Abstract
Isolated coronary arteritis (ICA) is an extremely rare and life-threatening vasculitis with only a limited number of reports in the literature. We retrospectively reviewed the clinical data of 10 ICA patients in our center from 2012 to 2022 and compared them with patients with Takayasu arteritis who presented with coronary arteritis initially (TAK-CA patients). We found that ICA predominantly affected women and most commonly involved the ostium and the proximal segment of the coronary arteries, causing mainly stenotic lesions. The C-reactive protein and erythrocyte sedimentation rate were grossly normal and significantly lower than those of TAK-CA patients (p = 0.027, p = 0.009, respectively). Intravascular ultrasound imaging showed superiority in differentiating coronary vasculitis from atherosclerosis. Restenosis of the coronary arteries occurred rapidly if not treated promptly and appropriately. Systemic glucocorticoid combined with immunosuppressive agents, especially cyclophosphamide, was a promising strategy for treating ICA.
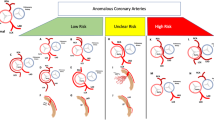
Graphical Abstract




Similar content being viewed by others
Data Availability
The data are available from the corresponding author on reasonable request.
Abbreviations
- ICA:
-
Isolated coronary arteritis
- CA:
-
Coronary arteritis
- TAK:
-
Takayasu arteritis
- PET/CT:
-
Positron emission tomography/computed tomography
- CAG:
-
Invasive coronary angiography
- CTA:
-
Computed tomography angiography
- CAD:
-
Coronary atherosclerotic heart disease
- WBC:
-
White blood cell
- ESR:
-
Erythrocyte sedimentation rate
- CRP:
-
C-reactive protein
- LM:
-
Left main
- LAD:
-
Left anterior descending
- LCX:
-
Left coronary circumflex artery
- CABG:
-
Coronary artery bypass graft
- IVUS:
-
Intravascular ultrasound
- VH:
-
Virtual histology
- CYC:
-
Cyclophosphamide
References
Norita K, de Noronha SV, Sheppard MN. Sudden cardiac death caused by coronary vasculitis. Virchows Arch. 2012;460(3):309–18. https://doi.org/10.1007/s00428-011-1173-z.
Vaideeswar P, Verma R, Gupta R. Infective coronary arteritis: a pathological analysis at autopsy. Hum Pathol. 2012;43(12):2334–41. https://doi.org/10.1016/j.humpath.2012.04.005.
Gori T Coronary vasculitis. Biomedicines (2021);9(6) https://doi.org/10.3390/biomedicines9060622.
Balink H, Bennink RJ, van Eck-Smit BL, et al. The role of 18F-FDG PET/CT in large-vessel vasculitis: appropriateness of current classification criteria? Biomed Res Int. 2014;2014:687608. https://doi.org/10.1155/2014/687608.
Chrapko BE, Chrapko M, Nocuń A, et al. Role of 18F-FDG PET/CT in the diagnosis of inflammatory and infectious vascular disease. Nucl Med Rev Cent East Eur. 2016;19(1):28–36. https://doi.org/10.5603/nmr.2016.0006.
Baymakova M, Demirev A, Kostadinova I, et al. Giant-cell arteritis without cranial manifestations presenting as fever of unknown origin: a diagnostic value of 18F-FDG PET/CT. Clin Ter. 2018;169(6):e274–6. https://doi.org/10.7417/ct.2018.2092.
Cassling RS, Lortz JB, Olson DR, et al. Fatal vasculitis (periarteritis nodosa) of the coronary arteries: angiographic ambiguities and absence of aneurysms at autopsy. J Am Coll Cardiol. 1985;6(3):707–14. https://doi.org/10.1016/s0735-1097(85)80135-2.
Swalwell CI, Reddy SK, Rao VJ. Sudden death due to unsuspected coronary vasculitis. Am J Forensic Med Pathol. 1991;12(4):306–12. https://doi.org/10.1097/00000433-199112000-00007.
Karger B, Fechner G. Sudden death due to giant cell coronary arteritis. Int J Legal Med. 2006;120(6):377–9. https://doi.org/10.1007/s00414-006-0090-1.
Dermengiu D, Hostiuc S, Cristian Curca G, et al. Sudden death due to isolated segmentary coronary vasculitis. Am J Forensic Med Pathol. 2014;35(4):223–31. https://doi.org/10.1097/PAF.0000000000000125.
Schweizer L, Fischer N, Fehr T, et al. Necrotising coronaritis with fatal outcome. BMJ Case Rep. 2017. https://doi.org/10.1136/bcr-2017-219489.
Sakai K, Asakura K, Saito K, et al. Sudden unexpected death due to coronary thrombosis associated with isolated necrotizing vasculitis in the coronary arteries of a young adult. Forensic Sci Med Pathol. 2019;15(2):252–7. https://doi.org/10.1007/s12024-019-00099-1.
Shimizu T, Sato A, Sakamoto K, et al. Intravascular ultrasound imaging of isolated and non aorto-ostial coronary Takayasu arteritis: a case report. BMC Cardiovasc Disord. 2020;20(1):260. https://doi.org/10.1186/s12872-020-01541-x.
