Abstract
Background
Colonisation by multidrug-resistant (MDR) bacteria is a global health issue. The identification of patients with a higher risk of colonisation is essential. Patients admitted to internal medicine services might represent a vulnerable population with a high risk of colonisation. This study was the first to assess social and clinical variables associated with a higher risk of perianal colonisation by MDR bacteria in a Spanish cohort of patients admitted to internal medicine service.
Methods
Patients admitted to an internal medicine service during 12 months of recruitment (1 March 2022 to 1 March 2023) were included in the study. Perianal swabs were performed at admission to identify the presence of MDR bacteria. Social and clinical variables were collected following a directed acyclic graph. A cluster analysis was performed to identify clinical profiles of higher risk. Bivariate analyses and multivariable logistic regression models were fitted to identify potential predictors of MDR bacteria colonisation.
Results
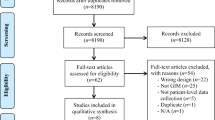
A total of 245 patients, according to the required sample size, were included. Of them, 46 (18.8%) were colonised by MDR bacteria in perianal swabs. Female sex, age > 80 years, dependency on activities of daily living, cognitive deterioration and living in long-term care facilities constituted the highest risk clinical profile. After adjustments, living in long-term care facilities and malnutrition remained the main risk factors identified.
Conclusion
Patients admitted to internal medicine services presented a high frequency of perianal colonisation by MDR bacteria. Social and clinical variables associated with bio-psycho-social susceptibility were associated with colonisation. Special surveillance is needed in internal medicine services to control the transmission.




Similar content being viewed by others
Data availability
Anonymous raw data from this study can be shared upon reasonable request from the corresponding author.
References
McEwen SA, Collignon PJ. Antimicrobial resistance: a one health perspective. Microbiol Spectr. 2018. https://doi.org/10.1128/microbiolspec.ARBA-0009-2017.
Rivera-Izquierdo M, Láinez-Ramos-Bossini AJ, Rivera-Izquierdo C, López-Gómez J, Fernández-Martínez NF, Redruello-Guerrero P, et al. OXA-48 carbapenemase-producing enterobacterales in spanish hospitals: an updated comprehensive review on a rising antimicrobial resistance. Antibiotics (Basel). 2021;10:89.
Sociedad Española de Medicina Preventiva, Salud Pública y Gestión Sanitaria. EPINE-EPPS [Prevalence Study of the Nosocomial Infections in Spain], Study, nº32 https://epine.es/api/documento-publico/2022%20EPINE%20Informe%20España%2020221201.pdf/reports-esp; 2022 Accessed 28 June 2023.
Junta de Andalucía. SVEA [Epidemiological Surveillance System of Andalusia], https://www.repositoriosalud.es/handle/10668/22621; 2022 Accessed 28 June 2023.
Dolci G, Burastero GJ, Paglia F, Cervo A, Meschiari M, Guaraldi G, et al. Epidemiology and prevention of early infections by multi-drug-resistant organisms in adults undergoing liver transplant: a narrative review. Microorganisms. 2023;11:1606.
Spanish Government. National Antibiotic Resistance Plan, 2023 [online]. Available from: https://www.aemps.gob.es/tag/pran/# Accessed 28 June 2023.
Carvalho-Brugger S, Miralbés Torner M, Jiménez Jiménez G, Badallo O, Álvares Lerma F, Trujillano J, et al. Preventive isolation criteria for the detection of multidrug-resistant bacteria in patients admitted to the Intensive Care Unit: A multicenter study within the Zero Resistance program. Med Intensiva (Engl Ed) 2023;S2173-5727(23)00057-7
Rivera-Izquierdo M, Benavente-Fernández A, López-Gómez J, Láinez-Ramos-Bossini AJ, Rodríguez-Camacho M, Valero-Ubierna MDC, et al. Prevalence of multi-resistant microorganisms and antibiotic stewardship among hospitalized patients living in residential care homes in spain: a cross-sectional study. Antibiotics (Basel). 2020;9:324.
European Society of Clinical Microbiology and Infectious Diseases. European Committee on Antimicrobial Susceptibility Testing (EUCAST), 2022 [online]. Available at: https://www.eucast.org/eucastguidancedocuments Accessed July 2023.
Timler M, Timler W, Bednarz A, Zakonnik Ł, Kozłowski R, Timler D, et al. Identification and preliminary hierarchisation of selected risk factors for carbapenemase-producing Enterobacteriaceae (CPE) colonisation: a prospective study. Int J Environ Res Public Health. 2023;20:1960.
Campos-Madueno EI, Moradi M, Eddoubaji Y, Shahi F, Moradi S, Bernasconi OJ, et al. Intestinal colonization with multidrug-resistant Enterobacterales: screening, epidemiology, clinical impact, and strategies to decolonize carriers. Eur J Clin Microbiol Infect Dis. 2023;42:229–54.
Callejón Fernández M, Madueño Alonso A, Abreu Rodríguez R, Aguirre-Jaime A, Castro Hernández MB, Ramos-Real MJ, et al. Risk factors for colonization by carbapenemase-producing bacteria in Spanish long-term care facilities: a multicentre point-prevalence study. Antimicrob Resist Infect Control. 2022;11:163.
