Abstract
Introduction
Arterial hypertension (AH) is prevalent in acromegaly, but few studies using 24-h ambulatory blood pressure monitoring (24 h-ABPM) suggest that its frequency may be different from office blood pressure (OBP). Left ventricular hypertrophy (LVH) is one of the most frequent cardiac abnormalities. Cardiac magnetic resonance (CMR) is considered the gold standard to evaluate the heart.
Objectives
To compare the frequency of AH when measured by 24 h-ABPM and by OBP and to correlate BP with cardiac mass.
Methods
Patients over 18 years of age with acromegaly underwent OBP evaluation and were later referred to the 24 h-ABPM. Treatment-naïve patients were submitted to CMR.
Results
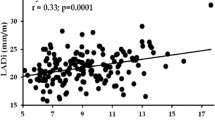
We evaluated 96 patients. From 29 non hypertensive patients by OBP, 9 had AH on 24 h-ABPM. In the group of patients with a previous diagnosis of AH by OBP, 25 had controlled BP and 42 had abnormal BP on 24 h-ABPM, when analyzed by OBP there were 28 with controlled BP. We observed a positive correlation between diastolic BP measured in 24 h-ABPM and IGF-I levels, but we did not observe the same correlation with age, sex, body mass index and GH levels. The CMR was performed in 11 patients. We found a positive correlation of left ventricular mass (LVM) and BP of 24 h-ABPM. In contrast, there was no correlation of OBP with CMR parameters.
Conclusions
We observed, that 24 h-ABPM in acromegaly allows the diagnosis of AH in some patients with normal BP in OBP and also to allow a better treatment. 24 h-ABPM shows a better correlation with VM by CMR.

Similar content being viewed by others
Data availability
The authors confirm that he understand journal Pituitary is a transformative journal. When research is accepted for publication, there is a choice to publish using either immediate gold open access or the traditional publishing route. The results/data/figures in this manuscript have not been published elsewhere, nor are they under consideration (from you or one of your Contributing Authors) by another publisher. All of the material is owned by the authors and/or no permissions are required.
References
Gadelha MR, Kasuki L, Lim DST, Fleseriu M (2019) Systemic complications of acromegaly and the impact of the current treatment landscape: an update. Endocr Rev 40(1):268–332
Colao A, Ferone D, Marzullo P, Lombardi G (2004) Systemic complications of acromegaly: epidemiology, pathogenesis, and management. Endocr Rev 25(1):102–152
Costenaro F, Martin A, Horn RF, Czepielewski MA, Rodrigues TC (2016) Role of ambulatory blood pressure monitoring in patients with acromegaly. J Hypertens 34(7):1357–1363
Minniti G, Moroni C, Jaffrain-Rea ML, Bondanini F, Gulino A, Cassone R et al (1998) Prevalence of hypertension in acromegalic patients: clinical measurement versus 24-hour ambulatory blood pressure monitoring. Clin Endocrinol 48(2):149–152
Colao A, Baldelli R, Marzullo P, Ferretti E, Ferone D, Gargiulo P et al (2000) Systemic hypertension and impaired glucose tolerance are independently correlated to the severity of the acromegalic cardiomyopathy. J Clin Endocrinol Metab 85(1):193–199
Mann DLZD, Libby P, Bonow RO, Braunwald E (2015) Braunwald’s heart disease: a textbook of cardiovascular medicine, 9th edn. Elsevier, Berlin
Sara LSGTA, Shiozaki AA, Villa AV, Oliveira AC, Albuquerque AS et al (2014) II diretriz da Ressonância Magnética e Tomografia Computadorizada Cardiovascular da Sociedade Brasileira de Cardiologia e do Colégio Brasilerio de Radiologia. Arq Iras Cardiol 103:6
Sara L, Szarf G, Tachibana A, Shiozaki AA, Villa AV, de Oliveira AC et al (2014) II guidelines on cardiovascular magnetic resonance and computed tomography of the Brazilian Society of Cardiology and the Brazilian College of Radiology. Arq Bras Cardiol 103(6 Suppl 3):1–86
Lopez-Velasco R, Escobar-Morreale HF, Vega B, Villa E, Sancho JM, Moya-Mur JL et al (1997) Cardiac involvement in acromegaly: specific myocardiopathy or consequence of systemic hypertension? J Clin Endocrinol Metab 82(4):1047–1053
