Abstract
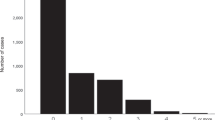
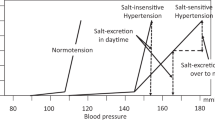
Nocturia has been increasingly recognized as a manifestation of various non-urological conditions including hypertension. In adults, blood pressure (BP) elevation has been identified as a robust correlate of nocturia, but such a relationship has not been studied in pediatric populations where nocturia is often attributed to hormonal, sleep, physiological or psychological disorders. Accordingly, this study aimed to determine the relationship between nocturia and BP elevation in adolescents. We prospectively studied 100 patients, aged 10–18 years, recruited from pediatric clinics at our institution. Nocturia (defined as ≥ 1 voids on voiding diary analysis) was present in 45% of the study sample (range: 1–4 voids/night). 37% of subjects self-reported awakening to urinate, and 34% of subjects had BP elevation according to age-dependent thresholds from current Pediatrics guidelines. On multivariate analyses, BP elevation was strongly associated with nocturia determined by both voiding diary (OR 26.2, 95% CI: 6.5, 106.0) and self-report. Conversely, nocturia was associated with increased odds of elevated BP by diary (26.3, 95% CI: 6.5, 106.4) and self-report (OR 8.1, 95% CI: 3.2, 20.5). In conclusion, nocturia appears to be common and is strongly associated with BP elevation in adolescents. These findings suggest that eliciting a history of nocturia holds promise as a simple method of identifying adolescents at risk for hypertension.

Similar content being viewed by others
References
Hashim, H., Blanker, M. H., Drake, M. J., et al. (2019). International Continence Society (ICS) report on the terminology for nocturia and nocturnal lower urinary tract function. Neurol Urodyn, 38(2), 499–508. https://doi.org/10.1002/nau.23917.
Weiss, J. P., Monaghan, T. F., Epstein, M. R., & Lazar, J. M. (2019). Future considerations in Nocturia and Nocturnal Polyuria. Urology, 133S, 34–42. https://doi.org/10.1016/j.urology.2019.06.014Epub 2019 Jun 22. PMID: 31233816.
Rahman, S. N., Cao, D. J., Monaghan, T. F. (2020). Phenotyping the Association between Nocturia and Hypertension: A systematic review and Meta-analysis. Journal of Urology, 101097JU0000000000001433.
Victor, R. G., Li, N., Blyler, C. A., et al. (2019). Nocturia as an unrecognized symptom of uncontrolled Hypertension in Black men aged 35 to 49 years. J Am Heart Assoc, 8(5), e010794. https://doi.org/10.1161/JAHA.118.010794PMID: 30827133; PMCID: PMC6474941.
Lazar, J. M., Posner, A., Akbar, K. (2022). Home Blood Pressure Monitoring And Nocturia In Adults. J Community Health, https://doi.org/10.1007/s10900-022-01171-8. Epub ahead of print. PMID: 36370256.
Matsushima, E., Otsuka, Y., Itani, O., Matsumoto, Y., & Kaneita, Y. (2022). Association between nighttime urinary frequency and sleep problems among Japanese adolescents. International Journal of Urology, 29(2), 152–157. https://doi.org/10.1111/iju.14744Epub 2021 Nov 17. PMID: 34786770.
Yazici, C. M., Abali, R., Tasdemir, N., Dogan, C., & Yildiz, T. (2014). Is nocturia of young adulthood a remnant of childhood nocturnal enuresis? International Urogynecology Journal, 25(2), 273–278. https://doi.org/10.1007/s00192-013-2203-y. quiz 277-8.
Mattsson, S. (1994). Urinary incontinence and nocturia in healthy schoolchildren. Acta Paediatr, 83(9): 950–954. https://doi.org/10.1111/j.1651-2227.1994.tb13179.x. PMID: 7819693.
Warner, T. C., Baandrup, U., Jacobsen, R., Bøggild, H., Østergaard, A., & Hagstrøm, P. S. (2019). S. Prevalence of nocturia and fecal and urinary incontinence and the association to childhood obesity: a study of 6803 Danish school children. J Pediatr Urol, 15(3): 225.e1-225.e8. doi: 10.1016/j.jpurol.2019.02.004. Epub 2019 Feb 15. PMID: 30930018.
Yüce, Ö., Bayrakçi, U. S., Gülleroğlu, K., & Baskın, E. (2016). Abnormal circadian blood pressure regulation in children with nocturnal enuresis. Renal Failure, 38(6), 899–905. Epub 2016 Apr 7. PMID: 27056252.
Kruse, A., Mahler, B., Rittig, S., & Djurhuus, J. C. (2009). Increased nocturnal blood pressure in enuretic children with polyuria. Journal of Urology, 182(4 Suppl), 1954–1960. https://doi.org/10.1016/j.juro.2009.04.079Epub 2009 Aug 20. PMID: 19695582.
