Abstract
Objective
We assessed the role of DHEA supplementation on pregnancy rates in women with diminished ovarian function.
Design
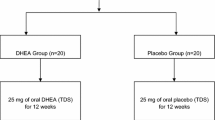
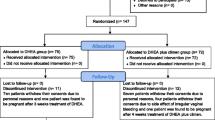
This is a case control study of 190 women with diminished ovarian function. The study group includes 89 patients who used supplementation with 75 mg daily of oral, micronized DHEA for up to 4 months prior to entry into in vitro fertilization (IVF). The control group is composed of 101 couples who received infertility treatment, but did not use DHEA. The primary outcome was clinical pregnancy after the patient’s initial visit. We developed a Cox proportional hazards model to compare the proportional hazards of pregnancy among women using DHEA with the controls group.
Results
Cumulative clinical pregnancy rates were significantly higher in the study group (25 pregnancies; 28.4% vs. 11 pregnancies; 11.9%; relative hazard of pregnancy in study group (HR 3.8; 95% CI 1.2–11.8; p < 0.05).
Conclusions
DHEA treatment resulted in significantly higher cumulative pregnancy rates. These data support a beneficial effect of DHEA supplementation among women with diminished ovarian function.

Similar content being viewed by others
References
Casson PR, Lindsay MS, Pisarska MD, Carson SA, Buster JE. Dehydroepiandrosterone supplementation augments ovarian stimulation in poor responders: a case series. Hum Reprod 2000;15(10):2129–32.
Barad D, Gleicher N. Increased oocyte production after treatment with dehydroepiandrosterone. Fertil Steril 2005;84(3):756.
Barad, Gleicher N. Effect of dehydroepiandrosterone on oocyte and embryo yields, embryo grade and cell number in IVF. Hum Reprod 2006;21(11):2845–9.
ASRM/SART-Registry. Assisted reproductive technology in the United States: 2000 results generated from the American Society for Reproductive Medicine/Society for Assisted Reproductive Technology Registry. Fertil Steril 2004;81(5):1207–20.
Barad D, Weghofer A, Gleicher N. O-291: evidence for an empiric definition of diminished ovarian reserve (DOR), ovarian resistance to stimulation and diagnosis of premature ovarian aging (POA), based on age-specific baseline FSH levels. Fertil Steril 2006;86(3, Supplement 1):S125–S6.
Schoolcraft W, Schlenker T, Gee M, Stevens J, Wagley L. Improved controlled ovarian hyperstimulation in poor responder in vitro fertilization patients with a microdose follicle-stimulating hormone flare, growth hormone protocol. Fertil Steril 1997;67(1):93–7.
Gleicher N, VanderLaan B, Pratt D, Karande V. Background pregnancy rates in an infertile population. Hum Reprod 1996;11(5):1011–2.
Collins JA, Wrixon W, Janes LB, Wilson EH. Treatment-independent pregnancy among infertile couples. N Engl J Med 1983;309(20):1201–6.
Karande V, Gleicher N. A rational approach to the management of low responders in in-vitro fertilization. Hum Reprod 1999;14(7):1744–8.
Harper AJ, Buster JE, Casson PR. Changes in adrenocortical function with aging and therapeutic implications. Semin Reprod Endocrinol 1999;17(4):327–38.
Hillier SG, Whitelaw PF, Smyth CD. Follicular oestrogen synthesis: The ‘two-cell, two-gonadotrophin’ model revisited. Mol Cell Endocrinol 1994;100(1–2):51–4.
Dorrington JH, Moon YS, Armstrong DT. Estradiol 17[beta] biosynthesis in cultured granulosa cells from hypophysectomized immature rats; stimulation by follicle stimulating hormone. Endocrinology 1975;97(5):1328–31.
Haning R Jr, Hackett R, Flood C, Loughlin J, Zhao Q, Longcope C. Plasma dehydroepiandrosterone sulfate serves as a prehormone for 48% of follicular fluid testosterone during treatment with menotropins. J Clin Endocrinol Metab 1993;76(5):1301–7.
Hillier SG. Sex steroid metabolism and follicular development in the ovary. Oxf Rev Reprod Biol 1985;7:168–222.
Daniel SAJ, Armstrong DT. Androgens in the ovarian microenvironment. Sem Reprod Endocrinol 1986;4(2):89–100.
