Abstract
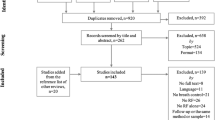
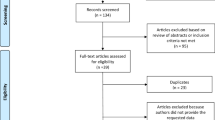
Meta-analysis was used to investigate the potential benefits of stress management interventions (SMIs) on vagally-mediated heart rate variability (HRV) in adults with cardiovascular disease. Electronic bibliographic databases were searched through August 2022. Randomized controlled trials and quasi-experimental studies assessing effects of SMIs on HRV were included. Methodological quality was assessed with a standardized checklist. A pooled effect size was calculated for vagally-mediated HRV indices (standard deviation of normal-to-normal intervals, root mean square of the successive differences, and high frequency power) using random effects models. Fourteen studies (1202 participants, Mage: 59 ± 6.25 years; 25% ± 16% women; 61% ± 22% White) were included. Ten studies (11 effects) reported short-term HRV assessment; a small between-group difference emerged for vagally-mediated HRV (d+ = .27, 95% confidence interval [CI] 0.01–0.52, k = 11). Most interventions examined biofeedback; these studies yielded a small between-group difference on vagally-mediated HRV (d+ = 0.31, 95% CI 0.09–0.53, k = 7, Q [6] = 3.82, p = .70, I2 = 11%). This is the first systematic examination of the effect of SMIs on HRV in adults with CVD. Findings suggest a small effect of SMIs on vagally-mediated HRV, with biofeedback likely driving the effect. More research is required to fully understand whether this benefit on vagally-mediated HRV applies to other SMIs.

Similar content being viewed by others
Data availability
De-identified data from this study are not available in a public archive. In light of the meta-analytic nature of this project, data used to calculate effect sizes can be obtained from the original sources cited in this text. Analytic code used to conduct the analyses presented in this study are not available in a public archive. They may be available by emailing the corresponding author. Materials used to conduct the study are not publicly available.
References
Becker, B. J. (1988). Synthesizing standardized mean-change measures. British Journal of Mathematical and Statistical Psychology, 41, 257–278. https://doi.org/10.1111/j.2044-8317.1988.tb00901.x
Begg, C. B., & Mazumdar, M. (1994). Operating characteristics of a rank correlation test for publication bias. Biometrics. https://doi.org/10.3109/17453674.2016.1153359
Beresnevaitė, M., Benetis, R., Taylor, G. J., Rašinskienė, S., Stankus, A., & Kinduris, S. (2016). Impact of a cognitive behavioral intervention on health-related quality of life and general heart rate variability in patients following cardiac surgery: An effectiveness study. Psychosomatics: Journal of Consultation and Liaison Psychiatry, 57, 605–615. https://doi.org/10.1016/j.psym.2016.04.004
Blumenthal, J. A., Sherwood, A., Babyak, M. A., Watkins, L. L., Waugh, R., Georgiades, A., Bacon, S. L., Hayano, J., Coleman, R. E., & Hinderliter, A. (2005). Effects of exercise and stress management training on markers of cardiovascular risk in patients with ischemic heart disease: A randomized controlled trial. JAMA: Journal of the American Medical Association, 293, 1626–1634.
Blumenthal, J. A., Sherwood, A., Smith, P. J., Watkins, L., Mabe, S., Kraus, W. E., Ingle, K., Miller, P., & Hinderliter, A. (2016). Enhancing cardiac rehabilitation with stress management training: A randomized, clinical efficacy trial. Circulation, 133(14), 1341–1350.
Brown, L., Rando, A. A., Eichel, K., Van Dam, N. T., Celano, C. M., Huffman, J. C., & Morris, M. E. (2021). The effects of mindfulness and meditation on vagally mediated heart rate variability: A meta-analysis. Psychosomatic Medicine, 83, 631–640.
Buccelletti, F., Gilardi, E. M., Scaini, E., Galiuto, L. E., Persiani, R. O., Biondi, A. L., Basile, F. L., & Silveri, N. G. (2009). Heart rate variability and myocardial infarction: Systematic literature review and metanalysis. European Review for Medical and Pharmacological Sciences, 13, 299–307.
