Abstract
Background
The co-occurrence of physical inactivity and poor mental health in the college student population can lead to chronic health issues that have negative short-term effects (e.g., academic success). Poor mental health is associated with long-term conditions (e.g., obesity, serious mental illness) that are linked to premature mortality. The purpose of this study was to examine the information–motivation–behavioral (IMB) skills model and evaluate its ability to explain the variance in the use of exercise prescription in mental health treatment.
Method
Mental health professionals (MHPs) (n = 255) were recruited from college counseling centers in the USA. Structural equation modeling was used to examine the relationship between the predictor variables of information (exercise knowledge and benefits of exercise), motivation (personal beliefs, perceived barriers, and organizational support), and behavioral skills (self-efficacy), and the outcome variable of exercise prescription (i.e., brief counseling and referral for exercise).
Results
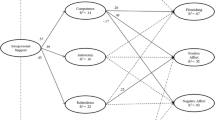
The predictors accounted for 23% of the variance in exercise prescription (p = .001). Organizational support had a significant direct effect on exercise prescription (β = 0.27, p = .05). Personal beliefs (β = 0.96, p = .05) and organizational support (β = 0.31, p = .04) had significant direct effects on self-efficacy for prescribing exercise. MHP personal exercise behavior was associated with exercise prescription.
Conclusion
MHPs may be willing to support physical activity promotion and exercise prescription, but organizational structures are critical to enhance and sustain the delivery of this adjunctive therapy. The personal exercise history of MHPs may be an important consideration for behavior change interventions. The development and validation of scales are important considerations for future intervention study design.



Similar content being viewed by others
Data Availability
Data is available upon request from the corresponding author.
References
National Institute of Mental Health. National Institute of Mental Health Statistics. 2019. https://www.nimh.nih.gov/health/statistics/mental-illness.shtml. Accessed 12 Mar 2023.
Vigo D, Thornicroft G, Atun R. Estimating the true global burden of mental illness. Lancet Psychiatry. 2016;3(2):171–8. https://doi.org/10.1016/S2215-0366(15)00505-2.
Bradshaw T, Pedley R. Evolving role of mental health nurses in the physical health care of people with serious mental health illness: physical health and psychosis. Int J Ment Health Nurs. 2012;21(3):266–73. https://doi.org/10.1111/j.1447-0349.2012.00818.x.
Scott D, Happell B. The high prevalence of poor physical health and unhealthy lifestyle behaviours in individuals with severe mental illness. Issues Ment Health Nurs. 2011;32(9):589–97. https://doi.org/10.3109/01612840.2011.569846.
Walker ER, McGee RE, Druss BG. Mortality in mental disorders and global disease burden implications: a systematic review and meta-analysis. JAMA Psychiat. 2015;72(4):334–41. https://doi.org/10.1001/jamapsychiatry.2014.2502.
Rosenbaum S, Hobson-Powell A, Davison K, et al. The role of sport, exercise, and physical activity in closing the life expectancy gap for people with mental illness: an international consensus statement by exercise and sports science Australia, American College of Sports Medicine, British Association of Sport and Exercise Science, and Sport and Exercise Science New Zealand. Transl J Am Coll Sports Med. 2018;3(10):72–3. https://doi.org/10.1249/TJX.0000000000000061.
Ashdown-Franks G, Firth J, Carney R, et al. Exercise as medicine for mental and substance use disorders: a meta-review of the benefits for neuropsychiatric and cognitive outcomes. Sports Med. 2020;50(1):151–70. https://doi.org/10.1007/s40279-019-01187-6.
Rosenbaum S, Vancampfort D, Steel Z, Newby J, Ward PB, Stubbs B. Physical activity in the treatment of post-traumatic stress disorder: a systematic review and meta-analysis. Psychiatry Res. 2015;230(2):130–6. https://doi.org/10.1016/j.psychres.2015.10.017.
Czosnek L, Lederman O, Cormie P, Zopf E, Stubbs B, Rosenbaum S. Health benefits, safety and cost of physical activity interventions for mental health conditions: a meta-review to inform translation efforts. Ment Health Phys Act. 2019;16:140–51. https://doi.org/10.1016/j.mhpa.2018.11.001.
