Abstract
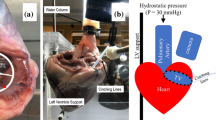
Annulus tension (AT) is defined as leaflet tension per unit length of the annulus circumference. AT was investigated to understand tricuspid valve (TV) annulus mechanics. Ten porcine TVs were mounted on a right ventricle rig with an annulus plate to simulate TV closure. The TVs were mounted on the annulus plate in a normal and dilated TV annulus sizes, and closed under transvalvular pressure of 40 mmHg with the annulus held peripherally by wires. Anterior papillary muscle (PM) and septal PM were displaced in the dilated annulus. Wire forces were measured, and ATs (N/m) were calculated. Clover repair was performed in the dilated TV state subsequently, and AT was calculated again. A one-way ANOVA and Tukey’s HSD test were used to test significances between the different TV states along each annulus segment with p < 0.05. Average ATs for the normal annulus, dilated annulus, and clover repair were 10.75 ± 1.87, 28.81 ± 10.51, and 26.93 ± 11.44 N/m, respectively. Septal annulus segments had the highest ATs when compared to the other segments. For the clover repair, there were no significant changes in AT values. ATs and leaflet forces increased roughly 3–4 times with annulus dilation. AT decelerates annulus dilation as previously shown in the mitral valve. Clover repair does not prevent further annulus dilation by AT change and should be accompanied by annuloplasty. AT improves annulus contraction during a cardiac cycle and should be considered when designing annuloplasty in the future.











Similar content being viewed by others
References
Bhattacharya, S., and Z. He. Role of annulus tension in annular dilatation. J. Heart Valve Dis. 18(5):481–487, 2009.
Bhattacharya, S., and Z. He. Annulus tension of the prolapsed mitral valve corrected by edge-to-edge repair. J. Biomech. 45(3):562–568, 2012. doi:10.1016/j.jbiomech.2011.11.005.
Bhattacharya, S., T. Pham, Z. He, and W. Sun. Tension to passively cinch the mitral annulus through coronary sinus access: an ex vivo study in ovine model. J. Biomech. 47(6):1382–1388, 2014. doi:10.1016/j.jbiomech.2014.01.044.
Castedo, E., A. Canas, R. A. Cabo, R. Burgos, and J. Ugarte. Edge-to-edge tricuspid repair for redeveloped valve incompetence after DeVega’s annuloplasty. Ann. Thorac. Surg. 75(2):605–606, 2003.
De Bonis, M., E. Lapenna, G. La Canna, A. Grimaldi, F. Maisano, L. Torracca, et al. A novel technique for correction of severe tricuspid valve regurgitation due to complex lesions. Eur. J. Cardio Thorac. Surg. 25(5):760–765, 2004. doi:10.1016/j.ejcts.2004.01.051.
Fawzy, H., K. Fukamachi, C. D. Mazer, A. Harrington, D. Latter, D. Bonneau, et al. Complete mapping of the tricuspid valve apparatus using three-dimensional sonomicrometry. J. Thorac. Cardiovasc. Surg. 141(4):1037–1043, 2011. doi:10.1016/j.jtcvs.2010.05.039.
Fukuda, S., G. Saracino, Y. Matsumura, M. Daimon, H. Tran, N. L. Greenberg, et al. Three-dimensional geometry of the tricuspid annulus in healthy subjects and in patients with functional tricuspid regurgitation: a real-time, 3-dimensional echocardiographic study. Circulation 114(1 Suppl):I492–I498, 2006. doi:10.1161/CIRCULATIONAHA.105.000257.
He, Z., and S. Bhattacharya. Papillary muscle and annulus size effect on anterior and posterior annulus tension of the mitral valve: an insight into annulus dilatation. J. Biomech. 41(11):2524–2532, 2008. doi:10.1016/j.jbiomech.2008.05.006.
He, Z., and S. Bhattacharya. Mitral valve annulus tension and the mechanism of annular dilation: an in vitro study. J. Heart Valve Dis. 19(6):701–707, 2010.
Hiro, M. E., J. Jouan, M. R. Pagel, E. Lansac, K. H. Lim, H. S. Lim, et al. Sonometric study of the normal tricuspid valve annulus in sheep. J. Heart Valve Dis. 13(3):452–460, 2004.
Hung, J. The pathogenesis of functional tricuspid regurgitation. Semin. Thorac. Cardiovasc. Surg. 22(1):76–78, 2010. doi:10.1053/j.semtcvs.2010.05.004.
Kotoulas, C., R. P. Jones, W. Turkie, and R. Hasan. Edge-to-edge repair of tricuspid valve in a corrected transposition of the great vessels. Hellenic J. Cardiol. 49(6):434–436, 2008.
Kragsnaes, E. S., J. L. Honge, J. B. Askov, J. M. Hasenkam, H. Nygaard, S. L. Nielsen, et al. In-plane tricuspid valve force measurements: development of a strain gauge instrumented annuloplasty ring. Cardiovasc. Eng. Technol. 4(2):131–138, 2013. doi:10.1007/s13239-013-0135-9.
Lapenna, E., M. De Bonis, A. Verzini, G. La Canna, D. Ferrara, M. C. Calabrese, et al. The clover technique for the treatment of complex tricuspid valve insufficiency: midterm clinical and echocardiographic results in 66 patients. Eur. J. Cardio Thorac. Surg. 37(6):1297–1303, 2010. doi:10.1016/j.ejcts.2009.12.020.