Carney, R. M., & Freeland, K. E. (2009). Depression and heart rate variability in patients with coronary heart disease. Cleveland Clinic Journal of Medicine, 76, S13. https://doi.org/10.1001/archpsyc.62.6.661
Carney, R. M., Freedland, K. E., Stein, P. K., Skala, J. A., Hoffman, P., & Jaffe, A. S. (2000). Change in heart rate and heart rate variability during treatment for depression in patients with coronary heart disease. Psychosomatic Medicine, 62, 639–647.
Catai, A. M., Pastre, C. M., de Godoy, M. F., da Silva, E., de Medeiros Takahashi, A. C., & Vanderlei, L. C. M. (2020). Heart rate variability: Are you using it properly? Standardisation checklist of procedures. Brazilian Journal of Physical Therapy, 24, 91–102.
Chambers, A. S., & Allen, J. J. (2002). Vagal tone as an indicator of treatment response in major depression. Psychophysiology, 39, 861–864. https://doi.org/10.1111/1469-8986.3960861
Chandrasekaran, A., Kinra, S., Ajay, V., & Chattopadhyay, K. (2019). Effectiveness and cost-effectiveness of a Yoga-based Cardiac Rehabilitation (Yoga-CaRe) program following acute myocardial infarction: Study rationale and design of a multi-center randomized controlled trial. International Journal of Cardiology, 280, 14–18.
Chang, R., Koo, M., Yu, Z., Kan, C., Chu, I., Hsu, C., & Chen, C. (2008). The effect of t’ai chi exercise on autonomic nervous function of patients with coronary artery disease. Journal of Alternative & Complementary Medicine, 14, 1107–1113. https://doi.org/10.1089/acm.2008.0166
Cheng, Y.-C., Huang, Y.-C., & Huang, W.-L. (2019). Heart rate variability as a potential biomarker for alcohol use disorders: A systematic review and meta-analysis. Drug and Alcohol Dependence, 204, 107502.
Chevalier, P., Cottraux, J., Mollard, E., Sai, N., Brun, S., Burri, H., Restier, L., & Adeleine, P. (2006). Prevention of implantable defibrillator shocks by cognitive behavioral therapy: A pilot trial. American Heart Journal, 151, 191. https://doi.org/10.1016/j.ahj.2005.10.007
Christa, S. E., Srivastava, P., Chandran, D. S., Jaryal, A. K., Yadav, R. K., Roy, A., & Deepak, K. K. (2019). Effect of yoga-based cardiac rehabilitation on heart rate variability: Randomized controlled trial in patients post-MI. International Journal of Yoga Therapy, 29, 43–50. https://doi.org/10.17761/2019-00019
Christa, S. E., Srivastava, P., Jaryal, A. K., Roy, A., Chandran, D. S., & Deepak, K. K. (2017). Heart rate variability in MI patients: Comparison of single and multivessel disease. Indian Journal of Physiology and Pharmacology, 61, 146–147.
Cohen, B. E., Edmondson, D., & Kronish, I. M. (2015). State of the art review: Depression, stress, anxiety, and cardiovascular disease. American Journal of Hypertension, 28, 1295–1302. https://doi.org/10.1093/ajh/hpv047
Deepak, K. K., & Christa, E. (2017). Role of yoga in patients with heart attack. https://doi.org/10.1002/central/CN-01892621/full
Del Pozo, J., & Gevirtz, R. (2002). The effect of resonant frequency cardiac biofeedback training on heart rate variability in a cardiac rehabilitation population. Applied Psychophysiology and Biofeedback, 27, 311–311.
Del Pozo, J. M. (2002). Biofeedback treatment increases heart rate variability in patients with known coronary artery disease. ProQuest Dissertations & Theses Global.
Del Pozo, J. M., Gevirtz, R. N., Scher, B., & Guarneri, E. (2004). Biofeedback treatment increases heart rate variability in patients with known coronary artery disease. American Heart Journal, 147, E11. https://doi.org/10.1016/j.ahj.2003.08.013
Downs, S. H., & Black, N. (1998). The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. Journal of Epidemiology & Community Health, 52, 377–384. https://doi.org/10.1136/jech.52.6.377
Duval, S., & Tweedie, R. (2000). Trim and fill: A simple funnel-plot–based method of testing and adjusting for publication bias in meta-analysis. Biometrics, 56, 455–463. https://doi.org/10.1111/j.0006-341x.2000.00455.x
Egger, M., Smith, G. D., Schneider, M., & Minder, C. (1997). Bias in meta-analysis detected by a simple, graphical test. British Medical Journal, 315, 629–634. https://doi.org/10.1136/bmj.315.7109.629
Freedland, K. E., Steinmeyer, B. C., Carney, R. M., Skala, J. A., Chen, L., & Rich, M. W. (2021). Depression and hospital readmissions in patients with heart failure. American Journal of Cardiology, 6, 66.