Kvam S, Kleppe CL, Nordhus IH, Hovland A. Exercise as a treatment for depression: a meta-analysis. J Affect Disord. 2016;202:67–86. https://doi.org/10.1016/j.jad.2016.03.063.
Weinstein AA, Koehmstedt C, Kop WJ. Mental health consequences of exercise withdrawal: a systematic review. Gen Hosp Psychiatry. 2017;49:11–8. https://doi.org/10.1016/j.genhosppsych.2017.06.001.
Glowacki K, Duncan MJ, Gainforth H, Faulkner G. Barriers and facilitators to physical activity and exercise among adults with depression: a scoping review. Ment Health Phys Act. 2017;13:108–19. https://doi.org/10.1016/j.mhpa.2017.10.001.
American College of Sports Medicine, Liguori G, Feito Y, Fountaine C, Roy B, editors. ACSM’s Guidelines for Exercise Testing and Prescription. 11th ed. Wolters Kluwer; 2021.
American College of Sports Medicine. What is exercise is medicine: a global health initiative. 2022. https://www.exerciseismedicine.org/about-eim/. Accessed 16 Mar 2023.
Adhikari K, Teare GF, Belon AP, Lee B, Kim MO, Nykiforuk C. Screening, brief intervention, and referral to treatment for tobacco consumption, alcohol misuse, and physical inactivity: an equity-informed rapid review. Public Health. 2024;226:237–47. https://doi.org/10.1016/j.puhe.2023.11.001.
Waite I, Grant D, Mayes J, Greenwood S. Can a brief behavioural change intervention encourage hospital patients with low physical activity levels to engage and initiate a change in physical activity behaviour? Physiotherapy. 2020;108:22–8. https://doi.org/10.1016/j.physio.2020.04.002.
Glowacki K, Weatherson K, Faulkner G. Barriers and facilitators to health care providers’ promotion of physical activity for individuals with mental illness: a scoping review. Ment Health Phys Act. 2019;16:152–68. https://doi.org/10.1016/j.mhpa.2018.10.006.
Fisher WA, Fisher JD, Harman J. The information-motivation-behavioral skills model: a general social psychological approach to understanding and promoting health behavior. In: Suls J, Wallston KA, editors. Social Psychological Foundations of Health and Illness. Blackwell Publishing Ltd; 2003. p. 82–106. https://doi.org/10.1002/9780470753552.ch4.
Misovich SJ, Martinez T, Fisher JD, Bryan A, Catapano N. Predicting breast self-examination: a test of the information-motivation-behavioral skills model. J Appl Soc Psychol. 2003;33(4):775–90. https://doi.org/10.1111/j.1559-1816.2003.tb01924.x.
Chang SJ, Choi S, Kim SA, Song M. Intervention strategies based on information-motivation-behavioral skills model for health behavior change: a systematic review. Asian Nurs Res. 2014;8(3):172–81. https://doi.org/10.1016/j.anr.2014.08.002.
Jia X, Zhou S, Luo D, Zhao X, Zhou Y, Cui Y. Effect of pharmacist-led interventions on medication adherence and inhalation technique in adult patients with asthma or COPD: a systematic review and meta-analysis. J Clin Pharm Ther. 2020;45(5):904–17. https://doi.org/10.1111/jcpt.13126.
Dai Z, Jing S, Liu X, et al. Development and validation of the diabetic self-management scale based on information-motivation-behavioral skills theory. Front Public Health. 2023;11:1109158. https://doi.org/10.3389/fpubh.2023.1109158.
Hackler D, Pinho V, McKinnon K. IMB Model in practice: social workers’ intentions to change their practice following HIV mental health training. Soc Work Health Care. 2013;52(5):483–97. https://doi.org/10.1080/00981389.2012.750258.
Walsh JL, Petroll AE. Factors related to pre-exposure prophylaxis prescription by U.S. primary care physicians. Am J Prev Med. 2017;52(6):e165–72. https://doi.org/10.1016/j.amepre.2017.01.025.
Crisford P, Winzenberg T, Venn A, Schultz M, Aitken D, Cleland V. Factors associated with physical activity promotion by allied and other non-medical health professionals: a systematic review. Patient Educ Couns. 2018;101(10):1775–85. https://doi.org/10.1016/j.pec.2018.05.011.
