Abstract
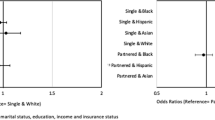
Objectives: To examine pre-pregnancy Medicaid coverage and initiation of prenatal care among women likely eligible for Medicaid coverage regardless of pregnancy. Methods: The Pregnancy Risk Assessment Monitoring System (PRAMS) was used to identify very low-income women with Medicaid payment for delivery. We then compared prenatal care initiation among women with (Non-GAP) and without (Medicaid GAP) pre-pregnancy Medicaid coverage. Results: Rates of first trimester prenatal care were 47.3% for women in the Medicaid GAP, 70.0% for women who were not. The adjusted odds ratio for being in the Medicaid GAP and delayed prenatal care was 2.7 (95% CI 1.2, 6.2), although this varied by race/ethnicity and education. The relationship was strongest among White and Hispanic women with less than a high school education: OR=13.8, (95% CI 3.0, 62.7) and OR=19.0 (95% CI 2.4, 149.2), respectively. Conclusions: Pre-pregnancy Medicaid coverage appears to be associated with early initiation of prenatal care. Almost a decade after welfare reform, it is essential to preserve the Medicaid expansions for pregnant women, foster Medicaid family planning waivers, and promote access to primary care and early prenatal care, particularly for very low-income women.
Similar content being viewed by others
References
Fiscella K. Does prenatal care improve birth outcomes? A critical review. Obstet Gynecol 1995;85:468–79.
Huntington J, Connell F. (Sounding Board). For every dollar spent-the cost-savings argument for prenatal care. N Eng J Med 1994;331:1303–7.
Martin J, Hamilton B, Sutton P, Ventura S, Menacker F, Munson M. Births: Final data for 2003. Natl Vital Stat Rep 2005;54(2).
Vintzileos A, Ananth C, Smulian J, Scorza W, Knuppel R. The impact of prenatal care on preterm births in the presence and absence of antenatal high-risk conditions. Am J Obstet Gynecol 2002;187(5):1254–7.
Vintzileos A, Ananth C, Smulian J, Scorza W, Knuppel R. Prenatal care and black-white fetal death disparity in the United States: Heterogeneity by high-risk conditions. Obstet Gynecol 2002;99:483–9.
Vintzileos A, Ananth C, Smulian J, Scorza W, Knuppel R. The impact of prenatal care on neonatal deaths in the presence and absence of antenatal high-risk conditions. Am J Obstet Gynecol 2002;186:1011–6.
Vintzileos A, Ananth C, Smulian J, Scorza W. The impact of prenatal care on preterm births among twin gestations in the United States, 1989–2000. Am J Obstet Gynecol 2003;189(3):818–23.
Kogan M, Alexander G, Jack B, Allen M. The association between adequacy of prenatal care utilization and subsequent pediatric care utilization in the United States. Pediatrics 1998;102:25–30.
Kogan M, Martin J, Alexander G, Kotelchuck M, Ventura S, Frigoletto F. Letter. Benefits and limitations of prenatal care. JAMA 1998;280:2071–3.
Meis P, Klebanoff M, Thorn E. Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. N Engl J Med 2003;348(24):2379–85.
Kotelchuck M. An evaluation of the Kessner adequacy of prenatal care index and a proposed adequacy of prenatal care utilization index. Am J Public Health 1994;84:1414–20.
Department of Health and Human Services. Healthy People 2010, Conference Edition. Available at: http://www.health.gov/healthypeople/Document/tableofcontents.htm. Access-ed January, 2004.
Howell E. The impact of the Medicaid expansions for pregnant women: A synthesis of the evidence. Med Care Res Rev 2001;58(1):3–30.
Dubay L, Joyce T, Kaestner R, Kenney G. Changes in prenatal care timing and low birth weight by race and socioeconomic status: Implications for the Medicaid expansions for pregnant women. Health Serv Res 2001;36(2):373–403.
Kramer M, Seguin L, Lydon J, Goulet L. Socio-economic disparities in pregnancy outcome: Why do the poor fare so poorly? Paediatr Perinat Epidemiol 2000;14:194–210.
Misra D, Grason H, Weisman C. An intersection of women's and perinatal health: The role of chronic conditions. Women's Health Issues 2000;10(5):256–67.
Jack B, Culpepper L. Preconception Care. In: Merkatz I, Thompson J, editors. New perspectives on prenatal care. New York, NY: Elsevier Science, 1990:69–88.
Egerter S, Braveman P, Marchi K. Timing of insurance and use of prenatal care among low-income women. Am J Public Health 2002;92(3):423–7.
Braveman P, Marchi K, Sarnoff R, Egerter S, Rittenhouse D. Promoting access to prenatal care: Lessons from the California experience. Washington, DC: The Henry J. Kaiser Family Foundation, 2003.
Ellwood M. The Medicaid eligibility maze: Coverage expands, but enrollment problems persist. Findings from a five state study. Cambridge, MA: Mathematica Policy Research, Inc., 1999.