Gathright, E. C., Salmoirago-Blotcher, E., DeCosta, J., Donahue, M. L., Feulner, M. M., Cruess, D. G., Wing, R. R., Carey, M. P., & Scott-Sheldon, L. A. (2021). Stress management interventions for adults living with heart failure: A systematic review and meta-analysis. Health Psychology, 40, 606–616.
Grässler, B., Thielmann, B., Böckelmann, I., & Hökelmann, A. (2021). Effects of different exercise interventions on heart rate variability and cardiovascular health factors in older adults: A systematic review. European Review of Aging and Physical Activity, 18, 1–21.
Hedges, L. V. (1981). Distribution theory for Glass’s estimator of effect size and related estimators. Journal of Educational Statistics, 6, 107–128. https://doi.org/10.2307/1164588
Higgins, J. P., & Thompson, S. G. (2002). Quantifying heterogeneity in a meta-analysis. Statistics in Medicine, 21, 1539–1558. https://doi.org/10.1002/sim.1186
Hillebrand, S., Gast, K. B., de Mutsert, R., Swenne, C. A., Jukema, J. W., Middeldorp, S., Rosendaal, F. R., & Dekkers, O. M. (2013). Heart rate variability and first cardiovascular event in populations without known cardiovascular disease: Meta-analysis and dose–response meta-regression. Europace, 15, 742–749.
Huedo-Medina, T. B., Sánchez-Meca, J., Marín-Martínez, F., & Botella, J. (2006). Assessing heterogeneity in meta-analysis: Q statistic or I2 index? Psychological Methods, 11, 193. https://doi.org/10.1037/1082-989X.11.2.193
Jadad, A. R., Moore, R. A., Carroll, D., Jenkinson, C., Reynolds, D. J. M., Gavaghan, D. J., & McQuay, H. J. (1996). Assessing the quality of reports of randomized clinical trials: Is blinding necessary? Controlled Clinical Trials, 17, 1–12. https://doi.org/10.1016/0197-2456(95)00134-4
Krishna, B. H. (2012a). Benefits of yoga therapy for heart problem patients. http://www.who.int/trialsearch/Trial2.aspx?TrialID=CTRI/2012/06/002734
Krishna, B. H. (2012b). Benefits of yoga therapy for heart problem patients. ctri.nic.in.
Krishna, B. H., Pal, P., Pal, G. K., Balachander, J., Jayasettiaseelon, E., Sreekanth, Y., Sridhar, M. G., & Gaur, G. S. (2014a). Effect of yoga therapy on heart rate, blood pressure and cardiac autonomic function in heart failure. Journal of Clinical and Diagnostic Research, 8, 14–16. https://doi.org/10.7860/JCDR/2014/7844.3983
Krishna, B. H., Pal, P., Pal, G. K., Balachander, J., Jayasettiaseelon, E., Sreekanth, Y., Sridhar, M. G., & Gaur, G. S. (2014b). Yoga improves quality of life and functional capacity in heart failure patients. Biomedical Research, 25, 178–182.
Krishna, B. H., Pal, P., Pal, G. K., Balachander, J., Jayasettiaseelon, E., Sreekanth, Y., Sridhar, M. G., & Gaur, G. S. (2014c). A randomized controlled trial to study the effect of yoga therapy on cardiac function and N terminal pro BNP in heart failure. Integrative Medicin Insights, 9, 1–6. https://doi.org/10.4137/IMI.S13939
Laborde, S., Mosley, E., & Thayer, J. F. (2017). Heart rate variability and cardiac vagal tone in psychophysiological research–recommendations for experiment planning, data analysis, and data reporting. Frontiers in Psychology, 8, 213.
