Abstract
Background
Several novel technologies allowing catheter ablation (CA) with a favorable safety/efficacy profile have been recently developed, but not yet extensively clinically tested in the setting of ventricular tachycardia CA.
Methods
In this technical report, we overview technical aspects and preclinical/clinical information concerning the application of three novel CA technologies in the ventricular milieu: a pulsed field ablation (PFA) generator (CENTAURI™, Galaxy Medical) to be used with linear, contact force-sensing radiofrequency ablation catheters; a contact force-sensing radiofrequency ablation catheter equipped with six thermocouples and three microelectrodes (QDOT Micro™, Biosense-Webster), allowing high-resolution mapping and temperature-controlled CA; and a flexible and mesh-shaped irrigation tip, contact force-sensing radiofrequency ablation catheter (Tactiflex, Abbott). We also report three challenging VT cases in which CA was performed using these technologies.
Results
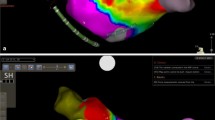
The CENTAURI system was used with the Tacticath™ (Abbott) ablation catheter to perform ventricular PFA in a patient with advanced heart failure, electrical storm, and a deep intramural septal substrate. Microelectrode mapping using QDOT Micro™ helped to refine substrate assessment in a VT patient with congenitally corrected transposition of the great arteries, and allowed the identification of the critical components of the VT circuit, which were successfully ablated. Tactiflex™ was used in two challenging CA cases (one endocardial and one epicardial), allowing acute and mid-term control of VT episodes without adverse events.
Conclusion
The ideation and development of novel technologies initially intended to treat atrial arrhythmias and successfully implemented in the ventricular milieu is contributing to the progressive improvement in the clinical benefits derived from VT CA, making this procedure key for successful management of increasingly complex patients.
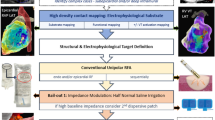
Graphical abstract





Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author, PC.
References
Hartzler GO. Electrode catheter ablation of refractory focal ventricular tachycardia. J Am Coll Cardiol. 1983;2(6):1107–13. https://doi.org/10.1016/s0735-1097(83)80337-4.
Guandalini GS, Liang JJ, Marchlinski FE. Ventricular tachycardia ablation: past, present, and future perspectives. JACC Clin Electrophysiol. 2019;5(12):1363–83. https://doi.org/10.1016/j.jacep.2019.09.015.
Cronin EM, Bogun FM, Maury P, Peichl P, Chen M, Namboodiri N, Aguinaga L, Leite LR, Al-Khatib SM, Anter E, Berruezo A, Callans DJ, Chung MK, Cuculich P, d’Avila A, Deal BJ, Bella PD, Deneke T, Dickfeld TM, Hadid C, Haqqani HM, Kay GN, Latchamsetty R, Marchlinski F, Miller JM, Nogami A, Patel AR, Pathak RK, Saenz Morales LC, Santangeli P, Sapp JL Jr, Sarkozy A, Soejima K, Stevenson WG, Tedrow UB, Tzou WS, Varma N, Zeppenfeld K. 2019 HRS/EHRA/APHRS/LAHRS expert consensus statement on catheter ablation of ventricular arrhythmias. J Interv Card Electrophysiol. 2020;59(1):145–298. https://doi.org/10.1007/s10840-019-00663-3.
Compagnucci P, Volpato G, Falanga U, Cipolletta L, Conti M, Grifoni G, Verticelli L, Schicchi N, Giovagnoni A, Casella M, Guerra F, Dello Russo A. Recent advances in three-dimensional electroanatomical mapping guidance for the ablation of complex atrial and ventricular arrhythmias. J Interv Card Electrophysiol. 2021;61(1):37–43. https://doi.org/10.1007/s10840-020-00781-3.
Marashly Q, Najjar SN, Hahn J, Rector GJ, Khawaja M, Chelu MG. Innovations in ventricular tachycardia ablation. J Interv Card Electrophysiol. 2022. https://doi.org/10.1007/s10840-022-01311-z. Epub ahead of print.