Araszkiewicz A, Prech M, Hrycaj P, et al. Acute myocardial infarction and rapid development of coronary aneurysms in a young woman–unusual presentation of Takayasu arteritis? Can J Cardiol. 2007;23(1):61–3. https://doi.org/10.1016/s0828-282x(07)70215-5.
Hernandez-Rodriguez J, Hoffman GS. Updating single-organ vasculitis. Curr Opin Rheumatol. 2012;24(1):38–45. https://doi.org/10.1097/BOR.0b013e32834d8482.
Arend WP, Michel BA, Bloch DA, et al. The American College of Rheumatology 1990 criteria for the classification of Takayasu arteritis. Arthritis Rheum. 1990;33(8):1129–34. https://doi.org/10.1002/art.1780330811.
Broncano J, Vargas D, Bhalla S, et al. CT and MR imaging of cardiothoracic vasculitis. Radiographics. 2018;38(4):997–1021. https://doi.org/10.1148/rg.2018170136.
Friedman KG, Gauvreau K, Hamaoka-Okamoto A, et al. Coronary artery aneurysms in Kawasaki Disease: risk factors for progressive disease and adverse cardiac events in the US Population. J Am Heart Assoc. 2016;5(9) https://doi.org/10.1161/jaha.116.003289.
Pagnoux C, Guillevin L. Cardiac involvement in small and medium-sized vessel vasculitides. Lupus. 2005;14(9):718–22. https://doi.org/10.1191/0961203305lu2207oa.
Jang JJ, Gorevic PD, and Olin JW. Images in vascular medicine. Giant cell arteritis presenting with acute myocardial infarction. Vasc Med. 2007;12(4):379. https://doi.org/10.1177/1358863x07083176.
Matsubara O, Kuwata T, Nemoto T, et al. Coronary artery lesions in Takayasu arteritis: pathological considerations. Heart Vessels Suppl. 1992;7:26–31. https://doi.org/10.1007/bf01744540.
Banerjee S, Bagheri M, Sandfort V, et al. Vascular calcification in patients with large-vessel vasculitis compared to patients with hyperlipidemia. Semin Arthritis Rheum. 2019;48(6):1068–73. https://doi.org/10.1016/j.semarthrit.2018.09.001.
Huang HL, Fong W, Peh WM, et al. The utility of FDG PET/CT in IgG4-related disease with a focus on coronary artery involvement. Nucl Med Mol Imaging. 2018;52(1):53–61. https://doi.org/10.1007/s13139-017-0494-5.
James OG, Christensen JD, Wong TZ, et al. Utility of FDG PET/CT in inflammatory cardiovascular disease. Radiographics. 2011;31(5):1271–86. https://doi.org/10.1148/rg.315105222.
Nasu K, Tsuchikane E, Katoh O, et al. Accuracy of in vivo coronary plaque morphology assessment: a validation study of in vivo virtual histology compared with in vitro histopathology. J Am Coll Cardiol. 2006;47(12):2405–12. https://doi.org/10.1016/j.jacc.2006.02.044.
Rav-Acha M, Plot L, Peled N, et al. Coronary involvement in Takayasu’s arteritis. Autoimmun Rev. 2007;6(8):566–71. https://doi.org/10.1016/j.autrev.2007.04.001.
Noma M, Sugihara M, Kikuchi Y. Isolated coronary ostial stenosis in Takayasu’s arteritis: case report and review of the literature. Angiology. 1993;44(10):839–44. https://doi.org/10.1177/000331979304401013.
Seguchi M, Hino Y, Aiba S, et al. Ostial stenosis of the left coronary artery as a sole clinical manifestation of Takayasu’s arteritis: a possible cause of unexpected sudden death. Heart Vessels. 1990;5(3):188–91. https://doi.org/10.1007/bf02059914.
Emi Y, Yamakado T, Futagami Y, et al. Isolated bilateral coronary ostial stenosis in Takayasu’s arteritis. Am Heart J. 1990;119(4):962–4. https://doi.org/10.1016/s0002-8703(05)80341-2.
Kihara M, Kimura K, Yakuwa H, et al. Isolated left coronary ostial stenosis as the sole arterial involvement in Takayasu’s disease. J Intern Med. 1992;232(4):353–5. https://doi.org/10.1111/j.1365-2796.1992.tb00597.x.
Acknowledgements
The authors thank the patients for participating in this study.
Funding
This study was supported by the Chinese Academy of Medical Sciences (CAMS) Innovation Fund for Medical Sciences (CIFMS) (2021-I2M-1–005).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Human Subjects Statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Competing Interests
The authors declare no competing interests.
Additional information
Associate Editor Angela Taylor oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, L., Li, J., Gan, T. et al. Isolated Coronary Arteritis in Adults: a Single-Center Experience from China. J. of Cardiovasc. Trans. Res. 16, 1184–1193 (2023). https://doi.org/10.1007/s12265-023-10388-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-023-10388-4