Lampert, R., Tuit, K., Hong, K.-I., Donovan, T., Lee, F., & Sinha, R. J. S. (2016). Cumulative stress and autonomic dysregulation in a community sample. Stress, 19, 269–279.
Lau, J., Ioannidis, J. P., Terrin, N., Schmid, C. H., & Olkin, I. (2006). The case of the misleading funnel plot. British Medical Journal, 333, 597–600. https://doi.org/10.1136/bmj.333.7568.597
Le, J., Dorstyn, D. S., Mpfou, E., Prior, E., & Tully, P. J. (2018). Health-related quality of life in coronary heart disease: A systematic review and meta-analysis mapped against the international classification of functioning, disability and health. Quality of Life Research, 27, 2491–2503. https://doi.org/10.1007/s11136-018-1885-5
Lehrer, P. M., & Gevirtz, R. (2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 756, 66.
Lehrer, P. M., Vaschillo, E., & Vaschillo, B. (2000). Resonant frequency biofeedback training to increase cardiac variability: Rationale and manual for training. Applied Psychophysiology and Biofeedback, 25, 177–191.
Limmer, A., Laser, M., & Schutz, A. (2022). Mobile heart rate variability biofeedback as a complementary intervention after myocardial infarction: A randomized controlled study. International Journal of Behavioral Medicine, 29, 230–239. https://doi.org/10.1007/s12529-021-10000-6
Lin, I. M., Fan, S. Y., Lu, H. C., Lin, T. H., Chu, C. S., Kuo, H. F., Lee, C. S., & Lu, Y. H. (2015). Randomized controlled trial of heart rate variability biofeedback in cardiac autonomic and hostility among patients with coronary artery disease. Behaviour Research and Therapy, 70, 38–46. https://doi.org/10.1016/j.brat.2015.05.001
Lipsey, M. W., & Wilson, D. B. (2001). Practical meta-analysis. SAGE.
Luskin, F., Reitz, M., Newell, K., Quinn, T. G., & Haskell, W. (2002). A controlled pilot study of stress management training of elderly patients with congestive heart failure. Preventive Cardiology, 5, 168–174.
Merz, C. N. (2001). Effects of meditation on mechanism of coronary heart disease. ClinicalTrials.gov.
Miller, W. R., Brown, J. M., Simpson, T. L., Handmaker, N. S., Bien, T. H., Luckie, L. F., Montgomery, H. A., Hester, R. K., & Tonigan, J. S. (1995). What works? A methodological analysis of the alcohol treatment outcome literature. Handbook of Alcoholism Treatment Approaches: Effective Alternatives, 6, 66.
Moher, D., Liberati, A., Tetzlaff, J., & Altman, D. G. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Annals of Internal Medicine, 151, 264–269. https://doi.org/10.1136/bmj.b2535
Morris, S. B., & DeShon, R. P. (2002). Combining effect size estimates in meta-analysis with repeated measures and independent-groups designs. Psychological Methods, 7, 105. https://doi.org/10.1037/1082-989X.7.1.105
Mortara, A., La Rovere, M. T., Pinna, G. D., Maestri, R., Capomolla, S., & Cobelli, F. (2000). Nonselective beta-adrenergic blocking agent, carvedilol, improves arterial baroflex gain and heart rate variability in patients with stable chronic heart failure. Journal of the American College of Cardiology, 36, 1612–1618.
Murgia, F., Melotti, R., Foco, L., Gögele, M., Meraviglia, V., Motta, B., Steger, A., Toifl, M., Sinnecker, D., Müller, A., & Merati, G. (2019). Effects of smoking status, history and intensity on heart rate variability in the general population: The CHRIS study. PLoS ONE, 14, e0215053.
Niemelä, M. J., Airaksinen, K. J., & Huikuri, H. V. (1994). Effect of beta-blockade on heart rate variability in patients with coronary artery disease. Journal of the American College of Cardiology, 23, 1370–1377.
Ohira, T., Roux, A. V. D., Prineas, R. J., Kizilbash, M. A., Carnethon, M. R., & Folsom, A. R. (2008). Associations of psychosocial factors with heart rate and its short-term variability: Multi-ethnic study of atherosclerosis. Psychosomatic Medicine, 70(2), 141–146.
Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., Brennan, S. E., & Chou, R. (2021). The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. British Medical Journal, 372, 66.
