Abstract
Objective
To explore the effects of long-term oral ACEIs/ARBs on the incidence of exacerbation and in-hospital mortality in elderly COVID-19 Omicron BA.2 patients with hypertension, especially patients aged 80 years or older.
Materials and methods
In this retrospective study, patients suffering mild and rcommon COVID-19 with hypertension who were hospitalized in the Shanghai Fourth People’s Hospital between April 2022 and June 2022 were enrolled. Primary outcomes included the incidence of exacerbation and in-hospital mortality. Secondary outcomes included the incidence of respiratory failure of patients, use of mechanical ventilation, nucleic acid conversion time (NCT), hospitalization costs, and the temporal trend of the incidence of exacerbations and in-hospital mortality in different age groups. The data were analysed using propensity score weighting (PSW).
Results
In the entire cohort, there were 298 ACEI/ARB users and 465 non-ACEI/ARB users. The ACEI/ARB group showed a lower incidence of exacerbation (OR = 0.64, 95% CI for OR: 0.46–0.89, P = 0.0082) and lower in-hospital mortality (OR = 0.49, 95% CI for OR: 0.27–0.89, P = 0.0201) after PSW. Sensitivity analysis obtained the same results. The results of the subgroup of patients aged 80 years and older obtained a similar conclusion as the whole cohort. Most of the study indicators did not differ statistically significantly in the subgroup of patients aged 60 to 79 years except for rates of mechanical ventilation and respiratory failure.
Conclusion
Antihypertensive therapy with ACEIs/ARBs might reduce the incidence of exacerbation and in-hospital mortality. The findings of this study support the use of ACEIs/ARBs in COVID-19 patients infected by Omicron BA.2, especially in patients aged 80 years or older with hypertension.
Similar content being viewed by others
Introduction
The coronavirus disease 2019 (COVID-19) pandemic is caused by the novel coronavirus SARS-CoV-2. Angiotensin-converting enzyme 2 (ACE2) is not only an enzyme but also a functional receptor on cell surfaces. SARS-CoV-2 enters host cells and causes ACE/ACE2 balance disruption and renin-angiotensin-aldosterone system (RAAS) activation. Some studies have shown that the expression of ACE2 and its regulation by conditions and potential complications may increase the susceptibility of tissues to COVID-19 [1]. Some researchers have proposed that the downregulation of ACE2 reduces susceptibility to SARS-CoV-2 infection in vitro, in vivo and human lungs and livers perfused ex situ by a series of model verification [2]. Angiotensin-converting enzyme inhibitors (ACEIs) and angiotensin II receptor blockers (ARBs) are RAAS inhibitors and have traditionally been used as first-line medications to treat hypertension [3, 4]. However, the use of ACEIs/ARBs in hypertensive patients with COVID-19 has aroused controversy. ACE2 is one of the issues at stake in the debate [5, 6]. Animal studies have demonstrated that ACEIs and ARBs can upregulate the expression of ACE2 [7]. Theoretically, such treatments could increase the risk of COVID-19 infection or exacerbate the severity of the disease. Several previous studies have shown that ACE2 expression is downregulated following SARS infection, which causes RAS overactivation and promotes pneumonia progression [8]. Oral treatment by ACEIs/ARBs could in turn inhibit the overactivation of RAS induced by the downregulation of ACE2 and thus prevent acute pulmonary injuries. Various cohort studies in different countries have investigated the relationship between ACEI or ARB treatment and severe outcomes of hospitalized COVID-19 patients, but the findings were inconsistent [9,10,11,12,13,14]. Richardson et al. [10] reported higher rates of mortality in patients on ACEIs/ARBs than in nonusers. In contrast, some evidence supports the benefit of using ACEIs or ARBs to potentially contribute to the improvement of clinical outcomes of COVID-19 patients with hypertension, and RAAS inhibitors might be associated with better COVID-19 prognosis [11, 12]. Some studies have proposed that ACEIs/ARBs are not associated with the severity and outcomes of COVID-19 infection in hospitalized patients with hypertension [13, 14].
The COVID-19 pandemic has even more drastic effects on elderly patients than on the general population. Large-scale clinical data have shown that elderly patients have a higher risk of COVID-19 incidence than the general population due to their advanced ages and medical comorbidities, such as hypertension and diabetes [15]. Most of the above studies have been conducted from the perspectives of mortality and infection rates, providing a reference basis for our clinical medication. The main focus of research so far has been on the early strain with stronger pathogenicity. In April 2022, the epidemic strain in Shanghai became Omicron, which has stronger transmission but weaker pathogenicity. We wanted to investigate whether COVID-19 Omicron is affected by ACEIs/ARBs.
