Abstract
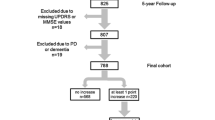
The progression of mild parkinsonian signs in the absence of idiopathic Parkinson’s disease in aging is unclear. This study aims to identify predictors of the evolution of mild parkinsonian signs in non-demented older adults. Two hundred ten participants (76.25 ± 7.10 years, 57 % women) were assessed at baseline and 1-year follow-up. Mild parkinsonian signs were defined as the presence of bradykinesia, rigidity and/or rest tremor. Depending upon the presence of these features at baseline and follow-up, participants were divided into one of four groups (no, transient, persistent or new-onset mild parkinsonian signs). Physical function was assessed using gait velocity. Ninety-five participants presented with mild parkinsonian signs at baseline. At 1-year follow-up, 59 demonstrated persistent mild parkinsonian signs, while 36 recovered (i.e., transient). Participants with persistent mild parkinsonian signs were older (79.66 ± 7.15 vs. 75.81 ± 7.37 years, p = 0.01) and evidenced slower gait velocity (90.41 ± 21.46 vs. 109.92 ± 24.32 cm/s, p < 0.01) compared to those with transient mild parkinsonian signs. Gait velocity predicted persistence of mild parkinsonian signs, even after adjustments (OR: 0.96, 95 % CI: 0.94–0.98). Fifty-five participants demonstrated new-onset of mild parkinsonian signs. In comparison to participants without mild parkinsonian signs, presence of cardiovascular but not cerebrovascular disease at baseline was associated with new-onset mild parkinsonian signs. Our study reveals that gait velocity was the main predictor of persistent mild parkinsonian signs, whereas cardiovascular disease was associated with new-onset mild parkinsonian signs. These findings suggest a vascular mechanism for the onset of mild parkinsonian signs and a different mechanism, possibly neurodegenerative, for the persistence of mild parkinsonian signs.


Similar content being viewed by others
References
Bennett DA, Beckett LA, Murray AM, Shannon KM, Goetz CG, Pilgrim DM, Evans DA (1996) Prevalence of parkinsonian signs and associated mortality in a community population of older people. N Engl J Med 334(2):71–76. doi:10.1056/NEJM199601113340202
Louis ED, Schupf N, Marder K, Tang MX (2006) Functional correlates of mild parkinsonian signs in the community-dwelling elderly: poor balance and inability to ambulate independently. Mov Disord 21(3):411–416. doi:10.1002/mds.20735
Louis ED, Luchsinger JA (2006) History of vascular disease and mild parkinsonian signs in community-dwelling elderly individuals. Arch Neurol 63(5):717–722. doi:10.1001/archneur.63.5.717
Uemura Y, Wada-Isoe K, Nakashita S, Nakashima K (2013) Depression and cognitive impairment in patients with mild parkinsonian signs. Acta Neurol Scand 128(3):153–159. doi:10.1111/ane.12089
Richards M, Stern Y, Marder K, Cote L, Mayeux R (1993) Relationships between extrapyramidal signs and cognitive function in a community-dwelling cohort of patients with Parkinson’s disease and normal elderly individuals. Ann Neurol 33(3):267–274. doi:10.1002/ana.410330307
Wilson RS, Schneider JA, Bienias JL, Evans DA, Bennett DA (2003) Parkinsonianlike signs and risk of incident Alzheimer disease in older persons. Arch Neurol 60(4):539–544. doi:10.1001/archneur.60.4.539
Louis ED, Tang MX, Mayeux R (2004) Parkinsonian signs in older people in a community-based study: risk of incident dementia. Arch Neurol 61(8):1273–1276. doi:10.1001/archneur.61.8.1273
Mitchell SL, Rockwood K (2000) The association between parkinsonism, Alzheimer’s disease, and mortality: a comprehensive approach. J Am Geriatr Soc 48(4):422–425
Waite LM, Grayson DA, Piguet O, Creasey H, Bennett HP, Broe GA (2005) Gait slowing as a predictor of incident dementia: 6-year longitudinal data from the Sydney older persons study. J Neurol Sci 229–230:89–93. doi:10.1016/j.jns.2004.11.009
Louis ED, Tang MX, Schupf N, Mayeux R (2005) Functional correlates and prevalence of mild parkinsonian signs in a community population of older people. Arch Neurol 62(2):297–302. doi:10.1001/archneur.62.2.297
Fleischman DA, Wilson RS, Schneider JA, Bienias JL, Bennett DA (2007) Parkinsonian signs and functional disability in old age. Exp Aging Res 33(1):59–76. doi:10.1080/03610730601006370
Louis ED, Tang MX, Schupf N (2010) Mild parkinsonian signs are associated with increased risk of dementia in a prospective, population-based study of elders. Mov Disord 25(2):172–178. doi:10.1002/mds.22943
Israeli-Korn SD, Massarwa M, Schechtman E, Strugatsky R, Avni S, Farrer LA, Friedland RP, Inzelberg R (2010) Mild cognitive impairment is associated with mild parkinsonian signs in a door-to-door study. J Alzheimers Dis 22(3):1005–1013. doi:10.3233/jad-2010-101230
Buchman AS, Leurgans SE, Nag S, Bennett DA, Schneider JA (2011) Cerebrovascular disease pathology and parkinsonian signs in old age. Stroke 42(11):3183–3189. doi:10.1161/strokeaha.111.623462