Hébert ET, Caughy MO, Shuval K. Primary care providers’ perceptions of physical activity counselling in a clinical setting: a systematic review. Br J Sports Med. 2012;46(9):625–31. https://doi.org/10.1136/bjsports-2011-090734.
Huijg JM, Gebhardt WA, Verheijden MW, et al. Factors influencing primary health care professionals’ physical activity promotion behaviors: a systematic review. Int J Behav Med. 2015;22(1):32–50. https://doi.org/10.1007/s12529-014-9398-2.
Vancampfort D, Stanton R, Probst M, et al. A quantitative assessment of the views of mental health professionals on exercise for people with mental illness: perspectives from a low-resource setting. Afr Health Sci. 2019;19(2):2172–82. https://doi.org/10.4314/ahs.v19i2.
Way K, Kannis-Dymand L, Lastella M, Lovell GP. Mental health practitioners’ reported barriers to prescription of exercise for mental health consumers. Ment Health Phys Act. 2018;14:52–60. https://doi.org/10.1016/j.mhpa.2018.01.001.
Newsome AM. Exercise promotion practices among mental health professionals: a scoping review. Issues Ment Health Nurs. 2023;44(7):591–601. https://doi.org/10.1080/01612840.2023.2212770.
Stanton R, Happell B. Exercise for mental illness: a systematic review of inpatient studies: exercise and mental illness. Int J Ment Health Nurs. 2014;23(3):232–42. https://doi.org/10.1111/inm.12045.
Soundy A, Stubbs B, Probst M, Hemmings L, Vancampfort D. Barriers to and facilitators of physical activity among persons with schizophrenia: a survey of physical therapists. Psychiatr Serv. 2014;65(5):693–6. https://doi.org/10.1176/appi.ps.201300276.
Burton NW, Pakenham KI, Brown WJ. Are psychologists willing and able to promote physical activity as part of psychological treatment? Int J Behav Med. 2010;17(4):287–97. https://doi.org/10.1007/s12529-010-9087-8.
Happell B, Scott D, Platania-Phung C, Nankivell J. Nurses’ views on physical activity for people with serious mental illness. Ment Health Phys Act. 2012;5(1):4–12. https://doi.org/10.1016/j.mhpa.2012.02.005.
Kinnafick FE, Papathomas A, Regoczi D. Promoting exercise behaviour in a secure mental health setting: healthcare assistant perspectives. Int J Ment Health Nurs. 2018;27(6):1776–83. https://doi.org/10.1111/inm.12484.
Radovic S, Melvin GA, Gordon MS. Clinician perspectives and practices regarding the use of exercise in the treatment of adolescent depression. J Sports Sci. 2018;36(12):1371–7. https://doi.org/10.1080/02640414.2017.1383622.
Stanton R, Reaburn P, Happell B. Barriers to exercise prescription and participation in people with mental illness: the perspectives of nurses working in mental health: barriers to exercise. J Psychiatr Ment Health Nurs. 2015;22(6):440–8. https://doi.org/10.1111/jpm.12205.
Verhaeghe N, De Maeseneer J, Maes L, Van Heeringen C, Annemans L. Health promotion in mental health care: perceptions from patients and mental health nurses. J Clin Nurs. 2013;22(11–12):1569–78. https://doi.org/10.1111/jocn.12076.
Worsley JD, Harrison P, Corcoran R. Bridging the gap: exploring the unique transition from home, school or college into university. Front Public Health. 2021;9:634285. https://doi.org/10.3389/fpubh.2021.634285.
Ebert DD, Buntrock C, Mortier P, et al. Prediction of major depressive disorder onset in college students. Depress Anxiety. 2019;36(4):294–304. https://doi.org/10.1002/da.22867.
Cornelius LR, van der Klink JJL, de Boer MR, Brouwer S, Groothoff JW. High prevalence of early onset mental disorders among long-term disability claimants. Disabil Rehabil. 2016;38(6):520–7. https://doi.org/10.3109/09638288.2015.1046566.
Sharp J, Theiler S. A review of psychological distress among university students: pervasiveness, implications and potential points of intervention. Int J Adv Couns. 2018;40(3):193–212. https://doi.org/10.1007/s10447-018-9321-7.