During the COVID-19 pandemic, once severe cases occur, the lack of medical resources may lead to adverse outcomes for patients to consider. Preventing patients from transitioning from mild to severe is important. The purpose of this retrospective cohort study was to investigate the relationship between the use of ACEIs/ARBs and the occurrence of COVID-19 Omicron exacerbation and the in-hospital mortality of elderly patients with hypertension.
Materials and methods
Patients
This is a retrospective cohort study. All patients who were diagnosed with COVID-19 according to being tested positive using real-time reverse transcription polymerase chain reaction (RT‒PCR) testing via nasopharyngeal swabs were screened from April 12, 2022 to June 17, 2022 at Shanghai Fourth People`s Hospital, Shanghai, China. The cases in the study were classified as Omicron BA.2 by inference from previous studies which performed genomic analysis showing that there was a predominance of Omicron during the period evaluated [16, 17]. The inclusion criteria were age 60 years or older, diagnosed with essential hypertension, and taking antihypertensive medication regularly over 1 month before study inclusion. Patients admitted with asymptomatic COVID-19, with other reasons requiring oral ACEI, with survival time less than 48 h after admission, or time of diagnosis that could not be determined were excluded. Causing one of our primary outcomes was the incidence of exacerbations, and we excluded patients admitted with a diagnosis of severe or critical COVID-19. The Shanghai Fourth People’s Hospital Electronic Health Record was used to collect clinical information such as demographics, treatment, intraoperative data, pathology, and clinical outcomes.
The amended Helsinki Declaration commissioned this study. The study was approved by the Ethics Committee of the hospital (No. 2022-074-001) and reported in the Chinese Clinical Trial Register (No. ChiCTR2200061804). This study followed the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) reporting guidelines for cohort study.
Exposure
We partitioned patients into ACEI/ARB and non-ACEI/ARB groups to investigate associations between ACEI or ARB use and outcomes in hypertensive populations. The ACEI/ARB group of oral medications containing ACEIs and ARBs. Patients receiving combination therapy which includes ACEIs/ARBs, belong to this group. The non-ACEI/ARB group of oral medications included CCBs and beta blockers but did not contain ACEIs/ARBs. The exposure of interest was prescription records indicating at least 1 month of prescription.
Covariates
Baseline characteristics, demographic data, patient symptoms, medical history, and laboratory results of patients were collected, including patient age, sex, vaccination, symptoms, use of drugs, disease severity, history of immunological diseases, history of cerebrovascular disease, history of diabetes, history of coronary heart disease, history of chronic obstructive pulmonary disease, history of tumour, arrhythmias, heart failure, chronic kidney disease (CKD), oral hypoglycaemic agents (OAds), patient source, transfer to ICU or not, respiratory rate, body temperature, pulse, oxyhemoglobin saturation, blood pressure, use of aspirin, use of clopidogrel and other relevant covariates (Table 1).
Outcomes
The incidence of exacerbations and in-hospital mortality in the two groups served as the primary outcomes. Assessment of disease status followed the guidelines of SARS-CoV-2 (The Ninth Trial Version of the Chinese National Health Commission): mild type, with slight clinical symptoms but no imaging presentation of pneumonia; common type, with fever, respiratory tract, and other symptoms, imaging findings of pneumonia; severe type, with any of the following conditions: respiratory distress, respiratory frequency ≥ 30 times/minutes, finger oxygen saturation at rest ≤ 93%, or oxygenation index [PaO2/FiO2] ≤ 300 mmHg (1 mmHg = 0.133 kPa), the clinical symptoms worsened progressively, and lung imaging showed that the lesions progressed significantly > 50% within 24 ~ 48 h; critical type, with any of the following conditions: respiratory failure requiring mechanical ventilation, shock, combined with other organ failure that requires intensive care unit care and treatment. Patients were considered to have an exacerbation if their disease status changed from mild or common to severe or critical during hospitalization. The incidence of exacerbations was defined as the proportion of patients who had an exacerbation among the total patients in the group. In-hospital mortality was defined as all-cause mortality during hospitalization, jointly and separately from COVID-19 infection.
