostatectomy (mean 3.2 days, range 1–7). Venous samples were taken from a peripheral vein (PVS), the right internal iliac vein, a deep right internal iliac vein branch, left internal iliac vein and a deep left internal iliac vein branch. Venous sampling results were compared to tumour volume, laterality, stage and grade in prostatectomy surgical specimens.
Results
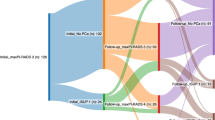
Mean PVS PSA was 4.29, range 2.3–6 ng/ml. PSA and PAP values in PVS did not differ significantly from internal iliac or deep internal iliac vein samples (p > 0.05). fPSA% was significantly higher in internal iliac (p = 0.004) and deep internal iliac (p = 0.003) vein samples compared to PVS. One of 7 patients had unilateral tumour only. This patient, with left–sided tumour, had a fPSA% of 6, 6, 6, 14 and 12 in his peripheral, right internal iliac, deep right internal iliac branch, left internal iliac and deep left internal iliac branch samples respectively. There were no adverse events.
Conclusion
fPSA%, unlike total PSA or PAP, is significantly higher in pelvic vein compared to peripheral vein samples when prostate cancer is present. Larger studies including patients with higher PSA values are warranted to further investigate this counterintuitive finding.

Similar content being viewed by others
References
Jemal A, Siegel R, Ward E, et al. Cancer statistics. CA Cancer J Clin. 2008;58(2):71–96.
Carrol PR. Early stage prostate cancer-do we have a problem with over-detection, overtreatment or both? J Urol. 2005;173(4):1061–2.
Mouraviev V, Mayes JM, Madden JF, Sun L, Polascik TJ. Analysis of laterality and percentage of tumor involvement in 1386 prostatectomized specimens for selection of unilateral focal cryotherapy. Tech Cancer Res Treat. 2007;6(2):91–6.
Djavan B, Susani M, Bursa B, Basharkhah A, Simak R, Marberger M. Predictability and significance of multifocal cancer in the radical prostatectomy specimen. Techn Urol. 1999;5(3):139–42.
Polascik TJ, Mayers JM, Sun L, Madden JF, Moul JW, Mouraviev V. Pathologic stage 2a and 2b prostate cancer in the recent prostate-specific antigen era: implications for unilateral ablative therapy. Prostate. 2008;68(13):1380–6.
Turpen R, Rosser CJ. Focal therapy for prostate cancer: revolution or evolution? BMC Urol. 2009;9:2.
Polascik TJ, Mouraviev V. Focal therapy for prostate cancer is a reasonable treatment option in properly selected patients. Urology. 2009;74(4):726–30.
Eggener SE, Scardino PT, Carroll PR, Zelefsky MJ, Sartor O, Hricak H, for the International task force on prostate cancer and the focal lesion paradigm, et al. Focal therapy for localized prostate cancer: a critical appraisal of rationale and modalities. J Urol. 2007;178(6):2260–7.
Scardino PT, Abenhaim LL. Focal therapy for prostate cancer: analysis by an international panel. Urology. 2008;72(6 Suppl):S1–2.
Mendez MH, Joh DY, Gupta R, Polascik TJ. Current trends and new frontiers in focal therapy for localized prostate cancer. Curr Urol Rep. 2015;16(6):35.
Fitzpatrick JM. PSA measurement in the treatment of BPH. BJU Int. 2004;93(1 Suppl):2–4.
Wendell-Smith C. Terminology of the prostate and related structures. Clin Anat. 2000;13(3):207–13.
Catalona WJ, Partin AW, Slawin KM, Brawer MK, Flanigan RC, Patel A, et al. Use of the percentage of free prostate-specific antigen to enhance differentiation of prostate cancer from benign prostatic diseases. JAMA. 1998;279(19):1542–7.