Paul-Labrador, M., Polk, D., Dwyer, J. H., Velasquez, I., Nidich, S., Rainforth, M., Schneider, R., & Merz, C. N. (2006). Effects of a randomized controlled trial of transcendental meditation on components of the metabolic syndrome in subjects with coronary heart disease. Archives of Internal Medicine, 166, 1218–1224. https://doi.org/10.1001/archinte.166.11.1218
Paul-Labrador, M. J., & Merz, C. N. (2003). Transcendental meditation improves insulin resistance in coronary artery disease subjects: A randomized controlled trial. Popular Science, 6, 66.
Pushpanathan, P., Madanmohan, T., & Swaminathan, R. P. (2011). Effect of 12 week yoga therapy on cardiac autonomic functions in patients of essential hypertension. Indian Journal of Physiology and Pharmacology, 55, 42–43.
Pushpanathan, P., Trakroo, M., Palamalai, S. R., Subramanian, S. K., Bhavanani, A. B., & Madhavan, C. (2015a). Randomized controlled trial of 12-week yoga therapy as lifestyle intervention in patients of essential hypertension and cardiac autonomic function tests. National Journal of Physiology, Pharmacy and Pharmacology, 6, 19–26. https://doi.org/10.5455/njppp.2015.5.2408201572
Pushpanathan, P., Trakroo, M., Swaminathan, R. P., & Madhavan, C. (2015b). Heart rate variability by Poincaré plot analysis in patients of essential hypertension and 12-week yoga therapy. National Journal of Physiology, Pharmacy and Pharmacology, 5, 174–180. https://doi.org/10.5455/njppp.2015.5.1012201412
Quintana, D. S. (2017). Statistical considerations for reporting and planning heart rate variability case–control studies. Psychophysiology, 54, 344–349.
Quintana, D., Alvares, G. A., & Heathers, J. (2016). Guidelines for Reporting Articles on Psychiatry and Heart rate variability (GRAPH): Recommendations to advance research communication. Translational Psychiatry, 6, e803–e803.
Quintana, D. S., & Heathers, J. A. (2014). Considerations in the assessment of heart rate variability in biobehavioral research. Frontiers in Psychology, 5, 805.
Richardson, S., Shaffer, J. A., Falzon, L., Krupka, D., Davidson, K. W., & Edmondson, D. (2012). Meta-analysis of perceived stress and its association with incident coronary heart disease. The American Journal of Cardiology, 110(12), 1711–1716.
Rosengren, A., Hawken, S., Ôunpuu, S., Sliwa, K., Zubaid, M., Almahmeed, W. A., Blackett, K. N., Sitthi-Amorn, C., Sato, H., & Yusuf, S. (2004). Association of psychosocial risk factors with risk of acute myocardial infarction in 11119 cases and 13648 controls from 52 countries (the INTERHEART study): Case–control study. The Lancet, 364, 953–962.
Roth, G. A., Johnson, C., Abajobir, A., Abd-Allah, F., Abera, S. F., Abyu, G., Ahmed, M., Aksut, B., Alam, T., Alam, K., & Alla, F. (2017). Global, regional, and national burden of cardiovascular diseases for 10 causes, 1990 to 2015. Journal of the American College of Cardiology, 70, 1–25. https://doi.org/10.1016/j.jacc.2017.04.052
Roth, G. A., Johnson, C. O., Abate, K. H., Abd-Allah, F., Ahmed, M., Alam, K., Alam, T., Alvis-Guzman, N., Ansari, H., Ärnlöv, J., & Atey, T. M. (2018). The burden of cardiovascular diseases among US states, 1990–2016. JAMA Cardiology, 3, 375–389. https://doi.org/10.1001/jamacardio.2018.0385
Russell, D. C., Smith, T. L., Krahn, D. D., Graskamp, P., Singh, D., Kolden, G. G., Sigmund, H., & Zhang, Z. (2015). Effects of cognitive behavioral stress management on negative mood and cardiac autonomic activity in ICD recipients. Pace-Pacing and Clinical Electrophysiology, 38, 951–965. https://doi.org/10.1111/pace.12668
Salmoirago-Blotcher, E., Hovey, K. M., Andrews, C. A., Allison, M., Brunner, R. L., Denburg, N. L., Eaton, C., Garcia, L., Sealy-Jefferson, S. M., Zaslavsky, O., & Kang, J. (2019). Psychological traits, heart rate variability, and risk of coronary heart disease in healthy aging women–the Women’s Health Initiative. Psychosomatic Medicine, 81, 256.