The secondary outcomes included (1) the incidence and difference of respiratory failure of patients, use of mechanical ventilation, nucleic acid conversion time (NCT), and hospitalization costs in these two groups and (2) the temporal trend of the incidence of exacerbations and in-hospital mortality in different age groups.
Statistical analysis
Continuous variables were expressed as means and standard deviations or median and interquartile ranges according to data distributions, and categorical variables were expressed as counts and percentages. Continuous, categorical, and ordinal variables were analysed with Student’s t-test, Pearson chi-square test or wilcoxon rank sum test, respectively. The inverse probability of treatment weighting (IPTW) method was used as Model 1 for propensity score weighting (PSW), which was used to account for the aforementioned confounders. The propensity score was determined using a logistic regression model with all covariates. Adequacy matching for no significant imbalance of each baseline covariate was assessed by standardized mean differences (SMDs), and |SMD| less than or equal to 0.1 means that there was no significant difference between the two groups. In subsequent analysis, unbalanced covariates were balanced by multivariable linear regression or logistic regression models.
We performed sensitivity analyses using propensity score matching (PSM) (Model 2) and multivariable regression analysis (Model 3) to evaluate the robustness of our findings. PSM was performed using the “greedy nearest-neighbour” algorithm and calculated the predicted probability of the ACEI/ARB group versus the non-ACEI/ARB group among all patients with 1:1 matching with a calliper distance of 0.2 of the standard deviation of the logit of the propensity score (Model 2). The aforementioned confounders for which the differences between the two groups were statistically significant were used to build the multivariable linear regression or logistic regression models as Model 3.
Subgroup analyses for all outcomes were carried out in the PSW cohort with patients aged 80 years and older and those aged 60 to 79 years. The Cochran-Armitage trend test was used to evaluate the significance of trends in the incidence of exacerbations and in-hospital mortality in different age groups.
All tests were two-tailed, and P < 0.05 was considered significant unless otherwise specified. Statistical analysis was performed using SAS version 9.4 (SAS Institute Inc.) and R version 4.0.4 (R Foundation for Statistical Computing).
Results
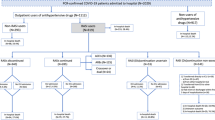
From April 2022 to July 2022, 941 patients diagnosed with laboratory-confirmed COVID-19 and taking hypertension medication regularly over 1 month were admitted to the Shanghai Fourth People`s Hospital. 78 patients were younger than 60, 1 patient had a survival time less than 48 h after admission, 47 patients were admitted with asymptomatic COVID-19, and 52 patients were admitted with severe and critical COVID-19 and were excluded according to the study protocol. Overall, 298 patients using ACEIs/ARBs and 465 patients using other drugs were included in the analysis (Fig. 1).
Baseline characteristics
Table 1 depicts the baseline characteristics of the entire cohort as well as the two groups of individuals (Table 1). Participants in the PSW and PSM included both those who used ACEIs/ARBs (n = 298) and those who did not (n = 465). There were 759 patients in the ACEI/ARB group and 760 patients in the non-ACEI/ARB group after PSW. Nearly all covariates were balanced between the two groups (SMD < 0.10), except the level of IL-6 (Table 1; Fig. 2).
Primary outcomes
Overall, the crude incidence of exacerbation in the ACEI/ARB group was 6.71% (20/298), and that in the non-ACEI/ARB group was 14.62% (68/465). There was a significantly lower incidence of exacerbation in patients using ACEIs/ARBs during hospitalization compared with patients without the use of ACEIs/ARBs (9.88% (75/760) vs. 13.23% (101/763), OR = 0.64, 95% CI for OR: 0.46–0.89, P = 0.0082, Table 2; Fig. 3) after PSW.
In the PSM cohort, the difference in exacerbation rate between the non-ACEI/ARB group and the ACEI/ARB group was not significant (6.74% (19/282) vs. 11.35% (32/282), OR = 0.56, 95% CI for OR: 0.31–1.02, P = 0.0589, Table 2; Fig. 3). The results of the multivariable logistic regression analysis were the same as those of Model 1 (OR = 0.33, 95% CI for OR: 0.18–0.63, P = 0.0008, Table 2; Fig. 3).