Dello Russo A, Compagnucci P, Bergonti M, Cipolletta L, Parisi Q, Volpato G, Santarelli G, Colonnelli M, Saenen J, Valeri Y, Carboni L, Marchese P, Marini M, Sarkozy A, Natale A, Casella M. Microelectrode voltage mapping for substrate assessment in catheter ablation of ventricular tachycardia: a dual-center experience. J Cardiovasc Electrophysiol. 2023;34(5):1216–27. https://doi.org/10.1111/jce.15908.
Schmidt B, Chen S, Tohoku S, Bordignon S, Bologna F, Chun KRJ. Single shot electroporation of premature ventricular contractions from the right ventricular outflow tract. Europace. 2022;24(4):597. https://doi.org/10.1093/europace/euab212.
Krause U, Bergau L, Zabel M, Müller MJ, Paul T. Flowerpower: pulsed field ablation of ventricular tachycardia in a patient with Ebstein’s anomaly. Eur Heart J Case Rep. 2023;7(3):ytad093. https://doi.org/10.1093/ehjcr/ytad093.
Ouss A, van Stratum L, van der Voort P, Dekker L. First in human pulsed field ablation to treat scar-related ventricular tachycardia in ischemic heart disease: a case report. J Interv Card Electrophysiol. 2023;66(3):509–10. https://doi.org/10.1007/s10840-022-01407-6.
Weyand S, Löbig S, Seizer P. First in human focal pulsed field ablation to treat an epicardial VT focus with an endocardial approach in non-ischemic cardiomyopathy. J Interv Card Electrophysiol. 2023;66(5):1057–8. https://doi.org/10.1007/s10840-023-01534-8.
Martin CA, Zaw MT, Jackson N, Morris D, Costanzo P. First worldwide use of pulsed-field ablation for ventricular tachycardia ablation via a retrograde approach. J Cardiovasc Electrophysiol. 2023;34(8):1772–5. https://doi.org/10.1111/jce.16002.
Verma A, Haines DE, Boersma LV, Sood N, Natale A, Marchlinski FE, Calkins H, Sanders P, Packer DL, Kuck KH, Hindricks G, Onal B, Cerkvenik J, Tada H, DeLurgio DB. PULSED AF Investigators. Pulsed field ablation for the treatment of atrial fibrillation: PULSED AF pivotal trial. Circulation. 2023;147(19):1422–32. https://doi.org/10.1161/CIRCULATIONAHA.123.063988.
Verma A, Asivatham SJ, Deneke T, Castellvi Q, Neal RE 2nd. Primer on pulsed electrical field ablation: understanding the benefits and limitations. Circ Arrhythm Electrophysiol. 2021;14(9):e010086. https://doi.org/10.1161/CIRCEP.121.010086.
Sandhu U, Alkukhun L, Kheiri B, Hodovan J, Chiang K, Splanger T, Castellvi Q, Zhao Y, Nazer B. In vivo pulsed-field ablation in healthy vs. chronically infarcted ventricular myocardium: biophysical and histologic characterization. Europace. 2023;25(4):1503–9. https://doi.org/10.1093/europace/euac252.
Compagnucci P, Casella M, Bianchi V, Franculli F, Vitali F, Santini L, Savarese G, Santobuono VE, Chianese R, Lavalle C, Amellone C, Pecora D, Calvanese R, Stronati G, Santoro A, Ziacchi M, Campari M, Valsecchi S, Calò L, Guerra F, Dello Russo A. Implantable defibrillator-detected heart failure status predicts ventricular tachyarrhythmias. J Cardiovasc Electrophysiol. 2023;34(5):1257–67. https://doi.org/10.1111/jce.15898.