Buchman AS, Shulman JM, Nag S, Leurgans SE, Arnold SE, Morris MC, Schneider JA, Bennett DA (2012) Nigral pathology and parkinsonian signs in elders without Parkinson disease. Ann Neurol 71(2):258–266. doi:10.1002/ana.22588
Holtzer R, Wang C, Verghese J (2013) Performance variance on walking while talking tasks: theory, findings, and clinical implications. Age. doi:10.1007/s11357-013-9570-7
Holtzer R, Mahoney J, Verghese J (2013) Intraindividual variability in executive functions but not speed of processing or conflict resolution predicts performance differences in gait speed in older adults. J Gerontol A Biol Sci Med Sci. doi:10.1093/gerona/glt180
Holtzer R, Goldin Y, Zimmerman M, Katz M, Buschke H, Lipton RB (2008) Robust norms for selected neuropsychological tests in older adults. Arch Clin Neuropsychol 23(5):531–541. doi:10.1016/j.acn.2008.05.004
Verghese J, Lipton RB, Hall CB, Kuslansky G, Katz MJ, Buschke H (2002) Abnormality of gait as a predictor of non-Alzheimer’s dementia. N Engl J Med 347(22):1761–1768. doi:10.1056/NEJMoa020441
Fahn SER (1987) Unified Parkinson’s Disease Rating Scale. MacMillan Healthcare Information, Florham Park
Allali G, Verghese J, Mahoney JR (2014) Contributions of mild parkinsonian signs to gait performance in the elderly. Age 36(4):9678. doi:10.1007/s11357-014-9678-4
Louis ED, Bennett DA (2007) Mild Parkinsonian signs: an overview of an emerging concept. Mov Disord 22(12):1681–1688. doi:10.1002/mds.21433
Yesavage JA, Brink TL, Rose TL, Lum O, Huang V, Adey M, Leirer VO (1982) Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res 17(1):37–49
Holtzer R, Verghese J, Xue X, Lipton RB (2006) Cognitive processes related to gait velocity: results from the Einstein aging study. Neuropsychology 20(2):215–223. doi:10.1037/0894-4105.20.2.215
Verghese J, Kuslansky G, Holtzer R, Katz M, Xue X, Buschke H, Pahor M (2007) Walking while talking: effect of task prioritization in the elderly. Arch Phys Med Rehabil 88(1):50–53. doi:10.1016/j.apmr.2006.10.007
Verghese J, Wang C, Lipton RB, Holtzer R, Xue X (2007) Quantitative gait dysfunction and risk of cognitive decline and dementia. J Neurol Neurosurg Psychiatry 78(9):929–935. doi:10.1136/jnnp.2006.106914
Verghese JHR, Lipton RB, Wang C (2009) Quantitative gait markers and incident fall risk in older adults. J Gerontol A Biol Sci Med Sci 64:896–901. doi:10.1093/gerona/glp033
Duff K, Humphreys Clark JD, O’Bryant SE, Mold JW, Schiffer RB, Sutker PB (2008) Utility of the RBANS in detecting cognitive impairment associated with Alzheimer’s disease: sensitivity, specificity, and positive and negative predictive powers. Arch Clin Neuropsychol 23(5):603–612. doi:10.1016/j.acn.2008.06.004
Corp I (Released 2011) SPSS Statistics for Windows. 20.0 edn. IBM Corp., Armonk, NY
Snijders AH, van de Warrenburg BP, Giladi N, Bloem BR (2007) Neurological gait disorders in elderly people: clinical approach and classification. Lancet Neurol 6(1):63–74
Bohnen NI, Frey KA, Studenski S, Kotagal V, Koeppe RA, Scott PJ, Albin RL, Muller ML (2013) Gait speed in Parkinson disease correlates with cholinergic degeneration. Neurology 81(18):1611–1616. doi:10.1212/WNL.0b013e3182a9f558
de Laat KF, van Norden AG, Gons RA, van Uden IW, Zwiers MP, Bloem BR, van Dijk EJ, de Leeuw FE (2012) Cerebral white matter lesions and lacunar infarcts contribute to the presence of mild parkinsonian signs. Stroke 43(10):2574–2579. doi:10.1161/strokeaha.112.657130
Wolf PA, Dawber TR, Thomas HE Jr, Kannel WB (1978) Epidemiologic assessment of chronic atrial fibrillation and risk of stroke: the Framingham study. Neurology 28(10):973–977
Kalra S, Grosset DG, Benamer HT (2010) Differentiating vascular parkinsonism from idiopathic Parkinson’s disease: a systematic review. Mov Disord 25(2):149–156. doi:10.1002/mds.22937
Acknowledgments
Research was supported by funding from the National Institute on Aging (R01AG036921-01A1 & R01AG044007-01A1). Special thanks to all of the CCMA research assistants for their assistance with data collection.
Conflicts of interest
No competing interests to report.
Funding
This study was supported by funds from the National Institutes of Health, National Institute on Aging (R01AG036921-01A1 & R01AG044007-01A1). Gilles Allali is supported by a Grant from the Geneva University Hospitals.
Ethical standards
The institutional review board of the Albert Einstein College of Medicine approved the experimental procedures and all participants provided written informed consent in accordance with the tenets of the Declaration of Helsinki.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mahoney, J.R., Verghese, J., Holtzer, R. et al. The evolution of mild parkinsonian signs in aging. J Neurol 261, 1922–1928 (2014). https://doi.org/10.1007/s00415-014-7442-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-014-7442-4