Mahmood, F., H. Kim, B. Chaudary, R. Bergman, R. Matyal, J. Gerstle, et al. Tricuspid annular geometry: a three-dimensional transesophageal echocardiographic study. J. Cardiothorac. Vasc. Anesth. 27(4):639–646, 2013. doi:10.1053/j.jvca.2012.12.014.
Ring, L., B. S. Rana, A. Kydd, J. Boyd, K. Parker, and R. A. Rusk. Dynamics of the tricuspid valve annulus in normal and dilated right hearts: a three-dimensional transoesophageal echocardiography study. Eur. Heart J. Cardiovasc. Imaging 13(9):756–762, 2012. doi:10.1093/ehjci/jes040.
Rogers, J. H., and S. F. Bolling. The tricuspid valve: current perspective and evolving management of tricuspidregurgitation. Circulation 119(20):2718–2725, 2009. doi:10.1161/CIRCULATIONAHA.108.842773.
Siefert, A. W., J. H. Jimenez, K. J. Koomalsingh, F. Aguel, D. S. West, T. Shuto, et al. Contractile mitral annular forces are reduced with ischemic mitral regurgitation. J. Thorac. Cardiovasc. Surg. 146(2):422–428, 2013. doi:10.1016/j.jtcvs.2012.10.006.
Siefert, A. W., J. H. Jimenez, D. S. West, K. J. Koomalsingh, R. C. Gorman, J. H. Gorman, 3rd, et al. In-vivo transducer to measure dynamic mitral annular forces. J. Biomech. 45(8):1514–1516, 2012. doi:10.1016/j.jbiomech.2012.03.009.
Siefert, A. W., E. L. Pierce, M. Lee, M. O. Jensen, C. Aoki, S. Takebayashi, et al. Suture forces in undersized mitral annuloplasty: novel device and measurements. Ann. Thorac. Surg. 98(1):305–309, 2014. doi:10.1016/j.athoracsur.2014.02.036.
Silver, M. D., J. H. Lam, N. Ranganathan, and E. D. Wigle. Morphology of the human tricuspid valve. Circulation 43(3):333–348, 1971.
Simonneau, G., N. Galie, L. J. Rubin, D. Langleben, W. Seeger, G. Domenighetti, et al. Clinical classification of pulmonary hypertension. J. Am. Coll. Cardiol. 43(12 Suppl S):5S–12S, 2004. doi:10.1016/j.jacc.2004.02.037.
Simonneau, G., M. A. Gatzoulis, I. Adatia, D. Celermajer, C. Denton, A. Ghofrani, et al. Updated clinical classification of pulmonary hypertension. J. Am. Coll. Cardiol. 62(25 Suppl):D34–D41, 2013. doi:10.1016/j.jacc.2013.10.029.
Spinner, E. M., D. Buice, C. H. Yap, and A. P. Yoganathan. The effects of a three-dimensional, saddle-shaped annulus on anterior and posterior leaflet stretch and regurgitation of the tricuspid valve. Ann. Biomed. Eng. 40(5):996–1005, 2012. doi:10.1007/s10439-011-0471-6.
Spinner, E. M., S. Lerakis, J. Higginson, M. Pernetz, S. Howell, E. Veledar, et al. Correlates of tricuspid regurgitation as determined by 3D echocardiography: pulmonary arterial pressure, ventricle geometry, annular dilatation, and papillary muscle displacement. Circ. Cardiovasc. Imaging. 5(1):43–50, 2012. doi:10.1161/CIRCIMAGING.111.965707.
Spinner, E. M., P. Shannon, D. Buice, J. H. Jimenez, E. Veledar, P. J. Del Nido, et al. In vitro characterization of the mechanisms responsible for functional tricuspid regurgitation. Circulation 124(8):920–929, 2011. doi:10.1161/CIRCULATIONAHA.110.003897.
Spinner, E. M., K. Sundareswaran, L. P. Dasi, V. H. Thourani, J. Oshinski, and A. P. Yoganathan. Altered right ventricular papillary muscle position and orientation in patients with a dilated left ventricle. J. Thorac. Cardiovasc. Surg. 141(3):744–749, 2011. doi:10.1016/j.jtcvs.2010.05.034.
Ton-Nu, T. T., R. A. Levine, M. D. Handschumacher, D. J. Dorer, C. Yosefy, D. Fan, et al. Geometric determinants of functional tricuspid regurgitation: insights from 3-dimensional echocardiography. Circulation 114(2):143–149, 2006. doi:10.1161/CIRCULATIONAHA.106.611889.
Vakil, K., H. Roukoz, M. Sarraf, B. Krishnan, M. Reisman, W. C. Levy, et al. Safety and efficacy of the MitraClip(R) system for severe mitral regurgitation: a systematic review. Catheter. Cardiovasc. Interv. 84(1):129–136, 2014. doi:10.1002/ccd.25347.
Wan, B., M. Rahnavardi, D. H. Tian, K. Phan, S. Munkholm-Larsen, P. G. Bannon, et al. A meta-analysis of MitraClip system versus surgery for treatment of severe mitral regurgitation. Ann. Cardiothorac. Surg. 2(6):683–692, 2013. doi:10.3978/j.issn.2225-319X.2013.11.02.
Acknowledgements
The pig hearts were donated by the Klemke Sausage Haus in Slaton, Texas, USA. The authors would like to thank the ARCS Foundation for their generous support. The authors would also like to thank Philip Henry for providing assistance with construction of the normal and dilated annulus plates.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Ajit P. Yoganathan oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Basu, A., He, Z. Annulus Tension on the Tricuspid Valve: An In-Vitro Study. Cardiovasc Eng Tech 7, 270–279 (2016). https://doi.org/10.1007/s13239-016-0267-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-016-0267-9