Im SI, Higuchi S, Lee A, Stillson C, Buck E, Morrow B, Schenider K, Speltz M, Gerstenfeld EP. Pulsed field ablation of left ventricular myocardium in a swine infarct model. JACC Clin Electrophysiol. 2022;8(6):722–31. https://doi.org/10.1016/j.jacep.2022.03.007.
Tzou WS, Tung R, Frankel DS, Vaseghi M, Bunch TJ, Di Biase L, Tholakanahalli VN, Lakkireddy D, Dickfeld T, Saliaris A, Weiss JP, Mathuria N, Tedrow U, Afzal MR, Vergara P, Nagashima K, Patel M, Nakahara S, Vakil K, Burkhardt JD, Tseng CH, Natale A, Shivkumar K, Callans DJ, Stevenson WG, Della Bella P, Marchlinski FE, Sauer WH. Ventricular tachycardia ablation in severe heart failure: an international ventricular tachycardia ablation center collaboration analysis. Circ Arrhythm Electrophysiol. 2017;10(1):e004494. https://doi.org/10.1161/CIRCEP.116.004494.
Josephson ME, Anter E. Substrate mapping for ventricular tachycardia: assumptions and misconceptions. JACC Clin Electrophysiol. 2015;1(5):341–52. https://doi.org/10.1016/j.jacep.2015.09.001.
Takigawa M, Kitamura T, Basu S, Bartal M, Martin CA, Martin R, Cheniti G, Vlachos K, Pillois X, Frontera A, Massoullié G, Thompson N, Bourier F, Lam A, Duchateau J, Pambrun T, Denis A, Derval N, Cochet H, Haïssaguerre M, Sacher F, Hocini M, Jaïs P. Effect of electrode size and spacing on electrograms: optimized electrode configuration for near-field electrogram characterization. Heart Rhythm. 2022;19(1):102–12. https://doi.org/10.1016/j.hrthm.2021.09.011.
Compagnucci P, Dello Russo A, Bergonti M, Anselmino M, Zucchelli G, Gasperetti A, Cipolletta L, Volpato G, Ascione C, Ferraris F, Valeri Y, Bongiorni MG, Natale A, Tondo C, De Ferrari GM, Casella M. Ablation index predicts successful ablation of focal atrial tachycardia: results of a multicenter study. J Clin Med. 2022;11(7):1802. https://doi.org/10.3390/jcm11071802.
Vlachos K, Letsas KP, Srinivasan NT, Frontera A, Efremidis M, Dragasis S, Martin CA, Martin R, Nakashima T, Bazoukis G, Kitamura T, Mililis P, Saplaouras A, Georgopoulos S, Sofoulis S, Kariki O, Koskina S, Takigawa M, Sacher F, Jais P, Santangeli P. The value of functional substrate mapping in ventricular tachycardia ablation. Heart Rhythm O2. 2022;4(2):134–46. https://doi.org/10.1016/j.hroo.2022.10.013.
González-Lozano J, Ballesteros G, Cano J, Osorio D, Urbano C. Endocardial substrate of ventricular tachycardia in an adult patient with congenitally corrected transposition of great arteries without surgical repair. Pacing Clin Electrophysiol. 2023. https://doi.org/10.1111/pace.14756.
Ptaszek LM, Koruth J, Santangeli P, Piccini JP, Ranjan R, Mahapatra S, Pipenhagen C, Fish JM, Moon LB, Ambrosius NM, Boudlali H, Jensen JA. Safe and effective delivery of high-power, short-duration radiofrequency ablation lesions with a flexible-tip ablation catheter. Heart Rhythm O2. 2022;4(1):42–50. https://doi.org/10.1016/j.hroo.2022.10.009.
Dello Russo A, D’Angelo L, Compagnucci P, Cipolletta L, Parisi Q, Valeri Y, Campanelli F, Volpato G, Carboni L, Ciliberti G, Stronati GE, Barbarossa A, La Piscopia V, Bondavalli B, Guerra F, Natale A, Casella M. High-power short-duration catheter ablation of atrial fibrillation: is it really a new era? Comparison between new and old radiofrequency contact force-sensing catheters. J Interv Card Electrophysiol. 2023. https://doi.org/10.1007/s10840-023-01612-x. Epub ahead of print.