Djavan B, Remzi M, Zlotta AR, Ravery V, Hammerer P, Reissigl A, et al. Complexed prostate-specific antigen, complexed prostate-specific antigen density of total and transition zone, complexed/total prostate-specific antigen ratio, free-to-total prostate-specific antigen ratio, density of total and transition zone prostate-specific antigen: results of the prospective multicenter European trial. Urology. 2002;60(4 Suppl 1):4–9.
Puppo P. Repeated negative prostate biopsies with persistently elevated or rising PSA: a modern urologic dilemma. Eur Urol. 2007;52(3):639–41.
Jones JS. Management of rising prostate-specific antigen following a negative biopsy. Curr Opin Urol. 2010;20(3):198–203.
Trock BJ. Circulating biomarkers for discriminating indolent from aggressive disease in prostate cancer active surveillance. Curr Opin Urol. 2014;24(3):293–302.
Whitesel JA, Donohue RE, Mani JH, Mohr S, Scanavino DJ, Augspurger RR, et al. Acid phosphatase: its influence on the management of carcinoma of the prostate. J Urol. 1984;131(1):70–2.
Andriole GL, Crawford ED, Grubb RL 3rd, Buys SS, Chia D, Church TR, et al. Prostate cancer screening in the randomized prostate, lung, colorectal, and ovarian cancer screening trial: mortality results after 13 years of follow-up. J Natl Cancer Inst. 2012;104(2):125–32.
Schröder FH, Hugosson J, Roobol MJ, Tammela TL, Zappa M, Nelen V, et al. Screening and prostate cancer mortality: results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet. 2014;384(9959):2027–35.
Pinsky PF, Parnes HL, Andriole G. Mortality and complications after prostate biopsy in the prostate, lung, colorectal and ovarian cancer screening (PLCO) trial. BJU Int. 2014;113(2):254–9.
Anastasiadis E, van der Meulen J, Emberton M. Hospital admissions after transrectal ultrasound-guided biopsy of the prostate in men diagnosed with prostate cancer: a database analysis in England. Int J Urol. 2015;22(2):181–6.
Carrol PR. Early stage prostate cancer-do we have a problem with over-detection, overtreatment or both? J Urol. 2005;173(4):1061–2.
Ward JF, Pisters LL. Considerations for patient selection for focal therapy. Ther Adv Urol. 2013;5(6):330–7.
Lau JH, Drake W, Matson M. The current role of venous sampling in the localization of endocrine disease. Cardiovasc Intervent Radiol. 2007;30(4):555–70.
Young W, Stanson A, Thompson G, et al. Role for adrenal venous sampling in primary aldosteronism. Surgery. 2004;136(6):1227–35.
Ginsburg M, Christoforidis GA, Zivin SP, Obara P, Wroblewski K, Angelos P, et al. Adenoma localization for recurrent or persistent primary hyperparathyroidism using dynamic four-dimensional CT and venous sampling. J Vasc Interv Radiol. 2015;26(1):79–86.
Kaltsas G, Mukherjee J, Kola B, Isidori AM, Hanson JA, Dacie JE, et al. Is ovarian and adrenal venous catheterization and sampling helpful in the investigation of hyperandrogenic women? Clin Endocrinol. 2003;59(1):34–43.
Agarwal MD, Trerotola SO. Combined adrenal and ovarian venous sampling to localize an androgen producing tumor. Cardiovasc Intervent Radiol. 2010;33(6):1266–9.
Lilja H. Biology of prostate-specific antigen. Urology. 2003;62(5 Suppl 1):27–33.
Greene KL, Albertsen PC, Babaian RJ, Carter HB, Gann PH, Han M, et al. Prostate specific antigen best practice statement: 2009 update. J Urol. 2013;189(1 Suppl):2–11.
Batson OV. The function of the vertebral veins and their role in the spread of metastases. Ann Surg. 1940;112(1):138–49.
Batson OV. The vertebral vein system: Caldwell Lecture, 1956. Am J Roentgenol Radium Ther Nucl Med. 1957;78(2):195–212.