Katznelson L, Laws ER Jr, Melmed S, Molitch ME, Murad MH, Utz A et al (2014) Acromegaly: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 99(11):3933–3951
World Health Organization (2000) Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organization technical report series, vol 894. World Health Organization, Geneva, pp 1–253
American Diabetes Association (2021) 2. Classification and diagnosis of diabetes: standards of medical care in diabetes-2021. Diabetes Care 44(Suppl 1):S15–S33
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C et al (2018) 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension 71(6):1269–1324
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M et al (2018) 2018 ESC/ESH Guidelines for the management of arterial hypertension: The Task Force for the management of arterial hypertension of the European Society of Cardiology and the European Society of Hypertension: The Task Force for the management of arterial hypertension of the European Society of Cardiology and the European Society of Hypertension. J Hypertens 36(10):1953–2041
Schneider RH, Salerno J, Brook RD (2020) 2020 International Society of Hypertension global hypertension practice guidelines—lifestyle modification. J Hypertens 38(11):2340–2341
Jones CR, Taylor K, Chowienczyk P, Poston L, Shennan AH (2000) A validation of the Mobil O Graph (version 12) ambulatory blood pressure monitor. Blood Press Monit 5(4):233–238
Parati G, Stergiou G, O’Brien E, Asmar R, Beilin L, Bilo G et al (2014) European Society of Hypertension practice guidelines for ambulatory blood pressure monitoring. J Hypertens 32(7):1359–1366
Petersen SE, Khanji MY, Plein S, Lancellotti P, Bucciarelli-Ducci C (2019) European Association of Cardiovascular Imaging expert consensus paper: a comprehensive review of cardiovascular magnetic resonance normal values of cardiac chamber size and aortic root in adults and recommendations for grading severity. Eur Heart J Cardiovasc Imaging 20(12):1321–1331
Marcu CB, Nijveldt R, Beek AM, Van Rossum AC (2007) Delayed contrast enhancement magnetic resonance imaging for the assessment of cardiac disease. Heart Lung Circ 16(2):70–78
Kasuki L, Rocha PDS, Lamback EB, Gadelha MR (2019) Determinants of morbidities and mortality in acromegaly. Arch Endocrinol Metab 63(6):630–637
Terzolo M, Matrella C, Boccuzzi A, Luceri S, Borriero M, Reimondo G et al (1992) Twenty-four hour profile of blood pressure in patients with acromegaly. Correlation with demographic, clinical and hormonal features. J Endocrinol Investig 22(1):48–54
Altikardes ZA, Kayikli A, Korkmaz H, Erdal H, Baba AF, Fak AS (2019) A novel method for dipper/non-dipper pattern classification in hypertensive and non-diabetic patients. Technol Health Care 27(S1):47–57
Hernandez-Gordillo D, Ortega-Gomez Mdel R, Galicia-Polo L, Castorena-Maldonado A, Vergara-Lopez A, Guillen-Gonzalez MA et al (2012) Sleep apnea in patients with acromegaly. Frequency, characterization and positive pressure titration. Open Respir Med J 6:28–33
van Haute FR, Taboada GF, Correa LL, Lima GA, Fontes R, Riello AP et al (2008) Prevalence of sleep apnea and metabolic abnormalities in patients with acromegaly and analysis of cephalometric parameters by magnetic resonance imaging. Eur J Endocrinol 158(4):459–465
Sanchez-Ortiga R, Climent V, Sanchez-Tejada L, Candela A, Pico A (2015) Severe sleep apnea-hypopnea syndrome is related to left ventricle dysfunction and hypertrophy in acromegalic patients. Endocrinol Nutr 62(8):366–372
Collop NA (2005) Obstructive sleep apnea: what does the cardiovascular physician need to know? Am J Cardiovasc Drugs 5(2):71–81
Jordan AS, McSharry DG, Malhotra A (2014) Adult obstructive sleep apnoea. Lancet 383(9918):736–747
Chiu HY, Chen PY, Chuang LP, Chen NH, Tu YK, Hsieh YJ et al (2017) Diagnostic accuracy of the Berlin questionnaire, STOP-BANG, STOP, and Epworth sleepiness scale in detecting obstructive sleep apnea: a bivariate meta-analysis. Sleep Med Rev 36:57–70
