Abstract
Background
The ColonRing™ represents a further advancement in compression anastomosis by using superelastic materials. In contrast to other compression devices, its field of application is identical to circular staplers. Yet, limited data are available and there are no reports on the use of this compression device for anastomoses in the lower rectum and in diverted cases.
Methods
Between November 2008 and March 2010 a nonrandomized prospective study of patients undergoing colorectal resection was done.
Results
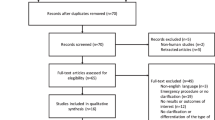
Sixty-two patients (30 female) with a median age of 67 years (range = 23-87) underwent surgery for benign (35) and malignant (27) indications;the surgery was performed laparoscopically in 53 (85.5%) cases. There were no leaks or other major complications related to the compression anastomosis. One patient died from sepsis caused by a leak of a colonic J-pouch. Three of 12 (25%) patients after (ultra-)low anterior resection experienced pain caused by the presence of the ring. Of 53 undiverted patients, rings were passed spontaneously in 52 (98.1%). No spontaneous passage occurred in patients with a stoma. Their rings were removed transanally prior to stoma closure. After a median of 6 months, endoscopic follow-up was performed in 60 patients (96.8%). Two anastomotic stenoses were detected (3.3%).
Conclusion
Construction of rectal anastomosis using this novel compression device is feasible and safe and appears to cause only few anastomotic strictures in the medium term. Discomfort or pain from the presence of the ring at anastomosis following (ultra-)low anterior resection can be observed in a relevant number of patients.



Similar content being viewed by others
References
Heald RJ, Leicester RJ (1981) The low stapled anastomosis. Br J Surg 68:333–337
Docherty JG, McGregor JR, Akyol AM et al (1995) Comparison of manually constructed and stapled anastomoses in colorectal surgery. West of Scotland and Highland Anastomosis Study Group. Ann Surg 221:176–184
Graf W, Gimelius B, Bergström R et al (1991) Complications after double and single stapling in rectal surgery. Eur J Surg 157:543–547
Rullier E, Laurent C, Garrelon JL et al (1998) Risk factors for anastomotic leakage after resection of rectal cancer. Br J Surg 85:355–358
Carlsen E, Schlichting E, Guldvog I et al (1998) Effect of the introduction of total mesorectal excision for the treatment of rectal cancer. Br J Surg 85:526–529
Matthiessen P, Hallböök O, Andersson M et al (2004) Risk factors for anastomotic leakage after anterior resection of the rectum. Colorectal Dis 6:462–469
Jech B, Felberbauer FX, Herbst F (2007) Complications of elective surgery for rectal cancer. Eur Surg 39:8–14
den Dulk M, Noter SL, Hendriks ER et al (2009) Improved diagnosis and treatment of anastomotic leakage after colorectal surgery. Eur J Surg Oncol 35:420–426
Taflampas P, Christodoulakis M, Tsiftsis DD (2009) Anastomotic leakage after low anterior resection for rectal cancer: facts, obscurity, and fiction. Surg Today 39:183–188
Thiede A, Geiger D, Dietz UA et al (1998) Overview on compression anastomoses: biofragmentable anastomosis ring multicenter prospective trial of 1666 anastomoses. World J Surg 22:78–86. doi:10.1007/s002689900353
Wullstein C, Gross E (2000) Compression anastomosis (AKA-2) in colorectal surgery: results in 442 consecutive patients. Br J Surg 87:1071–1075
Kaidar-Person O, Rosenthal R, Wexner SD et al (2008) Compression anastomosis: history and clinical considerations. Am J Surg 195:818–826
Chen TC, Ding KC, Yang MJ et al (1994) New device for biofragmentable anastomotic ring in low anterior resection. Dis Colon Rectum 37:834–836
Szold A (2008) New concepts for a compression anastomosis: Superelastic clips and rings. Minim Invasive Ther Allied Technol 17:168–171
Stewart D, Hunt S, Pierce R et al (2007) Validation of the NITI Endoluminal Compression Anastomosis Ring (EndoCAR) Device and Comparison to the Traditional Circular Stapled Colorectal Anastomosis in a Porcine Model. Surg Innov 14:252–260
Fasth S, Hedlund H, Svaninger G et al (1982) Autosuture of low colorectal anastomosis. Acta Chir Scand 148:535–539
Shimada S, Matsuda M, Uno K et al (1996) A new device for the treatment of coloproctostomic stricture after double stapling anastomoses. Ann Surg 224:603–608
Schlegel RD, Dehni N, Parc R et al (2001) Results of reoperations in colorectal anastomotic strictures. Dis Colon Rectum 44:1464–1468
Ambrosetti P, Francis K, De Peyer R et al (2008) Colorectal anastomotic stenosis after elective laparoscopic sigmoidectomy for diverticular disease: a prospective evaluation of 68 patients. Dis Colon Rectum 51:1345–1349