Flynn, J. T., Kaelber, D. C., Baker-Smith, C. M. (2017). Subcommittee on Screening and Management of High Blood Pressure in Children. Clinical Practice Guideline for Screening and Management of High Blood Pressure in Children and Adolescents. Pediatrics, 140(3): e20171904. Pediatrics. 2018;142(3):e20181739. https://doi.org/10.1542/peds.2018-1739. Erratum for: Pediatrics. 2017;140(3): PMID: 30177515.
Jackson, S. L., Zhang, Z., Wiltz, J. L., et al. (2018). Hypertension among youths - United States, 2001–2016. Mmwr. Morbidity and Mortality Weekly Report, 67, 758–762. https://doi.org/10.15585/mmwr.mm6727a2externalicon.
Hardy, S. T., Sakhuja, S., Jaeger, B. C., et al. (2021). Trends in blood pressure and Hypertension among US children and adolescents, 1999–2018. JAMA Netw Open, 4(4), e213917. https://doi.org/10.1001/jamanetworkopen.2021.3917.
Wong, S. N., Sung, T., & Leung, R. Y. (2006). L. C. Validation of three oscillometric blood pressure devices against auscultatory mercury sphygmomanometer in children. Blood Press Monit, 11(5): 281–291. https://doi.org/10.1097/01.mbp.0000209082.09623.b4. PMID: 16932037.
Monaghan, T. F., Rahman, S. N., Bliwise, D. L., et al. (2020). Identifying men with global polyuria on a nocturnal-only voiding diary. Neurourology and Urodynamics, 39(1), 347–352.
International Consultation on Incontinence Questionnaire Nocturia Module (ICIQ-N). https://iciq.net/iciq-n#.
Bell, C. S., Samuel, J. P., & Samuels, J. A. (2019). Prevalence of Hypertension in children. Hypertension, 73(1), 148–152. https://doi.org/10.1161/HYPERTENSIONAHA.118.11673PMID: 30571555; PMCID: PMC6291260.
BMI and BMI Categories for Children and Teens. https://www.cdc.gov/obesity/basics/childhood-defining.html.
Lin, L. I. (1989). A concordance correlation coefficient to evaluate reproducibility. Biometrics, 45(#1), 255–268. https://doi.org/10.2307/2532051.
Carroll, A. J., Tedla, Y. G., Padilla, R., et al. (2023). Adherence to the 2017 clinical practice guidelines for pediatric Hypertension in safety-net clinics. JAMA Netw Open, 6(4), e237043. https://doi.org/10.1001/jamanetworkopen.2023.7043.
Romero, J. C., & Knox, F. G. (1988). Mechanisms underlying pressure-related natriuresis: the role of the renin-angiotensin and prostaglandin systems. State of the art lecture. Hypertension, 11(6 Pt 2): 724–738. doi: 10.1161/01.hyp.11.6.724. PMID: 3292417.
Mekki, P., Monaghan, T. F., Lee, L., et al. (2021). Nocturia and electrocardiographic abnormalities among patients at an inner-city cardiology clinic. Neurourology and Urodynamics, 40(1), 509–514. https://doi.org/10.1002/nau.24590Epub 2020 Dec 21. PMID: 33348456.
Kao, K. W., Cheng, W., Wu, C. J., & Fan, Y. H. (2022). Nocturia independently predicts left ventricular hypertrophy and left atrial enlargement among patients with cardiac symptoms. Scientific Reports, 12(1), 14897. https://doi.org/10.1038/s41598-022-19190-9PMID: 36050443; PMCID: PMC9436922.
Torimoto, K., Hirayama, A., Samma, S., Yoshida, K., Fujimoto, K., & Hirao, Y. (2009). The relationship between nocturnal polyuria and the distribution of body fluid: Assessment by bioelectric impedance analysis. Journal of Urology, 181(1), 219–224. https://doi.org/10.1016/j.juro.2008.09.031(discussion 224).
Kansagra, S. (2020). Sleep disorders in adolescents. Pediatrics, 145(Supplement_2), S204–S209. https://doi.org/10.1542/peds.2019-2056I.
Bosch, J. L. H. R., & Weiss, J. P. (2013). The prevalence and causes of Nocturia. The Journal of Urology, 189, S86–92. https://doi.org/10.1016/j.juro.2012.11.033.
Robinson, D., Toozs-Hobson, P., & Cardozo, L. (2013). The effect of hormones on the lower urinary tract. Menopause Int, 19(4): 155–162. https://doi.org/10.1177/1754045313511398. PMID: 24336244.
Al-Mehaisen, L. M. M., Hani, B., & Al-Kuran, O. M. K., O. A. H (2018). Is age of menarche related to urinary symptoms in young Jordanian girls? A prospective cross-sectional study. J Taibah Univ Med Sci, 13(4), 332–337. PMID: 31435344; PMCID: PMC6694926.
Mock, L. L., Parmelee, P. A., Kutner, N., et al. (2008). Content validation of symptom-specific nocturia quality-of-life instrument developed in men: Issues expressed by women, as well as men. Urology, 72(4), 736–742.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Nothing to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Promi, T., Tologonova, G., Roberts, MC. et al. Nocturia and Blood Pressure Elevation in Adolescents. J Community Health 49, 379–384 (2024). https://doi.org/10.1007/s10900-023-01307-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-023-01307-4