Abstract
Introduction
Hypothyroidism is associated with pregnancy complications both for the mother and progeny and it should be considered in reproductive age. Thyroid autoimmunity is stated to be the main cause of hypothyroidism in iodine sufficient areas. Polycystic ovary syndrome (PCOS) is known as the most common endocrine disorder affecting women in reproductive age. Early diagnosis and treatment of hypothyroidism in PCOS may reduce the rate of infertility and pregnancy-related morbidity. In the present study we evaluated thyroid autoimmunity in PCOS patients.
Methods
Over a period of 12 months, 78 patients with PCOS were recruited to this case–control study. Three hundred and fifty age-matched women were studied as a control group. PCOS was defined according to the revised 2003 Rotterdam criteria. Thyroid size was estimated by inspection and palpation. Serum thyroid stimulating hormone (TSH), anti-thyroperoxidase antibody (anti-TPO Ab), and anti-thyroglobulin antibody (anti-Tg Ab) were measured.
Results
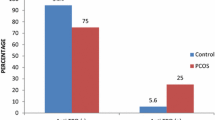
The mean ± SD of serum anti-TPO Ab in PCOS patients and subjects in the control group was 216 ± 428 and 131 ± 364 IU/mL, respectively (P = 0.04). Prevalence of goiter in PCOS patients was higher than that in control subjects (62.3 vs. 35.7%, P = 0.0001). Serum TSH and anti-Tg Ab in PCOS patients and control subjects did not differ significantly.
Conclusion
In this case–control study, anti-thyroid antibodies and goiter prevalence were significantly higher in PCOS patients. These data suggest that thyroid exam and evaluation of thyroid function and autoimmunity should be considered in such patients.
Similar content being viewed by others
References
Burek C, Rose N (2008) Autoimmune thyroiditis and ROS. Autoimmun Rev 7:530–537
Kostoglou-Athanassiou I, Ntalles K (2010) Hypothyroidism—new aspects of an old disease. Hippokratia 14:82–87
Poppe K, Velkeniers B, Glinoer D, Medscape (2008) The role of thyroid autoimmunity in fertility and pregnancy. Nat Clin Pract Endocrinol Metab 4:394–405
Tomer Y, Huber A (2009) The etiology of autoimmune thyroid disease: a story of genes and environment. J Autoimmun 32:231–239
Khalili N, Hashemipour M, Keshteli AH, Siavash M, Amini M (2009) The role of thyroid autoantibodies in the etiology of endemic goiter in schoolchildren of Isfahan, Iran. J Endocrinol Invest 32:899–902
Hashemipour M, Amini M, Aminorroaya A et al (2007) High prevalence of goiter in an iodine replete area: do thyroid auto-antibodies play a role? Asia Pac J Clin Nutr 16:403–410
Brent GA, Larsen PR, Davies TF (2008) Hypothyroidism and thyroiditis. In: Kronenberg HM, Melmed S, Polonsly KS, Larsen PR (eds) Williams text book of endocrinology, 11th edn. Saunders, Philadelphia, pp 378–383
Escobar-Morreale HF (2008) Polycystic ovary syndrome: treatment strategies and management. Expert Opin Pharmacother 9:2995–3008
Rosenfield RL (2008) What every physician should know about polycystic ovary syndrome. Dermatol Ther 21:354–361
Mascitelli L, Pezzetta F (2005) Polycystic ovary syndrome. N Engl J Med 352:2756–2757 (author reply 2756-2757)
Boomsma C, Fauser B, Macklon N (2008) Pregnancy complications in women with polycystic ovary syndrome. Semin Reprod Med 26:72–84
group REA-SPcw (2004) Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum Reprod 19:41–47
World Health Organization (2001) United Nations Children’s Fund and International Council for the Control of Iodine Deficiency Disorders. Assessment of iodine deficiency disorders and monitoring their elimination
Markou KB, Georgopoulos NA, Makri M et al (2003) Improvement of iodine deficiency after iodine supplementation in schoolchildren of Azerbaijan was accompanied by hypo and hyperthyrotropinemia and increased title of thyroid autoantibodies. J Endocrinol Invest 26:43–48
Janssen O, Mehlmauer N, Hahn S, Offner A, Gartner R (2004) High prevalence of autoimmune thyroiditis in patients with polycystic ovary syndrome. Eur J Endocrinol 150:363–369
Ott J, Aust S, Kurz C, Nouri K, Wirth S, Huber JC et al (2010) Elevated antithyroid peroxidase antibodies indicating Hashimoto’s thyroiditis are associated with the treatment response in infertile women with polycystic ovary syndrome. Fertil Steril 94:2895–2897
Giza S, Galli-Tsinopoulou A, Lazidou P, Trachana M, Goulis D (2008) HLA-DQB1*05 association with Hashimoto’s thyroiditis in children of Northern Greek origin. Indian Pediatr 45:493–496
Prapas N, Karkanaki A, Prapas I et al (2009) Genetics of polycystic ovary syndrome. Hippokratia 13:216–223
Hefler-Frischmuth K, Walch K, Huebl W et al (2010) Serologic markers of autoimmunity in women with polycystic ovary syndrome. Fertil Steril 93:2291–2294
Lahita R (1999) The role of sex hormones in systemic lupus erythematosus. Curr Opin Rheumatol 11:352–356
Acknowledgments
We would like to thank all the staff at Isfahan Endocrine and Metabolism Research Centre for their great cooperation with us. We are also thankful to the participants in the present study. This study was funded by the Vice Chancellery for Research and Technology, Isfahan University of Medical Sciences.
Conflict of interest
The authors declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kachuei, M., Jafari, F., Kachuei, A. et al. Prevalence of autoimmune thyroiditis in patients with polycystic ovary syndrome. Arch Gynecol Obstet 285, 853–856 (2012). https://doi.org/10.1007/s00404-011-2040-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-011-2040-5