Scott-Sheldon, L. A., Gathright, E. C., Donahue, M. L., Balletto, B., Feulner, M. M., DeCosta, J., Cruess, D. G., Wing, R. R., Carey, M. P., & Salmoirago-Blotcher, E. (2020). Mindfulness-based interventions for adults with cardiovascular disease: A systematic review and meta-analysis. Annals of Behavioral Medicine, 54, 67–73. https://doi.org/10.1093/abm/kaz020
Shaffer, F., & Ginsberg, J. P. (2017). An Overview of Heart Rate variability Metrics and Norms. Frontiers in Public Health, 5, 258. https://doi.org/10.3389/fpubh.2017.00258
Shaffer, F., McCraty, R., & Zerr, C. L. (2014). A healthy heart is not a metronome: an integrative review of the heart’s anatomy and heart rate variability. Frontiers in Psychology, 5, 1040. https://doi.org/10.3389/fpsyg.2014.01040
Sherwood, A. (2009). Coping Skills and Heart FailureL Outcomes and Mechanisms (COPE-HF). ClinicalTrials.gov.
Sherwood, A., Blumenthal, J. A., Koch, G. G., Hoffman, B. M., Watkins, L. L., Smith, P. J., O’Connor, C. M., Adams, K. F., Jr., Rogers, J. G., Sueta, C., & Chang, P. P. (2017). Effects of coping skills training on quality of life, disease biomarkers, and clinical outcomes in patients with heart failure: A randomized clinical trial. Circulation Heart Failure. https://doi.org/10.1161/CIRCHEARTFAILURE.116.003410
Sherwood, A., O’Connor, C. M., Routledge, F. S., Hinderliter, A. L., Watkins, L. L., Babyak, M. A., Koch, G. G., Adams, K. F., Jr., Dupree, C. S., Chang, P. P., & Hoffman, B. M. (2011). Coping effectively with heart failure (COPE-HF): Design and rationale of a telephone-based coping skills intervention. Journal of Cardiac Failure, 17, 201–207. https://doi.org/10.1016/j.cardfail.2010.11.001
Sin, N. L., Sloan, R. P., McKinley, P. S., & Almeida, D. M. (2016). Linking daily stress processes and laboratory-based heart rate variability in a national sample of midlife and older adults. Psychosomatic Medicine, 78, 573.
Sloan, R., & Bigger, J. J. (1991). Biobehavioral factors in Cardiac Arrhythmia Pilot Study (CAPS). Review and examination. Circulation, 83, 52–57.
Soares-Miranda, L., Sattelmair, J., Chaves, P., Duncan, G. E., Siscovick, D. S., Stein, P. K., & Mozaffarian, D. (2014). Physical activity and heart rate variability in older adults: The Cardiovascular Health Study. Circulation, 129, 2100–2110.
StataCorpLP. (2017). Stata statistical software. In (Version 16 for Windows).
Sterne, J. A., & Egger, M. (2001). Funnel plots for detecting bias in meta-analysis: Guidelines on choice of axis. Journal of Clinical Epidemiology, 54, 1046–1055. https://doi.org/10.1016/S0895-4356(01)00377-8
Swanson, K., Gevirtz, R., Brown, M., & Spira, J. (2007). Biofeedback increases heart rate variability in heart failure? Applied Psychophysiology and Biofeedback, 32, 59–59.
Swanson, K., Gevirtz, R., Brown, M., Spira, J., Guarneri, E., & Stoletniy, L. (2010). The effect of biofeedback on function in patients with heart failure. Applied Psychophysiology and Biofeedback, 35, 185–185.
Swanson, K. S., Gevirtz, R. N., Brown, M., Spira, J., Guarneri, E., & Stoletniy, L. (2009). The effect of biofeedback on function in patients with heart failure. Applied Psychophysiology and Biofeedback, 34, 71–91. https://doi.org/10.1007/s10484-009-9077-2
Task Force of the European Society of Cardiology the North American Society of Pacing Electrophysiology, T. F. E. S. C. N. A. S. P. (1996). Heart rate variability: Standards of measurement, physiological interpretation, and clinical use. European Heart Journal, 17, 354–381.