Suzuki T, Kurokawa K, Jimbo H, Hayashi M, Sekihara T, Takahashi H, et al. The role of intraabdominal pressure in venous blood drainage from the prostate into the vertebral vein system. Jpn J Physiol. 1993;43(5):697–708.
Franks LM. The spread of prostatic carcinoma to the bones. J Pathol Bacteriol. 1953;66:91–3.
McCormack RT, Rittenhouse HG, Finlay JA, Sokoloff RL, Wang TJ, Wolfert RL, et al. Molecular forms of prostate-specific antigen and the human kallikrein gene family: a new era. Urology. 1995;45(5):729–44.
Catalona WJ, Partin AW, Slawin KM, Brawer MK, Flanigan RC, Patel A, et al. Use of the percentage of free prostate-specific antigen to enhance differentiation of prostate cancer from benign prostatic diseases. JAMA. 1998;279(19):1542–7.
Richardson TD, Wojno KJ, Liang LW, Giacherio DA, England BG, Henricks WH, et al. Half-life determination of serum free prostate-specific antigen following radical retropubic prostatectomy. Urology. 1996;48(6A Suppl):40–4.
Turkbey B, Albert PS, Kurdziel K, Choyke PL. Imaging localized prostate cancer: current approaches and new developments. AJR. 2009;192(6):1471–80.
Hamoen EH, de Rooij M, Witjes JA, Barentsz JO, Rovers MM. Use of the prostate imaging reporting and data system (PI-RADS) for prostate cancer detection with multiparametric magnetic resonance imaging: a diagnostic meta-analysis. Eur Urol. 2015;67(6):1112–21.
Blomqvist L, Carlsson S, Gjertsson P, Heintz E, Hultcrantz M, Mejare I, et al. Limited evidence for the use of imaging to detect prostate cancer: a systematic review. Eur J Radiol. 2014;83(9):1601–6.
Schoots IG, Petrides N, Giganti F, Bokhorst LP, Rannikko A, Klotz L, et al. Magnetic resonance imaging in active surveillance of prostate cancer: a systematic review. Eur Urol. 2015;67(4):627–36.
Ross AE, D’Amico AV, Freedland SJ. Which, when and why? Rational use of tissue-based molecular testing in localized prostate cancer. Prostate Cancer Prostatic Dis. 2015. doi:10.1038/pcan.2015.31.
Falzarano SM, Ferro M, Bollito E, Klein EA, Carrieri G, Magi-Galluzzi C. Novel biomarkers and genomic tests in prostate cancer: a critical analysis. Minerva Urol Nefrol. 2015;67(3):211–31.
Acknowledgments
Grant Support: Study supported with a seed Research Grant: F. Hoffmann- La Roche Ltd. (Roche Diagnostics). 15,000 US Dollar Grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
This study was funded by a 15,000 US Dollar seed research grant from Roche diagnostics: F. Hoffmann- La Roche Ltd. Author A declares no other potential conflict of interest. Authors Priti Lal, Micah M. Watts, Catherine Mc Gorrian and Thomas J. Guzzo declare that they have no conflicts of interest. Author Scott O. Trerotola declares grants from Vascular Pathways, personal fees from Bard Peripheral Vascular, personal fees from Orbimed, personal fees from Teleflex, personal fees from Cook, personal fees from WL Gore, personal fees from Lutonix and personal fees from Medcomp. These are all outside the submitted work, and there is no conflict of interest. Author Gregory J. Nadolski declares grants from Guerbet, LLC. This is outside the submitted work, and there is no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Farrelly, C., Lal, P., Trerotola, S.O. et al. Correlation of Peripheral Vein Tumour Marker Levels, Internal Iliac Vein Tumour Marker Levels and Radical Prostatectomy Specimens in Patients with Prostate Cancer and Borderline High Prostate-Specific Antigen: A Pilot Study. Cardiovasc Intervent Radiol 39, 724–731 (2016). https://doi.org/10.1007/s00270-016-1322-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-016-1322-5