The in-hospital mortality of the ACEI/ARB group was 1.34% (4/298), and that of the non-ACEI/ARB group was 4.73% (22/465). In the primary analysis, patients who used ACEIs/ARBs had significantly lower in-hospital mortality than those who did not (2.12% (16/760) vs. 4.24% (32/763), OR = 0.49, 95% CI for OR: 0.27–0.89, P = 0.0201, Table 2; Fig. 3) after PSW. In Model 2, the difference in in-hospital mortality between the non-ACEI/ARB group and ACEI/ARB group was not statistically significant (1.42% (4/282) vs. 3.19% (9/282), OR = 0.44, 95% CI for OR: 0.13–1.43, P = 0.1719, Table 2; Fig. 3). Model 3 (multivariable logistic regression analysis) produced the same results as Model 1 (OR = 0.25, 95% CI for OR: 0.07–0.87, P = 0.0294, Table 2; Fig. 3).
Secondary outcomes
The incidence of mechanical ventilation in the ACEI/ARB group was 3.02% (9/298), and that in the non-ACEI/ARB group was 9.03% (42/465). Patients who used ACEIs/ARBs had a significantly lower incidence of mechanical ventilation than those who did not (4.53% (34/760) vs. 8.01% (61/763), OR = 0.54, 95% CI for OR: 0.35–0.82, P = 0.0046, Table 2; Fig. 3) after PSW. In Model 2, the difference in in-hospital mortality between the non-ACEI/ARB group and ACEI/ARB group was not statistically significant (2.84% (8/282) vs. 6.38% (18/282), OR = 0.43, 95% CI for OR: 0.18-1.00, P = 0.0505, Table 2; Fig. 3). Model 3 (multivariable logistic regression analysis) produced the same results as Model 1 (OR = 0.29, 95% CI for OR: 0.11–0.76, P = 0.0117, Table 2; Fig. 3).
The incidence of respiratory failure in the ACEI/ARB group was 3.02% (9/298), and that in the non-ACEI/ARB group was 10.32% (48/465). Patients who used ACEIs/ARBs had a significantly lower incidence of respiratory failure than those who did not (4.53% (34/760) vs. 9.18% (70/763), OR = 0.46, 95% CI for OR: 0.30–0.70, P = 0.0003, Table 2; Fig. 3) after PSW. Model 2 (2.84% (8/282) vs. 7.09% (20/282), OR = 0.38, 95% CI for OR: 0.17–0.88, P = 0.0245, Table 2; Fig. 3) and Model 3 (OR = 0.19, 95% CI for OR: 0.07–0.51, P = 0.0010, Table 2; Fig. 3) came to the same result as Model 1.
The median COVID-19 NCT of all cohorts was 14 days (interquartile range = 10–18 days). In the PSW cohort, the median NCT of the ACEI/ARB group was significantly shorter than that of the non-ACEI/ARB group (13.0 (9.0–17.0) vs. 14.0 (10.0–19.0), β=-1.23, 95% CI for β: -2.21 - -0.26, P = 0.0132, Table 2), and the same conclusion was reached in the PSM cohort (13.0 (9.0–17.0) vs. 14.0 (10.0–19.0), β=-1.33, 95% CI for β: -2.44 - -0.21, P = 0.0199, Table 2). However, the difference between the 2 groups in multivariable linear regression analysis (β=-0.91, 95% CI for β: -1.86-0.04, P = 0.0619, Table 2) was not statistically significant.
The difference in total hospitalization costs between the ACEI/ARB group and the non-ACEI/ARB group (1335.90 (912.84-2109.78) vs. 1458.21 (991.93-2376.11), β=-124.16, 95% CI for β: -476.19–227.86, P = 0.4889, Table 2) was not significant in the PSW cohort.
The incidence of exacerbation and all-cause death increased from 60 to 69 years old to ≥ 90 years old (Pexacerbation < 0.0001, Pall−cause death < 0.0001, Table 3; Fig. 4) in the PSW cohort, and the trend test of both groups came to the same result (Table 3; Fig. 4).
Subgroup analyses
In patients aged 80 years and older, the results of subgroup analyses were reasonably close to those of the primary analysis. The ACEI/ARB group had a significantly lower rate of exacerbation (10.64% (43/407) vs. 17.75% (78/441), OR = 0.56, 95% CI for OR: 0.37–0.83, P = 0.0039, Table 4), in-hospital mortality (2.93% (12/407) vs. 6.36% (28/441), OR = 0.45, 95% CI for OR: 0.23–0.90, P = 0.0235, Table 4), and incidence of respiratory failure (7.62% (31/407) vs. 12.42% (55/441), OR = 0.59, 95% CI for OR: 0.37–0.94, P = 0.0252, Table 4).