Handler A, Rosenberg D, Rankin K, Zimbeck M, Adams K. The effect of welfare reform on the pre-pregnancy insurance status of public aid recipients: Women in the Medicaid GAP. J Health Care Poor Underserved 2006;17(1):162--179.
Rogers M, Ahluwalia I, Melvin C. The Pregnancy Risk Assessment Monitoring System (PRAMS). J Womens Health 1998;7(7):799–801.
Wilson J. The crucial link between literacy and health. Ann Intern Med 2003;139(10):875–8.
Ku L, Fremstad S, Broaddus M. Noncitizens' use of public benefits has declined since 1996: Recent report paints misleading picture of impact of eligibility restrictions on immigrant families. Washington, DC: Center on Budget and Policy Priorities, 2003.
Gold RB. Immigrants and Medicaid after welfare reform. The Guttmacher report on public policy. 2003;6(2):6–9.
Feld P, Power B. Immigrants' access to health care after welfare reform: Findings from focus groups in four cities. Washington, DC: Kaiser Commission on Medicaid and the Uninsured, The Henry J. Kaiser Family Foundation, 2000.
Kaiser Commission on Medicaid and the Uninsured. Medicaid eligibility and citizenship status: Policy Implications for immigrant populations. Washington, DC: Kaiser Commission on Medicaid and the Uninsured, The Henry J. Kaiser Family Foundation, 2000.
Augustyn M, Maiman L. Psychological and sociological barriers to prenatal care. Women's Health Issues 1994;4(1):20–7.
Kost K, Landry D, Darroch J. Predicting maternal behaviors during pregnancy: Does intention status matter? Fam Plann Pers 1998;30(2):79–88.
Sanders-Phillips K, Davis S. Improving prenatal care services for low-income African-American women and infants. J Health Care Poor Underserved 1998;9(1):14–29.
Nothnagle M, Marchi K, Egerter S, Braveman P. Risk factors for late or no prenatal care following Medicaid expansions in California. Matern Child Health J 2000;4(4):251–9.
National Governor's Association for Best Practices. MCH update 2002; State health coverage for low-income pregnant women, children and parents. June 9, 2003.
Piper J, Ray W, Griffin M. Effects of Medicaid eligibility expansion on prenatal care and pregnancy outcome in Tennessee. JAMA 1990;264(17):2219–23.
Braveman P, Bennett T, Lewis C, Egerter S, Showstack J. Access to prenatal care following major Medicaid eligibility expansions. JAMA 1993;269:1285–9.
Haas J, Udvarhelyi S, Morris C, Epstein A. The effect of providing health coverage to poor uninsured pregnant women in Massachusetts. JAMA 1993;269(1):87–91.
Ray W, Mitchel E Jr, Piper J. Effect of Medicaid expansions on preterm birth. Am J Prev Med 1997;13:292–7.
Baldwin LM, Larson E, Connell F, Nordlund D, Cain K, Cawthon ML, Bryns P, Rosenblatt R. The effect of expanding Medicaid prenatal services on birth outcomes. Am J Public Health 1998;88:1623–9.
Long S, Marquis MS. The effects of Florida's Medicaid eligibility expansion for pregnant women. Am J Public Health 1998;88:371–6.
Kaiser Family Foundation. Medicaid: A critical source of support for family planning in the United States. Issue Brief. Menlo Park, CA: The Henry J. Kaiser Family Foundation, April, 2005.
Blumberg S, Cynamon M. Misreporting Medicaid enrollment: Results of three studies linking telephone surveys to state administrative records. In: Cynamon M, Kulka M, editors. Proceedings of the Seventh Conference on Health Survey Research Methods. DHHS. Hyattsville, MD, 2001. DHHS Publication No. (PHS) 01–1013.
National Conference of State Legislatures and American Public Welfare Association. Analysis of the Personal Responsibility and Work Opportunity Reconciliation Act of 1996. Revised August 30, 1996.
Williams L, Morrow B, Lansky A, Becky L, Barfield W, Helms K, Lipscomb L, Whitehead N. Surveillance for selected maternal behaviors and experiences before, during and after pregnancy. Morbidity and Mortality Weekly Report, Surveillance Summaries, 52/SS-11, 2003.
Phares T, Morrow B, Lansky A, Barfield C, Prince C, Marchi K, Braveman P, Williams L, Kinniburgh B. Surveillance for disparities in maternal health-related behaviors-selected states, Pregnancy Risk Assessment Monitoring System (PRAMS), 2000–2001. Morbidity and Mortality Weekly Report, Surveillance Summaries, 53/SS-4, July 2, 2004.
Acknowledgements
This analysis was conducted with funding support from the Maternal and Child Health Bureau Research Program, Grant R40MC00209. The authors thank members of the PRAMS staff at the Centers for Disease Control and Prevention and the PRAMS staff from the eight states included in this analysis for permitting us to use the PRAMS data and for reviewing and providing feedback on the completed manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosenberg, D., Handler, A., Rankin, K.M. et al. Prenatal care initiation among very low-income women in the aftermath of welfare reform: does pre-pregnancy Medicaid coverage make a difference?. Matern Child Health J 11, 11–17 (2007). https://doi.org/10.1007/s10995-006-0077-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-006-0077-z