Duffy ME, Twenge JM, Joiner TE. Trends in mood and anxiety symptoms and suicide-related outcomes among U.S. undergraduates, 2007–2018: evidence from two national surveys. J Adolesc Health. 2019;65(5):590–8. https://doi.org/10.1016/j.jadohealth.2019.04.033.
American College Health Association. American College Health Association-National College Health Assessment III: Undergraduate Student Reference Group Executive Summary Spring 2022. American College Health Association; 2022.
Gorman K, Bruns C, Chin C, et al. The Association for University and College Counseling Center Directors Annual Survey: 2022. 2022. https://www.aucccd.org/assets/documents/Survey/2021-22%20Annual%20Survey%20Report%20Public%20FINAL.pdf. Accessed 13 Mar 2023.
Benton SA, Robertson JM, Tseng WC, Newton FB, Benton SL. Changes in counseling center client problems across 13 years. Prof Psychol Res Pract. 2003;34(1):66–72. https://doi.org/10.1037/0735-7028.34.1.66.
Bland HW, Melton B, Bigham L, Welle PD. Quantifying the impact of physical activity on stress tolerance in college students. Coll Stud J. 2014;48:559–68.
Rodríguez-Romo G, Acebes-Sánchez J, García-Merino S, Garrido-Muñoz M, Blanco-García C, Diez-Vega I. Physical activity and mental health in undergraduate students. Int J Environ Res Public Health. 2022;20(1):195. https://doi.org/10.3390/ijerph20010195.
Snedden TR, Scerpella J, Kliethermes SA, et al. Sport and physical activity level impacts health-related quality of life among collegiate students. Am J Health Promot. 2019;33(5):675–82. https://doi.org/10.1177/0890117118817715.
Kwan MY, Cairney J, Faulkner GE, Pullenayegum EE. Physical activity and other health-risk behaviors during the transition into early adulthood. Am J Prev Med. 2012;42(1):14–20. https://doi.org/10.1016/j.amepre.2011.08.026.
Winpenny EM, Smith M, Penney T, et al. Changes in physical activity, diet, and body weight across the education and employment transitions of early adulthood: a systematic review and meta-analysis. Obes Rev Off J Int Assoc Study Obes. 2020;21(4): e12962. https://doi.org/10.1111/obr.12962.
Ferreira Silva RM, Mendonça CR, Azevedo VD, Raoof Memon A, Noll PRES, Noll M. Barriers to high school and university students’ physical activity: a systematic review. PLoS ONE. 2022;17(4):e0265913. https://doi.org/10.1371/journal.pone.0265913.
Newsome A, Gilliard T, Phillips A, Dedrick R. Understanding the perceptions of sedentary college students’ engagement in physical activity: application of the theory of planned behavior. J Am Coll Health. 2021;1–10. https://doi.org/10.1080/07448481.2021.1998069.
Buckworth J, Granello DH, Belmore J. Incorporating personality assessment into counseling to help college students adopt and maintain exercise behaviors. J Coll Couns. 2002;5(1):15–25. https://doi.org/10.1002/j.2161-1882.2002.tb00203.x.
Karvinen K, Balneaves L, Courneya K, Perry B, Truant T, Vallance J. Evaluation of online learning modules for improving physical activity counseling skills, practices, and knowledge of oncology nurses. Oncol Nurs Forum. 2017;44(6):729–38. https://doi.org/10.1188/17.ONF.729-738.
Lent RW, Hill CE, Hoffman MA. Development and validation of the counselor activity self-efficacy scales. J Couns Psychol. 2003;50(1):97–108. https://doi.org/10.1037/0022-0167.50.1.97.
Stanton R, Happell B, Reaburn P. The development of a questionnaire to investigate the views of health professionals regarding exercise for the treatment of mental illness. Ment Health Phys Act. 2014;7(3):177–82. https://doi.org/10.1016/j.mhpa.2014.06.001.
Romain AJ, Trottier A, Karelis AD, Abdel-Baki A. Do mental health professionals promote a healthy lifestyle among individuals experiencing serious mental illness? Issues Ment Health Nurs. 2020;41(6):531–9. https://doi.org/10.1080/01612840.2019.1688436.
