Abstract
Purpose
To investigate the impact of heterogeneity in patient indications or insemination protocols on neonatal outcomes of singletons following early rescue ICSI (rICSI) treatments.
Methods
A retrospective study was conducted. Propensity score matching and multivariable logistic regression were used to adjust for confounders and biases.
Results
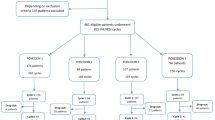
A total of 9095 IVF patients, 2063 ICSI patients, and 642 early rICSI patients were included in the study. No differences were detected in neonatal outcomes except small for gestational age (SGA) which increased in early rICSI patients compared with both unmatched and matched IVF groups with the risk ratio (RR) of 1.31 (95% CI: 1.05, 1.64) and 1.49 (95% CI: 1.05, 2.12). Further analysis showed that SGA increased significantly in partial fertilization failure (PFF) cycles with RRs of 1.56 (95% CI: 1.08, 2.27) and 1.78 (95% CI: 1.22, 2.59) compared with both unmatched and matched IVF patients but not in TFF patients. A positive association between fertilization rate via IVF and birth weight z-score was revealed in the PFF patients.
Conclusion
Early rICSI in patients with total fertilization failure (TFF) appeared to be safe in terms of neonatal outcomes. However, when expanding the indications of rICSI to PFF patients, the SGA in the offspring increased, suggesting a potential effect on long-term health. Since other treatment options, such as using only the IVF-origin embryos still exist for these patients, further studies were needed to confirm the optimal decision for these patients.

Similar content being viewed by others
Data availability
Not applicable.
References
ESHRE Special Interest Group of Embryology and Alpha Scientists in Reproductive Medicine. The Vienna consensus: report of an expert meeting on the development of ART laboratory performance indicators. Reprod Biomed Online. 2017;35(5):494–510.
Shinar S, et al. Total fertilization failure in intra-cytoplasmic sperm injection cycles–classification and management. Gynecol Endocrinol. 2014;30(8):593–6.
Combelles CM, et al. Diagnosing cellular defects in an unexplained case of total fertilization failure. Hum Reprod. 2010;25(7):1666–71.
Huang B, et al. Neonatal outcomes after early rescue intracytoplasmic sperm injection: an analysis of a 5-year period. Fertil Steril. 2015;103(6):1432-7.e1.
Paffoni A, et al. Should rescue ICSI be re-evaluated considering the deferred transfer of cryopreserved embryos in in-vitro fertilization cycles? A systematic review and meta-analysis. Reprod Biol Endocrinol. 2021;19(1):121.
Zhu X, et al. Clinical outcome of different embryo transfer strategies after late rescue ICSI procedure: a 10-year total fertilisation failure cohort study. BMC Pregnancy Childbirth. 2023;23(1):549.
Chen C, Kattera S. Rescue ICSI of oocytes that failed to extrude the second polar body 6 h post-insemination in conventional IVF. Hum Reprod. 2003;18(10):2118–21.
Chen L, et al. Neonatal outcome of early rescue ICSI and ICSI with ejaculated sperm. J Assist Reprod Genet. 2014;31(7):823–8.
Zeng J, et al. Fertilization and neonatal outcomes after early rescue intracytoplasmic sperm injection: a retrospective analysis of 16,769 patients. Arch Gynecol Obstet. 2022;306(1):249–58.
He Y, et al. Effect of early cumulus cells removal and early rescue ICSI on pregnancy outcomes in high-risk patients of fertilization failure. Gynecol Endocrinol. 2018;34(8):689–93.
Xiong F, et al. Perinatal and neonatal outcomes of pregnancies after early rescue intracytoplasmic sperm injection in women with primary infertility compared with conventional intracytoplasmic sperm injection: a retrospective 6-year study. BMC Pregnancy Childbirth. 2020;20(1):460.
Jiang L, et al. Effect of early rescue ICSI and split IVF-ICSI in preventing low fertilization rate during the first ART cycle: a real-world retrospective cohort study. Reprod Med Biol. 2022;21(1): e12420.
Kong P, et al. Effects of early cumulus cell removal on treatment outcomes in patients undergoing in vitro fertilization: a retrospective cohort study. Front Endocrinol (Lausanne). 2021;12: 669507.
Zhu J, et al. Association between etiologic factors in infertile couples and fertilization failure in conventional in vitro fertilization cycles. Andrology. 2015;3(4):717–22.
Blanc AK, Wardlaw T. Monitoring low birth weight: an evaluation of international estimates and an updated estimation procedure. Bull World Health Organ. 2005;83(3):178–85.
Jiang X, et al. Predicting the unexpected total fertilization failure in conventional in vitro fertilization cycles: what is the role of semen quality? Front Cell Dev Biol. 2023;11:1133512.
