Abstract
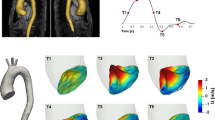
Little is known of the likely changes in blood flow velocity profiles and aortic wall shear stress (WSS) following transcatheter aortic valve implantation (TAVI). The objective of this study was to investigate the effects of TAVI on flow patterns in the thoracic aorta by using cardiovascular magnetic resonance imaging (CMR) and computational fluid dynamics (CFD). An elderly patient with aortic stenosis was examined using MRI pre- and post-TAVI, and CFD simulations were carried out incorporating MRI-derived patient-specific anatomy and upstream flow conditions. Pre-TAVI velocity profiles demonstrated the highly disturbed turbulent flow and jet impacting the wall of the arch owing to the partial opening of the stenosed aortic valve, with likely pathological effects. In the Post-TAVI aorta, velocity profiles were similar to those of healthy aortas with spatially more uniform WSS and lower turbulence levels, demonstrating the favourable effects of the TAVI procedure in restoring normal aortic flow. This study has shown both the effectiveness of TAVI on an individual patient and the advantage of the combined CMR and CFD method for a comprehensive patient-specific assessment of pre- and post-TAVI aortic flow patterns and WSS over CMR alone.










Similar content being viewed by others
References
Bluestein, D., and S. Einav. Transition to turbulence in pulsatile flow through heart valves—a modified stability approach. ASME J. Biomech. Eng. 116:477–497, 1994.
Bluestein, D., Y. M. Li, and I. B. Krukenkamp. Free emboli formation in the wake of bi-leaflet mechanical heart valves and the effects of implantation techniques. J. Biomech. 35:1533–1540, 2002.
Bluestein, D., E. Rambod, and M. Gharib. Vortex shedding as a mechanism for free emboli formation in mechanical heart valves. ASME J. Biomech. Eng. 122:125–134, 2000.
Bogren, H. G., and M. Buonocore. 4D magnetic resonance velocity mapping of blood flow patterns in the aorta in young vs elderly normal subjects. J. Magn. Reson. Imaging 10:861–869, 1999.
Bonow, R. O., B. A. Carabello, C. Kanu, A. C. de Leon, D. P. Faxon, M. D. Freed, W. H. Gaasch, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association task force on practice guidelines (writing committee to revise the 1998 guidelines for the management of patients with valvular heart disease): developed in collaboration with the society of cardiovascular anesthesiologists: endorsed by the society for cardiovascular angiography and interventions and the society of thoracic surgeons. Circulation 114:84–231, 2006.
Cheng, R., Y. G. Lai, and K. B. Chandran. Three-dimensional fluid–structure interaction simulation of bileaflet mechanical heart valve flow dynamics. Ann. Biomed. Eng. 32:1471–1483, 2004.
Cribier, A., H. Eltchaninoff, A. Bash, N. Borenstein, C. Tron, F. Bauer, G. Derumeaux, et al. Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis: first human case description. Circulation 106:3006–3008, 2002.
de Hart, J., G. W. M. Peters, P. J. G. Schreurs, and F. P. T. Baaijens. A two dimensional fluid–structure interaction model of the aortic valve. J. Biomech. 33:1079–1088, 2000.
de Hart, J., G. W. M. Peters, P. J. G. Schreurs, and F. P. T. Baaijens. A three dimensional computational analysis of fluid–structure interaction in the aortic valve. J. Biomech. 36:103–112, 2003.
Dumont, K., J. Vierendeels, R. Kaminsky, G. van Nooten, P. Verdonck, and D. Bluestein. Comparison of the hemodynamic and thrombogenic performance of two bileaflet mechanical heart valves using a CFD/FSI model. ASME J. Biomech. Eng. 129:558–565, 2007.
Dwyer, H. A., P. B. Matthews, A. Azadani, N. Jaussaud, L. Ge, T. S. Guy, and E. E. Tseng. Computational fluid dynamics simulation of transcatheter aortic valve degeneration. Interact. Cardiovasc. Thorac. Surg. 9:301–308, 2009.
Elefteriades, J. A. Thoracic aortic aneurysm: reading the enemy’s playbook. Curr. Probl. Cardiol. 33:203–277, 2008.
El-Hamamsy, I., and M. H. Yacoub. Cellular and molecular mechanisms of thoracic aortic aneurysms. Nat. Rev. Cardiol. 6:771–786, 2009.
Frydrychowicz, A., A. F. Stalder, M. F. Russe, J. Bock, S. Bauer, A. Harloff, A. Berger, M. Langer, J. Hennig, and M. Markl. Three-dimensional analysis of segmental wall shear stress in the aorta by flow-sensitive four-dimensional-MRI. J. Magn. Reson. Imaging 30:77–84, 2009.
Ge, L., L. P. Dasi, F. Sotiropoulos, and A. P. Yoganathan. Characterization of hemodynamic forces induced by mechanical heart valves: Reynolds vs viscous stresses. Ann. Biomed. Eng. 36:276–297, 2008.
Gonzales, R. C., and R. E. Woods. Digital Image Processing. Upper Saddle River: Prentice-Hall Inc., 2002.
Hope, T. A., M. Markl, L. Wingstrom, M. T. Alley, D. C. Miller, and R. J. Herfkens. Comparison of flow patterns in ascending aortic aneurysms and volunteers using four-dimensional magnetic resonance velocity mapping. J. Magn. Reson. Imaging 26:1471–1479, 2007.
Huang, Z. J., C. L. Merkle, S. Abdallah, and J. M. Tarbell. Numerical simulation of unsteady laminar flow through a tilting disk heart valve: prediction of vortex shedding. J. Biomech. 27:391–402, 1994.