In the subgroup of patients aged 60 to 79 years, the ACEI/ARB group showed a lower incidence of mechanical ventilation (0.97% (3/353) vs. 4.76% (15/322), OR = 0.16, 95% CI for OR: 0.05–0.57, P = 0.0046, Table 4) and respiratory failure (0.97% (3/353) vs. 4.76% (15/322), OR = 0.16, 95% CI for OR: 0.05–0.57, P = 0.0046, Table 4) than the non-ACEI/ARB group.
Discussion
In this retrospective study, our results suggest that ACEI or ARB treatment could reduce the incidence of exacerbation and possibly decrease the mortality of elderly COVID-19 patients with preexisting hypertension. After subgroup analysis, the main benefit was for hypertensive patients over 80 years old. In addition, the incidence of mechanical ventilation and respiratory failure in the ACEI/ARB group was significantly lower, and the median COVID-19 NCT in the ACEI/ARB group was shorter than that in the non-ACEI/ARB group. However, there was no statistically significant difference in the average hospitalization expenses between the two groups of patients. This finding supported the continued use of RAS inhibitors in COVID-19 Omicron patients with hypertension, which provides clinical evidence for the recommendations.
The effects of ACEIs/ARBs on clinical outcomes appeared to be influenced by RAAS, as the coronavirus SARS-CoV-2 entered the cells through ACE2 [18]. Previous animal studies have shown that ACEI/ARB treatment could upregulate the expression of the ACE2 receptor [19]. ACEIs/ARBs could elevate the level of ACE2 to exacerbate SARS-Cov2 infection. As a result, prolonged ACEI/ARB therapy may worsen patients’ COVID-19 duration. However, some fundamental studies and pathophysiological studies reported opposite findings [20, 21]. Long-term use of ARBs could block the detrimental effects of angiotensin II to prevent acute pulmonary injuries, such as pulmonary vasoconstriction, pulmonary vascular permeability elevation, inflammation, and interstitial fibrosis [21]. The severity of COVID-19 is associated with interleukin-6 (IL-6), C-reactive protein (CRP), and other proinflammatory factors [22, 23]. The binding of SARS-CoV-2 to host ACE2 results in the release of proinflammatory factors, which may harm vital organs through an IL-6-induced cytokine storm [24]. Previous studies have demonstrated that early intervention to alleviate such cytokine storms could improve the clinical outcomes of severe COVID-19 [25]. Patients with hypertension who take ACEIs or ARBs may produce less angiotensin II, express more ACE2, and have significantly reduced inflammatory cytokine production [25]. Meng et al. [13] observed that patients receiving ACEI or ARB therapy had a lower rate of severe diseases and a trend towards a lower level of IL-6 in peripheral blood. We made a speculative connection between the results and the use of ACEIs/ARBs to reduce cytokine storms, which then reduced the impairment of lung function and accelerated the speed of rehabilitation. A reduction in mortality might also be associated with this. This result is consistent with a study from a retrospective study in France that concluded that in very old subjects hospitalized in geriatric settings for COVID-19, mortality was significantly lower in subjects treated with ARB or ACEI before the onset of infection [26].
The severity of COVID-19 is associated with various risk factors, such as older age, male sex, and comorbidities [5, 6, 8, 15, 27]. Hypertension, coronary heart disease, diabetes, and advanced age could also increase susceptibility to SARS-CoV-2 infection [28, 29]. According to reports, COVID-19 patients generally have a mortality rate of 1–5%, but further analysis by age reveals that the mortality rate for patients aged 80 years and older may be as high as 14.8% [27]. A WHO report showed that after adjusting for the confounding effects of age, sex, ethnicity, prior infection, vaccination status, comorbidities, effect of province and effect of public/private sector, the Omicron variant had a reduced severity and lower mortality compared with the Delta variant [30]. Substitutions in the receptor-binding domain of Omicron may be associated with the enhanced affinity of S-protein to the ACE2 receptor, which might lead to the increased transmissibility of the Omicron variant [31]. Previous studies have mostly reported the impact of ACEI/ARB drugs on early strains, but we are more concerned about whether Omicron is also affected, especially in elderly individuals. The findings of this study showed that the mortality rate for patients aged 80 years and older was 4.71%. It was slightly lower in the ACEI/ARB group, at 2.93%. However, patients older than 80 years in the aged subgroup had a higher incidence of exacerbation and mortality than patients younger than 79 years, indicating that SARS-CoV-2 infection could lead to more severe outcomes in elderly patients, especially in patients aged 80 years and older. The results suggested that elderly patients with hypertension might choose antihypertensive drugs more carefully after COVID-19 infection.