ASIR Medicine ESIG Embryology. Istanbul consensus workshop on embryo assessment: proceedings of an expert meeting. Reprod Biomed Online. 2011;22(6):632–46.
Zhu L, et al. Chinese neonatal birth weight curve for different gestational age. Zhonghua Er Ke Za Zhi. 2015;53(2):97–103.
Repping S, et al. Use of the total motile sperm count to predict total fertilization failure in in vitro fertilization. Fertil Steril. 2002;78(1):22–8.
Krog M, et al. Fertilization failure after IVF in 304 couples–a case-control study on predictors and long-term prognosis. Eur J Obstet Gynecol Reprod Biol. 2015;184:32–7.
Li J, et al. Development a nomogram to predict fertilisation rate of infertile males with borderline semen by using semen parameters combined with AMH and INHB. Andrologia. 2021;53(9): e14182.
Tian T, et al. Prediction of fertilization disorders in the in vitro fertilization/intracytoplasmic sperm injection: a retrospective study of 106,728 treatment cycles. Front Endocrinol (Lausanne). 2022;13: 870708.
Wang Q, et al. Nomogram models to predict low fertilisation rate and total fertilisation failure in patients undergoing conventional IVF cycles. BMJ Open. 2022;12(11): e067838.
Coticchio G, et al. The destinies of human embryos reaching blastocyst stage between Day 4 and Day 7 diverge as early as fertilization. Hum Reprod. 2023;38(9):1690–9.
Liu L, et al. Clinical outcome of cycles with oocyte degeneration after intracytoplasmic sperm injection. Syst Biol Reprod Med. 2017;63(2):113–9.
Liu L, et al. Oocyte degeneration in a cohort adversely affects clinical outcomes in conventional IVF cycles: a propensity score matching study. Front Endocrinol (Lausanne). 2023;14:1164371.
Scaravelli G, et al. Fertilization rate as a novel indicator for cumulative live birth rate: a multicenter retrospective cohort study of 9,394 complete in vitro fertilization cycles. Fertil Steril. 2021;116(3):766–73.
Du M, et al. Clinical and neonatal outcomes of children born after ICSI with or without surgically acquired sperm: a retrospective cohort study. Front Endocrinol (Lausanne). 2021;12: 788050.
Catford SR, et al. Long-term follow-up of ICSI-conceived offspring compared with spontaneously conceived offspring: a systematic review of health outcomes beyond the neonatal period. Andrology. 2018;6(5):635–53.
Ma NZ, et al. The influence of male age on treatment outcomes and neonatal birthweight following assisted reproduction technology involving intracytoplasmic sperm injection (ICSI) cycles. Andrologia 2018;50(1):e12826.
Anderson RE, et al. Do paternal semen parameters influence the birth weight or BMI of the offspring? A study from the Utah population database. J Assist Reprod Genet. 2018;35(5):793–9.
Hessami K, et al. Fetal reduction of triplet pregnancies to twins vs singletons: a meta-analysis of survival and pregnancy outcome. Am J Obstet Gynecol. 2022;227(3):430-439.e5.
Joseph KS, Kramer MS. The fetuses-at-risk approach: survival analysis from a fetal perspective. Acta Obstet Gynecol Scand. 2018;97(4):454–65.
Acknowledgements
We appreciate all clinicians, embryologists, and nurses of the Reproductive Medicine Center, Xiamen University Affiliated Chenggong Hospital for their treatments provided to the infertile couples included in the study.
Funding
This work was supported by the Natural Science Foundation of Xiamen Municipality, China (grant no. 3502Z202373122); the National Natural Science Foundation of China (grant no. 22176159); and the Xiamen Medical Advantage subspecialty construction project (grant no. 2018296).
Author information
Authors and Affiliations
Contributions
JG, XJ, JC, LL, and JR contribute to the conception, design, and manuscript. XJ, LO, CY, KC, XY, ZL, and JC contribute to the acquisition of data. JG, XJ, CM, and JC contribute to the analysis and interpretation of data. All authors read and approved the manuscript; all data were generated in-house, and no paper mill was used.
Corresponding author
Ethics declarations
Ethical approval
The study was approved by the Institutional Review Board from the Ethical Committee of the Medical College Xiamen University.
Consent to participate
Informed consent was unnecessary because the research was based on non-identifiable records approved by the ethics committee.
Consent for publication
Informed consent was unnecessary because the research was based on non-identifiable records approved by the ethics committee.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Geng, J., Cai, J., Ouyang, L. et al. Indications affect neonatal outcomes following early rescue ICSI: a retrospective study. J Assist Reprod Genet 41, 661–672 (2024). https://doi.org/10.1007/s10815-024-03040-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-024-03040-w