Gore-Langton R, Armstrong D. Follicular steroidogenesis and its control. In: Knobil E, Neill J, editors. The physiology of reproduction. New York: Raven Press; 1988. p. p. 331–85.
Harlow CR, Hillier SG, Hodges JK. Androgen modulation of follicle-stimulation hormone-induced granulosa cell steroidogenesis in the primate ovary. Endocrinology 1986;119(3):1403–5.
Vendola K, Zhou J, Wang J, Famuyiwa OA, Bievre M, Bondy CA. Androgens promote oocyte insulin-like growth factor I expression and initiation of follicle development in the primate ovary. Biol Reprod 1999;61(2):353–7.
Yan Z, Lee GY, Anderson E. Influence of dehydroepiandrosterone on the expression of insulin-like growth factor-1 during cystogenesis in polycystic rat ovaries and in cultured rat granulosa cells. Biol Reprod 1997;57(6):1509–16.
Casson PR, Santoro N, Elkind-Hirsch K, et al. Postmenopausal dehydroepiandrosterone administration increases free insulin-like growth factor-I and decreases high-density lipoprotein: a six-month trial. Fertil Steril 1998;70(1):107–10.
Frattarelli JL, Peterson EH. Effect of androgen levels on in vitro fertilization cycles. Fertil Steril 2004;81(6):1713–4.
Barbieri RL, Sluss PM, Powers RD, et al. Association of body mass index, age, and cigarette smoking with serum testosterone levels in cycling women undergoing in vitro fertilization. Fertil Steril 2005;83(2):302–8.
Goswami SK, Das T, Chattopadhyay R, et al. A randomized single-blind controlled trial of letrozole as a low-cost IVF protocol in women with poor ovarian response: a preliminary report. Hum Reprod 2004;19(9):2031–5.
Mitwally MF, Casper RF. Aromatase inhibition improves ovarian response to follicle-stimulating hormone in poor responders. Fertil Steril 2002;77(4):776–80.
MacDougall M, Tan S, Balen A, Jacobs H. A controlled study comparing patients with and without polycystic ovaries undergoing in-vitro fertilization. Hum Reprod 1993;8(2):233–7.
Maciel GAR, Baracat EC, Benda JA, et al. Stockpiling of transitional and classic primary follicles in ovaries of women with polycystic ovary syndrome. J Clin Endocrinol Metab 2004;89(11):5321–7.
Amirikia H, Savoy-Moore RT, Sundareson AS, Moghissi KS. The effects of long-term androgen treatment on the ovary. Fertil Steril 1986;45(2):202–8.
Pache TD, Chadha S, Gooren LJ, et al. Ovarian morphology in long-term androgen-treated female to male transsexuals. A human model or the study of polycystic ovarian syndrome? Histopathology.1991;19(5):445–52.
Kaipia A, Hsueh AJ. Regulation of ovarian follicle atresia. Annu Rev Physiol 1997;59:349–63.
Billig H, Furuta I, Hsueh AJ. Estrogens inhibit and androgens enhance ovarian granulosa cell apoptosis. Endocrinology 1993;133(5):2204–12.
Kroboth PD, Salek FS, Pittenger AL, Fabian TJ, Frye RF. DHEA and DHEA-S: a review. J Clin Pharmacol 1999;39(4):327–48.
Kaaks R, Berrino F, Key T, et al. Serum sex steroids in premenopausal women and breast cancer risk within the European Prospective Investigation into Cancer and Nutrition (EPIC). J Natl Cancer Inst 2005;97(10):755–65.
McClamrock HD, Adashi EY. Gestational hyperandrogenism. Fertil Steril 1992;57(2):257–74.
Sir-Petermann T, Maliqueo M, Angel B, Lara HE, Perez-Bravo F, Recabarren SE. Maternal serum androgens in pregnant women with polycystic ovarian syndrome: possible implications in prenatal androgenization. Hum Reprod 2002;17(10):2573–9.
Author information
Authors and Affiliations
Corresponding author
Additional information
DB and NG are signatories on a pending patent application which claims a beneficial benefit for dehydroepiandrosterone supplementation on ovarian function.
Rights and permissions
About this article
Cite this article
Barad, D., Brill, H. & Gleicher, N. Update on the use of dehydroepiandrosterone supplementation among women with diminished ovarian function. J Assist Reprod Genet 24, 629–634 (2007). https://doi.org/10.1007/s10815-007-9178-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-007-9178-x