ACEIs and ARBs are both RAAS inhibitors, but it is insufficient that our study does not differentiate between ACEIs and ARBs. Lumping them together might mask specific effects of one or the other. Some scholars have proposed that ARBs might be superior to ACEs for the treatment of hypertensive COVID-19 patients [32]. Research has shown that among hypertensive patients hospitalized for COVID-19, ARBs were associated with a lower crude rate of in-hospital mortality [33]. The differences between ACEIs and ARBs require further research.
Overall, these findings suggested potential beneficial effects observed with continued use of ACEI/ARB therapy in elderly COVID-19 Omicron BA.2 patients with hypertension. Other studies should also investigate whether ACEIs/ARBs were continued during hospitalization. Findings should be confirmed using other populations and study designs, including randomized controlled trials in both the general and younger populations.
Limitations
As a retrospective study, there were several limitations in this study. First, due to the study’s retrospective design, not all confounding factors could be eliminated. BMI could be a key covariate, but the data were incomplete. Second, the study is a single-centre retrospective study. This design inherently has limitations in terms of generalizability. Third, due to insufficient data, patients could not be stratified based on when they used ACEIs/ARBs. Although various models could be used to adjust the confounding variables, other variables that could explain the severity of COVID-19 were possibly overlooked in this study. Finally, this study period is short, and we cannot be sure that the findings are not influenced by seasonal or other temporal factors. Although the findings of this study demonstrated that chronic exposure to ACEIs/ARBs was associated with better outcomes, the influences of these limitations should be considered.
Conclusion
This study provided support for the continued use of ACEIs or ARBs by clinicians because they might slow the progression of mild and regular COVID-19 to severe COVID-19. The use of ACEIs/ARBs could benefit patients aged 60 years or older, especially patients aged 80 years or older.
Data Availability
The datasets used or analysed during the current study are available from the corresponding author on reasonable request.
References
Beyerstedt S, Casaro EB, Rangel ÉB. COVID-19: angiotensin-converting enzyme 2 (ACE2) expression and tissue susceptibility to SARS-CoV-2 Infection. Eur J Clin Microbiol Infect Dis. 2021;40(5):905–19. https://doi.org/10.1007/s10096-020-04138-6.
Brevini T, Maes M, Webb GJ, et al. FXR inhibition may protect from SARS-CoV-2 Infection by reducing ACE2. Nature. 2023;615(7950):134–42. https://doi.org/10.1038/s41586-022-05594-0.
Kovell LC, Ahmed HM, Misra S, et al. US Hypertension management guidelines: a review of the recent past and recommendations for the future. J Am Heart Assoc. 2015;4. https://doi.org/10.1161/JAHA.115.002315.
Flack JM, Adekola B. Blood pressure and the new ACC/AHA Hypertension guidelines. Trends Cardiovasc Med. 2020;30:160–4. https://doi.org/10.1016/j.tcm.2019.05.003.
Li W, Moore MJ, Vasilieva N, et al. Angiotensin-converting enzyme 2 is a functional receptor for the SARS coronavirus[J]. Nature. 2003;426:450–4. https://doi.org/10.1038/nature02145
Xu X, Chen P, Wang J, et al. Evolution of the novel coronavirus from the ongoing Wuhan outbreak and modeling of its spike protein for risk of human transmission. Sci China Life Sci. 2020;63:457–60. https://doi.org/10.1007/s11427-020-1637-5.
Ferrario CM, Jessup J, Chappell MC, et al. Effect of angiotensin-converting enzyme inhibition and angiotensin II receptor blockers on cardiac angiotensin-converting enzyme 2. Circulation. 2005;111:2605–10. https://doi.org/10.1161/CIRCULATIONAHA.104.510461.