Virani, S. S., Alonso, A., Benjamin, E. J., Bittencourt, M. S., Callaway, C. W., Carson, A. P., Chamberlain, A. M., Chang, A. R., Cheng, S., Delling, F. N., & Djousse, L. (2021). Heart disease and stroke statistics—2021 update: A report from the American Heart Association. Circulation, 143, e254–e743.
Wang, L. S., Zhang, F., Liu, H. Y., & Lü, X. H. (2006). Influence of the biofeedback relaxation training on the heart rate variability of patients with coronary heart disease. Chinese Journal of Clinical Rehabilitation, 10, 13–15.
Yeh, G. Y., Mietus, J. E., Peng, C. K., Phillips, R. S., Davis, R. B., Wayne, P. M., Goldberger, A. L., & Thomas, R. J. (2008a). Enhancement of sleep stability with Tai Chi exercise in chronic heart failure: Preliminary findings using an ECG-based spectrogram method. Sleep Medicine, 9, 527–536. https://doi.org/10.1016/j.sleep.2007.06.003
Yeh, G. Y., Wayne, P. M., & Phillips, R. S. (2008b). T’ai Chi exercise in patients with chronic heart failure. Medicine and Sport Science, 52, 195–208. https://doi.org/10.1159/000134300
Yeh, G. Y., Wood, M. J., Lorell, B. H., Stevenson, L. W., Eisenberg, D. M., Wayne, P. M., Goldberger, A. L., & Davis, R. B. (2004). Effects of Tai Chi mind-body movement therapy on functional status and exercise capacity in patients with chronic heart failure: A randomized controlled trial. American Journal of Medicine, 117, 541–548.
Yu, L.-C., Lin, I. M., Fan, S.-Y., Chien, C.-L., & Lin, T.-H. (2018). One-year cardiovascular prognosis of the randomized, controlled, short-term heart rate variability biofeedback among patients with coronary artery disease. International Journal of Behavioral Medicine, 25, 271–282. https://doi.org/10.1007/s12529-017-9707-7
Funding
The research reported in this paper was supported by the National Center for Complementary and Integrative Health of the National Institutes of Health under award number 5R01AT008815 to Lori A. J. Scott-Sheldon, PhD and Michael P. Carey, PhD (Multiple PIs). Emily C. Gathright, PhD was supported by K23AG061214-01A1 from the National Institute on Aging. Elena Salmoirago-Blotcher, MD, was supported by National Institutes of Health grants R01AG076438 and R01HL149672 and Shufang Sun, PhD was supported by K23AT011173 from the National Center for Complementary and Integrative Health and the Adolescent/Young Adult Biobehavioral HIV Training Grant (T32MH078788; Larry K. Brown, PI) from the National Institute of Mental Health. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
ECG contributed equally to conceptualization, data curation, investigation, and served as lead in formal analysis and writing–original draft. JWH contributed equally to writing–review & editing, and served in a supporting role for conceptualization. SS served in a supporting role for writing-original draft and review & editing. LS contributed equally to data curation and investigation and served in a supporting role for writing–review & editing. JD contributed equally to data curation and investigation and served in a supporting role for validation and for writing–review & editing. BB contributed equally to data curation and investigation and served in a supporting role for writing–review & editing. MPC served as lead for conceptualization and funding acquisition, contributed equally to writing–review & editing and served in a supporting role for supervision. LAJS-S served as lead for conceptualization and funding acquisition, data curation, investigation, methodology, supervision, and served in a supporting role for writing–review & editing. ECS-B served as lead for writing-review & editing, contributed equally to conceptualization, supervision, and served in a supporting role for funding acquisition.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests relevant to the content of this article.
Ethical approval
Not applicable; this is a systematic review and meta-analysis of publicly available literature.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gathright, E.C., Hughes, J.W., Sun, S. et al. Effects of stress management interventions on heart rate variability in adults with cardiovascular disease: a systematic review and meta-analysis. J Behav Med 47, 374–388 (2024). https://doi.org/10.1007/s10865-024-00468-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10865-024-00468-4