Andalusian Health Service. Care of the pluripathological patient [online]. Available from: https://www.sspa.juntadeandalucia.es/servicioandaluzdesalud/profesionales/cartera-de-servicios/atencion-primaria/i-area-de-atencion-la-persona/2-atencion-especifica/22-atencion-problemas-cronicos/227-paciente-pluripatologico Accessed 28 June 2023.
Royston P. Multiple imputation of missing values: further update of ice, with an emphasis on categorical variables. Stata J. 2009;9:466–77.
Van Buuren S. Multiple imputation of discrete and continuous data by fully conditional specification. Stat Methods Med Res. 2007;16:219–42.
White IR, Royston P, Wood AM. Multiple imputation using chained equations: issues and guidance for practice. Stat Med. 2011;30:377–99.
González-Montalvo JI, Ramírez-Martín R, Menéndez Colino R, Alarcón T, Tarazona-Santabalbina FJ, Martínez-Velilla N, et al. Geriatría transversal. Un reto asistencial para el siglo xxi [Cross-speciality geriatrics: a health-care challenge for the 21st century]. Rev Esp Geriatr Gerontol. 2020;55:84–97.
Veronese N, Custodero C, Demurtas J, Smith L, Barbagallo M, Maggi S, et al. Comprehensive geriatric assessment in older people: an umbrella review of health outcomes. Age Ageing. 2022;51:afac104.
Parker SG, McCue P, Phelps K, et al. What is comprehensive geriatric assessment (CGA)? An umbrella review. Age Ageing. 2018;47:149–55.
Tacconelli E, Mazzaferri F, de Smet AM, Bragantini D, Eggimann P, Huttner BD, et al. ESCMID-EUCIC clinical guidelines on decolonization of multidrug-resistant Gram-negative bacteria carriers. Clin Microbiol Infect. 2019;25:807–17.
Merrick B, Sergaki C, Edwards L, Moyes DL, Kertanegara M, Prossomariti D, et al. Modulation of the Gut microbiota to control antimicrobial resistance (AMR)—a narrative review with a focus on faecal microbiota transplantation (FMT). Infect Dis Rep. 2023;15:238–54.
Gargiullo L, Del Chierico F, D’Argenio P, Putignani L. Gut microbiota modulation for multidrug-resistant organism decolonization: present and future perspectives. Front Microbiol. 2019;10:1704.
Bilsen MP, Lambregts MMC, van Prehn J, Kuijper EJ. Faecal microbiota replacement to eradicate antimicrobial resistant bacteria in the intestinal tract - a systematic review. Curr Opin Gastroenterol. 2022;38:15–25.
Macareño-Castro J, Solano-Salazar A, Dong LT, Mohiuddin M, Espinoza JL. Fecal microbiota transplantation for carbapenem-resistant Enterobacteriaceae: a systematic review. J Infect. 2022;84:749–59.
Pérez-Nadales E, Cano Á, Recio M, Artacho MJ, Guzmán-Puche J, Doblas A, et al. Randomised, double-blind, placebo-controlled, phase 2, superiority trial to demonstrate the effectiveness of faecal microbiota transplantation for selective intestinal decolonisation of patients colonised by carbapenemase-producing Klebsiella pneumoniae (KAPEDIS). BMJ Open. 2022;12: e058124.
Martinez JA. Efficacy of a probiotic or fecal microbiota transplantation (FMT) on the eradication of rectal multidrug-resistant gram-negative Bacilli (MDR-GNB) Carriage (PROFTMDECOL). Study Record | Beta ClinicalTrials.gov [Internet]. NCT04431934. Available from: https://clinicaltrials.gov/study/NCT04431934?tab=history. Accessed 28 June 2023.
Martin EM, Bryant B, Grogan TR, Rubin ZA, Russell DL, Elashoff D, Uslan DZ. Noninfectious hospital adverse events decline after elimination of contact precautions for MRSA and VRE. Infect Control Hosp Epidemiol. 2018;39:788–96.
Acknowledgements
We wish to acknowledge all personnel of internal medicine service of the Hospital Universitario San Cecilio for their predisposition, for the collecting of rectal swab samples and for the facilities they have provided for the correct development of this work.
Funding
No funding.
Author information
Authors and Affiliations
Contributions
MCV, AB, JJJ and MR designed the study. JPR and MR performed the statistical analysis. MCV and MR wrote the first draft of the manuscript. MCV, AB, JPR, FM, JL, SF, NC, CG, JJJ and MR collected the raw data and critically revised the design of the study. All authors reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have completed the ICMJE uniform disclosure form at https://www.icmje.org/coi_disclosure.pdf and declare: no support from any organisation for the submitted work.
Ethical approval and consent to participate
This study was approved by the Provincial Ethical Committee of Granada on 22 February 2022, code MR_161121.
Consent for publication
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
del Carmen Valero-Ubierna, M., Benavente-Fernández, A., Pérez de Rojas, J. et al. Social and clinical predictors of perianal colonisation by multidrug-resistant bacteria for geriatric patients in the internal medicine service. Infection 52, 231–241 (2024). https://doi.org/10.1007/s15010-023-02153-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-023-02153-1