Liu Y, Yang Y, Zhang C, et al. Clinical and biochemical indexes from 2019-nCoV infected patients linked to viral loads and lung injury. Sci China Life Sci. 2020;63:364–74. https://doi.org/10.1007/s11427-020-1643-8.
Grover A, Oberoi M. A systematic review and meta-analysis to evaluate the clinical outcomes in COVID-19 patients on angiotensin-converting enzyme inhibitors or angiotensin receptor blockers. Eur Heart J Cardiovasc Pharmacother. 2021;7:148–57. https://doi.org/10.1093/ehjcvp/pvaa064.
Richardson S, Hirsch JS, Narasimhan M, et al. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area [published correction appears in JAMA. 2020;323(20):2098]. JAMA. 2020;323(20):2052–9. https://doi.org/10.1001/jama.2020.6775.
Meng J, Xiao G, Zhang J, et al. Renin-angiotensin system inhibitors improve the clinical outcomes of COVID-19 patients with Hypertension. Emerg Microbes Infect. 2020;9:757–60. https://doi.org/10.1080/22221751.2020.1746200.
Zhang P, Zhu L, Cai J, et al. Association of inpatient use of angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers with mortality among patients with Hypertension hospitalized with COVID-19 [published correction appears in Circ Res. 2020;127(6):e147. Rohit, Loomba [corrected to Loomba, Rohit]]. Circ Res. 2020;126(12):1671–81. https://doi.org/10.1161/CIRCRESAHA.120.317134.
Li J, Wang X, Chen J, Zhang H, Deng A. Association of renin-angiotensin system inhibitors with severity or risk of death in patients with Hypertension hospitalized for coronavirus Disease 2019 (COVID-19) Infection in Wuhan, China. JAMA Cardiol. 2020;5:825–30. https://doi.org/10.1001/jamacardio.2020.1624.
Bauer AZ, Gore R, Sama SR, et al. Hypertension, medications, and risk of severe COVID-19: a Massachusetts community-based observational study. J Clin Hypertens (Greenwich). 2021;23(1):21–7. https://doi.org/10.1111/jch.14101.
Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. The Lancet. 2020;395:1054–62. https://doi.org/10.1016/S0140-6736(20)30566-3.
Ling Y, Lu G, Liu F, et al. The Omicron BA.2.2.1 subvariant drove the wave of SARS-CoV-2 outbreak in Shanghai during spring 2022. Cell Discov. 2022;8(1):97. https://doi.org/10.1038/s41421-022-00468-1. Published 2022 Sep 27.
Ao Y, Li J, Wei Z, et al. Clinical and virological characteristics of SARS-CoV-2 Omicron BA.2.2 variant outbreaks during April to May, 2022, Shanghai, China. J Infect. 2022;85(5):573–607. https://doi.org/10.1016/j.jinf.2022.07.027.
Vaduganathan M, Vardeny O, Michel T et al. Renin-angiotensin-aldosterone system inhibitors in patients with Covid-19. N Engl J Med. 2020;382(17):1653–9. https://doi.org/10.1056/NEJMsr2005760
Danser AHJ, Epstein M, Batlle D. Renin-angiotensin system blockers and the COVID-19 pandemic: at present there is no evidence to abandon renin-angiotensin system blockers. Hypertension. 2020;75:1382–5. https://doi.org/10.1161/HYPERTENSIONAHA.120.15082.
Battistoni A, Volpe M. Might renin-angiotensin systemblockers play a role in the COVID-19 pandemic? Eur Heart J Cardiovasc Pharmacother. 2020;6:248–51. https://doi.org/10.1093/EHJCVP/PVAA030.
Yang G, Tan Z, Zhou L, et al. Effects of angiotensin II receptor blockers and ACE (angiotensin-converting enzyme) inhibitors on virus Infection, inflammatory status, and clinical outcomes in patients with COVID-19 and Hypertension: a single-center retrospective study. Hypertension. 2020;76:51–8. https://doi.org/10.1161/HYPERTENSIONAHA.120.15143.
Gao Y, Li T, Han M, et al. Diagnostic utility of clinical laboratory data determinations for patients with the severe COVID-19. J Med Virol. 2020;92:791–6. https://doi.org/10.1002/jmv.25770.
Bao J, Li C, Zhang K, et al. Comparative analysis of laboratory indexes of severe and non-severe patients infected with COVID-19. Clin Chim Acta. 2020;509:180–94. https://doi.org/10.1016/j.cca.2020.06.009.