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Ravitch MM, Steichen FM (1972) Technics of staple suturing in the gastrointestinal tract. Ann Surg 175:815–837
Knight CD, Griffen F (1980) An improved technique for low anterior resection of the rectum using the EEA stapler. Surgery 88:710–714
Griffen FD, Knight CD Sr, Whitaker JM et al (1990) The double stapling technique for low anterior resection. Results, modifications, and observations. Ann Surg 211:745–751
Lustosa SA, Matos D, Atallah AN et al (2002) Stapled versus handsewn methods for colorectal anastomosis surgery: a systematic review of randomized controlled trials. Sao Paulo Med J 120:132–136
Rahbari NN, Weitz J, Hohenberger W et al (2010) Definition and grading of anastomotic leakage following anterior resection of the rectum: a proposal by the International Study Group of Rectal Cancer. Surgery 147:339–351
Hansen O, Schwenk W, Hucke HP et al (1996) Colorectal stapled anastomoses. Experiences and results. Dis Colon Rectum 39:30–36
Eckmann C, Kujath P, Schiedeck TH et al (2004) Anastomotic leakage following low anterior resection: results of a standardized diagnostic and therapeutic approach. Int J Colorectal Dis 19:128–133
Khan AA, Wheeler JM, Cunningham C et al (2008) The management and outcome of anastomotic leaks in colorectal surgery. Colorectal Dis 10:587–592
Hirano Y, Omura K, Tatsuzawa Y et al (2006) Tissue oxygen saturation during colorectal surgery measured by near-infrared spectroscopy: pilot study to predict anastomotic complications. World J Surg 30:457–461. doi:10.1007/s00268-005-0271-y
D’Hoore A, Hompes D, Folkesson J et al (2008) Circular ‘superelastic’ compression anastomosis: from the animal lab to clinical practice. Minim Invasive Ther Allied Technol 17:172–175
Dauser B, Herbst F (2009) NITI Endoluminal Compression Anastomosis Ring (NITI CAR 27®): a breakthrough in compression anastomoses? Eur Surg 41:116–119
Tulchinsky H, Kashtan H, Rabau M et al (2010) Evaluation of the NiTi Shape Memory BioDynamix ColonRing in colorectal anastomosis: first in human multi-center study. Int J Colorectal Dis 25:1453–1458
Buchberg BS, Masoomi H, Bergman H et al (2011) The use of a compression device as an alternative to hand-sewn and stapled colorectal anastomoses: is three a crowd? J Gastrointest Surg 15(2):304–310
Ho YH, Ashour MA (2010) Techniques for colorectal anastomosis. World J Gastroenterol 16:1620–1621
Riss S, Stift A, Meier M et al (2010) Endo-sponge assisted treatment of anastomotic leakage following colorectal surgery. Colorectal Dis 12:104–108
van Koperen PJ, van Berge Henegouwen MI, Rosman C et al (2009) The Dutch multicenter experience of the endo-sponge treatment for anastomotic leakage after colorectal surgery. Surg Endosc 23:1379–1383
Maggiori L, Bretagnol F, Lefèvre JH et al (2011) Conservative management is associated with decreased risk of definitive stoma after anastomotic leakage complicating sphincter-saving resection for rectal cancer. Colorectal Dis 13. doi:10.1111/j.1463-1318.2010.02252.x
Bannura GC, Cumsille MA, Barrera AE et al (2004) Predictive factors of stenosis after stapled colorectal anastomosis: prospective analysis of 179 consecutive patients. World J Surg 28:921–925. doi:10.1007/s00268-004-7375-7
Suchan KL, Muldner A, Manegold BC (2003) Endoscopic treatment of postoperative colorectal anastomotic strictures. Surg Endosc 17:1110–1113
Virgilio C, Cosentino S, Favara C et al (1995) Endoscopic treatment of postoperative colonic strictures using an achalasia dilator: short-term and long-term results. Endoscopy 27:219–222
Waxman BP, Ramsay AH (1986) The effect of stapler diameter and proximal colostomy on narrowing at experimental circular stapled large bowel anastomosis. Aust N Z J Surg 56:797–801
Martínez-Serrano MA, Parés D, Pera M et al (2009) Management of lower gastrointestinal bleeding after colorectal resection and stapled anastomosis. Tech Coloproctol 13:49–53
Disclosure
There were no financial ties with the manufacturer (NiTi Surgical Solutions Ltd., Netanya, Israel) or the supplier (AFS Medical GmbH, Teesdorf, Austria) of the devices used in this study. There was no financial support for study personnel, free equipment, or writing services.
Author information
Authors and Affiliations
Corresponding author
Additional information
The study was registered at ClinicalTrials.gov under NCT01056913.
Rights and permissions
About this article
Cite this article
Dauser, B., Winkler, T., Loncsar, G. et al. Compression Anastomosis Revisited: Prospective Audit of Short- and Medium-term Outcomes in 62 Rectal Anastomoses. World J Surg 35, 1925–1932 (2011). https://doi.org/10.1007/s00268-011-1135-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-011-1135-2