Hutchinson, B. R., and G. D. Raithby. A multigrid method based on the additive correction strategy. Numer. Heat Transfer. 9:511–537, 1986.
Kilner, P. J., G. Z. Yang, R. H. Mohiaddin, D. N. Firmin, and D. B. Longmore. Helical and retrograde secondary flow patterns in the aortic arch studied by three-directional magnetic resonance velocity mapping. Circulation 88:2235–2247, 1993.
Lai, Y. G., K. B. Chandran, and J. Lemmon. A numerical simulation of mechanical heart valve closure fluid dynamics. J. Biomech. 35:881–892, 2002.
Malek, A. M., S. L. Alper, and S. Izumo. Hemodynamic shear stress and its role in atherosclerosis. JAMA. 282:2035–2042, 1999.
Menter, F., R. Langtry, and S. Volker. Transition modelling for general purpose CFD codes. Flow Turbul. Combust. 77:277–303, 2006.
Morbiducci, U., R. Ponzini, G. Rizzo, M. Cadioli, A. Esposito, F. Cobelli, A. Maschio, et al. In vivo quantification of helical blood flow in human aorta by time-resolved three-dimensional cine phase contrast magnetic resonance imaging. Ann. Biomed. Eng. 37:516–531, 2009.
Nerem, R. M., W. A. Seed, and N. B. Wood. An experimental study of the velocity distribution and transition to turbulence in the aorta. J. Fluid Mech. 52:137–160, 1972.
Nkomo, V. T., J. M. Gardin, T. N. Skelton, J. S. Gottdiener, C. G. Scott, and M. Enriquez-Sarano. Burden of valvular heart diseases: a population-based study. Lancet 368:1005–1011, 2006.
Nobili, M., U. Morbiducci, R. Ponzini, C. D. Gaudio, A. Balducci, M. Grigioni, F. M. Montevecchi, and A. Redaelli. Numerical simulation of the dynamics of a bileaflet prosthetic heart valve using a fluid-structure interaction approach. J. Biomech. 41:2539–2550, 2008.
Parker, K. H. Instability in arterial blood flow. In: Cardiovascular Flow Dynamics and Measurements, edited by N. H. C. Hwang, and N. A. Normann. Baltimore: University Park Press, 1977, pp. 633–663.
Peskin, C. S., and D. M. McQueen. Modeling prosthetic heart valves for numerical analysis of blood flow through the heart. J. Comput. Phys. 37:113–132, 1994.
Stein, P. D., and H. N. Sabbah. Turbulent blood flow in the ascending aorta of humans with normal and diseased aortic valves. Circ. Res. 39:58–65, 1976.
Sun, W., K. Li, and E. Sirois. Simulated elliptical bioprosthetic valve deformation: implications for asymmetric transcatheter valve deployment. J. Biomech. 43:3085–3090, 2010.
Suo, J., J. Oshinski, and D. P. Giddens. Effects of wall motion and compliance on flow patterns in the ascending aorta. ASME J. Biomech. Eng. 125:347–354, 2003.
Tan, F. P. P., A. Borghi, R. H. Mohiaddin, N. B. Wood, S. Thom, and X. Y. Xu. Analysis of flow patterns in a patient-specific thoracic aortic aneurysm model. Comput. Struct. 87:680–690, 2009.
Tan, F. P. P., N. B. Wood, G. Tabor, and X. Y. Xu. Comparison of LES of steady transitional flow in an idealized stenosed axisymmetric artery model with a RANS transitional model. ASME J. Biomech. Eng. 133:051001-1–051001-12, 2011.
Viscardi, F., C. Vergara, C. L. Antiga, S. Merelli, A. Veneziani, G. Puppini, G. Faggian, A. Mazzucco, and G. B. Luciani. Comparative finite element model analysis of ascending aortic flow in bicuspid and tricuspid aortic valve. Artif. Organs. 34:1114–1120, 2010.
Webb, J. G., L. Altwegg, R. Boone, A. Chung, J. Ye, S. Lichtenstein, M. Lee, et al. Transcatheter aortic valve implantation: impact on clinical and valve-related outcomes. Circulation 119:3009–3016, 2009.
Webb, J. G., S. Pasupati, K. Humphries, C. Thompson, L. Altwegg, R. Moss, A. Sinhal, et al. Percutaneous transarterial aortic valve replacement in selected high-risk patients with aortic stenosis. Circulation 116:755–763, 2007.
Weinberg, E. J., and M. R. Mofrad. Transient, three-dimensional, multiscale simulations of the human aortic valve. Cardiovasc. Eng. 7:140–155, 2007.
Weston, M. W., D. V. LaBorde, and A. P. Yoganathan. Estimation of the shear stress on the surface of an aortic valve leaflet. Ann. Biomed. Eng. 27:572–579, 1999.
Wilcox, D. C. Turbulence Modelling for CFD (1st ed.). Glendale: Griffin Printing, 1993.
Wilcox, D. C. Turbulence Modelling for CFD (3rd ed.). La Canada: DCW Industries, 2006.
Yoganathan, A. P., Z. He, and S. C. Jones. Fluid mechanics of heart valves. Ann. Rev. Biomed. Eng. 6:331–362, 2004.
Acknowledgments
The first author acknowledges funding received from the Foundation for Circulatory Health, International Centre for Circulatory Health, London. RT was supported by the Magdi Yacoub Institute as the Qatar Cardiovascular Research Center Fellow. The work was also supported by the cardiovascular biomedical research unit of Royal Brompton Hospital and Imperial College London.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor W. Robert Taylor oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Tan, F.P.P., Xu, X.Y., Torii, R. et al. Comparison of Aortic Flow Patterns Before and After Transcatheter Aortic Valve Implantation. Cardiovasc Eng Tech 3, 123–135 (2012). https://doi.org/10.1007/s13239-011-0073-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-011-0073-3