Yamaguchi J, Takigawa M, Goya M, Martin C, Amemiya M, Yamamoto T, Nishimura T, Nakamura R, Shirai Y, Tao S, Miyazaki S, Takahashi Y, Sasano T. Impact of tip design and thermocouple location on the efficacy and safety of radiofrequency application. J Interv Card Electrophysiol. 2023;66(4):885–96. https://doi.org/10.1007/s10840-022-01219-8.
Kim YG, Shim J, Boo KY, Kim DY, Lee KN, Choi JI, Kim YH. Slit-based irrigation catheters can reduce procedure-related ischemic stroke in atrial fibrillation patients undergoing radiofrequency catheter ablation. PLoS ONE. 2020;15(10):e0239339. https://doi.org/10.1371/journal.pone.0239339.
Mohanty S, Trivedi C, Di Biase L, Burkhardt JD, Della Rocca DG, Gianni C, MacDonald B, Mayedo A, Shetty SS, Zagrodzky W, Baqai F, Bassiouny M, Gallinghouse GJ, Horton R, Al-Ahmad A, Natale A. Endocardial scar-homogenization with vs without epicardial ablation in VT patients with ischemic cardiomyopathy. JACC Clin Electrophysiol. 2022;8(4):453–61. https://doi.org/10.1016/j.jacep.2021.12.011.
Hawson J, Anderson RD, Al-Kaisey A, Chieng D, Segan L, Watts T, Campbell T, Morton J, McLellan A, Kistler P, Voskoboinik A, Pathik B, Kumar S, Kalman J, Lee G. Functional assessment of ventricular tachycardia circuits and their underlying substrate using automated conduction velocity mapping. JACC Clin Electrophysiol. 2022;8(4):480–94. https://doi.org/10.1016/j.jacep.2021.12.013.
Sosa E, Scanavacca M, D’Avila A, Pilleggi F. A new technique to perform epicardial mapping in the electrophysiology laboratory. J Cardiovasc Electrophysiol. 1996;7:531–6. https://doi.org/10.1111/j.1540-8167.1996.tb00559.x.
De Martino G, Compagnucci P, Mancusi C, Vassallo E, Calvanese C, Della Ratta G, Librera M, Franciulli M, Marino L, Russo AD, Casella M. Stepwise endo-/epicardial catheter ablation for atrial fibrillation: the Mediterranea approach. J Cardiovasc Electrophysiol. 2021;32(8):2107–15. https://doi.org/10.1111/jce.15151.
Garg L, Daubert T, Lin A, Dhakal B, Santangeli P, Schaller R, Hyman MC, Kumareswaran R, Arkles J, Nazarian S, Lin D, Riley MP, Supple GE, Frankel DS, Zado E, Callans DJ, Marchlinski FE, Dixit S. Utility of prolonged duration endocardial ablation for ventricular arrhythmias originating from the left ventricular summit. JACC Clin Electrophysiol. 2022;8(4):465–76. https://doi.org/10.1016/j.jacep.2021.12.010.
Acknowledgements
Michela Colonnelli, BE; Giulia Santarelli, BE; Valentina La Piscopia, BE; and Barbara Bondavalli, BE, for help in the preparation of images.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Each patient provided his/her written informed consent.
Conflict of interest
A.D.R. is a consultant for Abbott Medical. A.N. is a consultant for Biosense Webster, Stereotaxis, and Abbott, and has received speaker honoraria/travel from Medtronic, Atricure, Biotronik, and Janssen. All other authors declared no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Compagnucci, P., Valeri, Y., Conti, S. et al. Technological advances in ventricular tachycardia catheter ablation: the relentless quest for novel solutions to old problems. J Interv Card Electrophysiol (2023). https://doi.org/10.1007/s10840-023-01705-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10840-023-01705-7