Sawatari H, Chishaki A, Ando SI (2016) The epidemiology of sleep disordered breathing and hypertension in various populations. Curr Hypertens Rev 12(1):12–17
Kario K (2009) Obstructive sleep apnea syndrome and hypertension: mechanism of the linkage and 24-h blood pressure control. Hypertens Res 32(7):537–541
Marrone O, Bonsignore MR (2018) Blood-pressure variability in patients with obstructive sleep apnea: current perspectives. Nat Sci Sleep 10:229–242
Jones NR, McCormack T, Constanti M, McManus RJ (2020) Diagnosis and management of hypertension in adults: NICE guideline update 2019. Br J Gen Pract 70(691):90–91
Cohen JB (2020) Masked hypertension: fragile in more ways than one. Hypertension 76(4):1079–1080
Brguljan-Hitij J, Thijs L, Li Y, Hansen TW, Boggia J, Liu YP et al (2014) Risk stratification by ambulatory blood pressure monitoring across JNC classes of conventional blood pressure. Am J Hypertens 27(7):956–965
Ohtsuka H, Komiya I, Aizawa T, Yamada T (1995) Hypertension in acromegaly: hereditary hypertensive factor produces hypertension by enhancing IGF-I production. Endocr J 42(6):781–787
Vitale G, Pivonello R, Auriemma RS, Guerra E, Milone F, Savastano S et al (2005) Hypertension in acromegaly and in the normal population: prevalence and determinants. Clin Endocrinol 63(4):470–476
Arosio M, Reimondo G, Malchiodi E, Berchialla P, Borraccino A, De Marinis L et al (2012) Predictors of morbidity and mortality in acromegaly: an Italian survey. Eur J Endocrinol 167(2):189–198
Schutte AE, Volpe M, Tocci G, Conti E (2014) Revisiting the relationship between blood pressure and insulin-like growth factor-1. Hypertension 63(5):1070–1077
Treibel TA, Zemrak F, Sado DM, Banypersad SM, White SK, Maestrini V et al (2015) Extracellular volume quantification in isolated hypertension—changes at the detectable limits? J Cardiovasc Magn Reson 17:74
Bogazzi F, Lombardi M, Strata E, Aquaro G, Di Bello V, Cosci C et al (2008) High prevalence of cardiac hypertophy without detectable signs of fibrosis in patients with untreated active acromegaly: an in vivo study using magnetic resonance imaging. Clin Endocrinol 68(3):361–368
Warszawski L, Kasuki L, Sa R, Dos Santos Silva CM, Volschan I, Gottlieb I et al (2016) Low frequency of cardniac arrhythmias and lack of structural heart disease in medically-naive acromegaly patients: a prospective study at baseline and after 1 year of somatostatin analogs treatment. Pituitary 19(6):582–589
Funding
This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector.
Author information
Authors and Affiliations
Contributions
PR collected the data and wrote the initial draft, FC and JB performed the cardio logic evaluations supervised by EM, MG and LK supervised the study and critically reviewed the data. All others approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
M.R.G. has served as an advisory board member for Ipsen, Novartis Pharmaceuticals, Novo Nordisk, Re-cordati Rare Diseases and Crinetics Pharmaceuticals; as a research investigator for Crinetics Pharmaceuticals, Recordati Rare Diseases and Novartis Pharmaceuticals; and as a speaker for Crinetics Pharmaceuticals, Novartis Pharmaceuticals, Ipsen, Novo Nordisk and Recordati Rare Diseases. L.K. has received speaker fees from Novartis and Ipsen.
Ethical approval
This study was conducted in accordance with the Declaration of Helsinki and was approved by the Ethics Committee of HUCFF/UFRJ (3. 858. 071) and Faculdade de Medicina da UFRJ and all patients signed written informed consent forms.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rocha, P., Barroso, J., Carlos, F. et al. Importance of 24 h ambulatory blood pressure monitoring in patients with acromegaly and correlation with cardiac magnetic resonance findings. Pituitary 26, 402–410 (2023). https://doi.org/10.1007/s11102-023-01321-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-023-01321-8