Ainsworth BE, Haskell WL, Herrmann SD, et al. 2011 Compendium of Physical Activities: a second update of codes and MET values. Med Sci Sports Exerc. 2011;43(8):1575–81. https://doi.org/10.1249/MSS.0b013e31821ece12.
Lynn MR. Determination and quantification of content validity. Nurs Res. 1986;35(6):382–5.
Schumacker RE, Lomax RG. A Beginner’s Guide to Structural Equation Modeling. 4th ed. Routledge; 2016.
Hu L, Bentler PM. Fit indices in covariance structure modeling: sensitivity to underparameterized model misspecification. Psychol Methods. 1998;3(4):424–53. https://doi.org/10.1037/1082-989X.3.4.424.
Stubbs B, Vancampfort D, Rosenbaum S, et al. An examination of the anxiolytic effects of exercise for people with anxiety and stress-related disorders: a meta-analysis. Psychiatry Res. 2017;249:102–8. https://doi.org/10.1016/j.psychres.2016.12.020.
Aylett E, Small N, Bower P. Exercise in the treatment of clinical anxiety in general practice – a systematic review and meta-analysis. BMC Health Serv Res. 2018;18(1):559. https://doi.org/10.1186/s12913-018-3313-5.
Golightly YM, Allen KD, Ambrose KR, et al. Physical activity as a vital sign: a systematic review. Prev Chronic Dis. 2017;14: 170030. https://doi.org/10.5888/pcd14.170030.
Coleman KJ, Ngor E, Reynolds K, et al. Initial validation of an exercise “vital sign” in electronic medical records. Med Sci Sports Exerc. 2012;44(11):2071–6. https://doi.org/10.1249/MSS.0b013e3182630ec1.
Stanton R, Happell B, Reaburn P. Investigating the exercise-prescription practices of nurses working in inpatient mental health settings. Int J Ment Health Nurs. 2015;24(2):112–20. https://doi.org/10.1111/inm.12125.
Leyland SD, Currie A, Anderson SD, Bradley E, Ling J. Offering physical activity advice to people with serious mental illness: the beliefs of mental health professionals. Ment Health Phys Act. 2018;15:1–6. https://doi.org/10.1016/j.mhpa.2018.05.002.
Hill CE, O’Brien KM. Helping skills: facilitating exploration, insight, and action. 1st ed. Washington DC: APA Books; 1999.
Lobelo F, Duperly J, Frank E. Physical activity habits of doctors and medical students influence their counselling practices. Br J Sports Med. 2008;43(2):89–92. https://doi.org/10.1136/bjsm.2008.055426.
Levinson CA, Rodebaugh TL, Menatti AR, Weeks JW. Development and validation of the social exercise and anxiety measure (SEAM): assessing fears, avoidance, and importance of social exercise. J Psychopathol Behav Assess. 2013;35(2):244–53. https://doi.org/10.1007/s10862-012-9326-1.
Glanz K, Rimer BK, Viswanath K, editors. Health behavior: theory, research, and practice. 5th ed. Jossey-Bass & Pfeiffer Imprints: Wiley; 2015.
Leutwyler H, Hubbard EM, Jeste DV, Vinogradov S. “We’re not just sitting on the periphery”: a staff perspective of physical activity in older adults with schizophrenia. Gerontologist. 2013;53(3):474–83. https://doi.org/10.1093/geront/gns092.
Stubbs B, Soundy A, Probst M, et al. The assessment, benefits and delivery of physical activity in people with schizophrenia: a survey of members of the international organization of physical therapists in mental health: physiotherapy in schizophrenia. Physiother Res Int. 2014;19(4):248–56. https://doi.org/10.1002/pri.1592.
Kline RB. Principles and practice of structural equation modeling. 4th ed. New York, NY: The Guilford Press; 2016.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Newsome, A.M., Kilpatrick, M. & Dedrick, R.F. Exercise Prescription Practices Among Mental Health Professionals on College Campuses: Testing the Information–Motivation–Behavioral Skills Model. Int.J. Behav. Med. (2024). https://doi.org/10.1007/s12529-024-10266-6
Accepted:
Published:
DOI: https://doi.org/10.1007/s12529-024-10266-6