Iwasaki M, Saito J, Zhao H, et al. Inflammation triggered by sars-cov-2 and ace2 augment drives multiple organ failure of severe covid-19: molecular mechanisms and implications. Inflammation. 2021;44:13–34. https://doi.org/10.1007/s10753-020-01337-3.
Ye Q, Wang B, Mao J. The pathogenesis and treatment of the ‘Cytokine Storm’’ in COVID-19’. J Infect. 2020;80:607–13. https://doi.org/10.1016/j.jinf.2020.03.037.
Genet B, Vidal JS, Cohen A, et al. COVID-19 in-hospital mortality and use of renin-angiotensin system blockers in geriatrics patients. J Am Med Dir Assoc. 2020;21:1539–45. https://doi.org/10.1016/j.jamda.2020.09.004.
Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus Disease 2019 (COVID-19) outbreak in China: summary of a report of 72314 cases from the Chinese center for Disease control and prevention. JAMA. 2020;323:1239–42. https://doi.org/10.1001/jama.2020.2648.
Fang L, Karakiulakis G, Roth M. Are patients with Hypertension and Diabetes Mellitus at increased risk for COVID-19 Infection? The Lancet Respiratory. 2020;8:e21. https://doi.org/10.1016/S2213.
Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. The Lancet. 2020;395:497–506. https://doi.org/10.1016/S0140-6736(20)30183-5.
Who. Severity of Disease associated with Omicron variant as compared with Delta variant in hospitalized patients with suspected or confirmed SARS-CoV-2 Infection. In: World Health Organization; 2022.
Chen KK, Tsung-Ning Huang D, Huang LM. SARS-CoV-2 variants - evolution, spike protein, and vaccines. Biomed J. 2022;45(4):573–9. https://doi.org/10.1016/j.bj.2022.04.006.
Zhao HJ, Li Y, Wang DY, Yuan HT. ARB might be superior to ACEI for treatment of hypertensive COVID-19 patients. J Cell Mol Med. 2021;25(23):11031–4. https://doi.org/10.1111/jcmm.17051.
Hamada S, Suzuki T, Tokuda Y, et al. Comparing clinical outcomes of ARB and ACEi in patients hospitalized for acute COVID-19. Sci Rep. 2023;13(1):11810. https://doi.org/10.1038/s41598-023-38838-8. Published 2023 Jul 21.
Acknowledgements
The authors of this study would like to thank all the medical personnel involved in the diagnosis and treatment of patients in the Shanghai Fourth People’s Hospital; we also thank Zhenzhen Chen, Tongtong Jia, Meiling Zhang (Department of pain medicine, Fourth People’s Hospital, Shanghai, China), Sijia Yuan and Lipeng Wang (Department of Information, Fourth People’s Hospital, Shanghai, China) for their guidance during information collection.
Funding
This work was partly supported by the National Natural Science Foundation of China [grant number 81971042], the Key Supported Clinical Specialties of Hongkou District Health Committee [grant number HKZK2020A06], the Discipline Boosting Program of Shanghai Fourth People’s Hospital (SY-XKZT-2020-1013), the Three-Year Action Plan for Strengthening Public Health System in Shanghai(2020–2022)Subject Chief Scientist(GWV-10.2-XD05), and Pilot Program of Naval Medical University (Cheng WU).
Author information
Authors and Affiliations
Contributions
L.X. and C.W. conceptualized and designed the study, and reviewed and revised the manuscript. Z.Z., Y.W., and S.W. drafted the initial manuscript, prepared figures and tables, designed the data collection instruments, collected data, carried out the initial analyses, and reviewed. H.C. and Z.W. revised the manuscript and supervised data collection, and critically reviewed the manuscript for important intellectual content. All authors approved the final manuscript as submitted and agreed to be accountable for all aspects of the work. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Ethics Committee of the Shanghai Fourth People’s hospital (No. 2022-074-001) and reported in the Chinese Clinical Trial Register (No. ChiCTR2200061804).
The Ethics Committee of the Shanghai Fourth People’s hospital waived the need of informed consent.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Zhang, Z., Wu, S., Wang, Z. et al. Long-term oral ACEI/ARB therapy is associated with disease severity in elderly COVID-19 omicron BA.2 patients with hypertension. BMC Infect Dis 23, 882 (2023). https://doi.org/10.1186/s12879-023-08913-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12879-023-08913-6