Abstract
Background
The prevalence of sleep disordered breathing is high in patients with end-stage renal disease. Salt intake is related to the severity of obstructive sleep apnea in patients with resistant hypertension and hyperaldosteronism. We investigated the relationship between salt intake and sleep disordered breathing in patients on maintenance hemodialysis.
Patients and methods
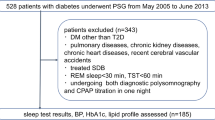
We studied 128 dialysis outpatients (mean age 63 ± 11 years) who were followed at Kokura Daiichi Hospital. We estimated each patient's salt intake using an InBody S10 body composition analyzer and measured the 3% oxygen desaturation index (ODI) during sleep using a Pulsewatch: PMP-200 GplusX.
Results
The average estimated salt intake was 8.0 ± 2.6 g/day, and the median value of that was 7.5 g/day. Blood pressure (BP) before and after dialysis were 140 ± 18/78 ± 11 and 127 ± 13/72 ± 8 mmHg, respectively. The geometric average number of 3% ODI was 7.1, and sleep disordered breathing was detected in 30% of all subjects. The patients with ≥ 7.5 g/day salt intake were younger and more frequently male and had higher body mass index (BMI) and BP before dialysis compared to those with salt intakes < 7.5 g/day. Patients with ≥ 7.5 g/day salt intake had a significantly higher geometric average number of 3% ODI; however, this relationship became weaker after adjusting for BMI. The same relationship was obtained for the prevalence of sleep disordered breathing.
Conclusion
The prevalence of sleep disordered breathing in patients on maintenance hemodialysis was high, and the sleep disordered breathing was associated with salt intake and BMI.




Similar content being viewed by others
References
Uemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42(9):1297–9.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018; 71 (6): e13-e115, 2018.
The Ministry of Health, Labour, and Welfare. The results of the 2017 National Health and Nutrition Survey in Japan. https://www.mhlw.go.jp/content/10904750/000351576.pdf.
Initiative KDOQ, (K, DOQI), . K/DOQI clinical practice guidelines on hypertension and antihypertensive agents in chronic kidney disease. Am J Kidney Dis. 2004;43(5 Suppl 1):S1–290.
Fouque D, Vennegoor M, Wee P, Wanner C, Basci A, Canaud B, et al. EBPG guideline on nutrition. Nephrol Dial Transplant. 2007;22(Suppl 2):ii45–87.
Ohta Y, Ishizuka A, Nakamura S, Shoubu A, Nakatani K, Nakamura H, et al. Salt intake and the awareness of salt restriction in dialysis patients. Ketsuatu. 2015;22(8):50–5 ((in Japanese)).
Pimenta E, Stowasser M, Gordon RD, Harding SM, Batlouni M, Zhang B, et al. Increased dietary sodium is related to severity of obstructive sleep apnea in patients with resistant hypertension and hyperaldosteronism. Chest. 2013;143(4):978–83.
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V. Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med. 2005;353(19):2034–41.
Gottlieb DJ, Yenokyan G, Newman AB, O’Connor GT, Punjabi NM, Quan SF, et al. Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure: The Sleep Heart Health Study. Circulation. 2010;122(4):352–60.
Sim JJ, Rasgon SA, Derose SF. Review article: managing sleep apnoea in kidney diseases. Nephrology. 2010;15(2):146–52.
Ezzat H, Mohab A. Prevalence of sleep disorders among ESRD patients. Ren Fail. 2015;37(6):1013–9.
Tang SC, Lam B, Lai AS, Pang CB, Tso WK, Khong PL, et al. Improvement in sleep apnea during nocturnal peritoneal dialysis is associated with reduced airway congestion and better uremic clearance. Clin J Am Soc Nephrol. 2009;4(2):410–8.
Beecroft JM, Hoffstein V, Pierratos A, Chan CT, McFarlane PA, Hanly PJ. Pharyngeal narrowing in end-stage renal disease: implications for obstructive sleep apnoea. Eur Respir J. 2007;30(5):965–71.
Tang SC, Lam B, Lam JC, Chan CK, Chow CC, Ho YW, et al. Impact of nephrotic edema of the lower limbs on obstructive sleep apnea: gathering a unifying concept for the pathogenetic role of nocturnal rostral fluid shift. Nephrol Dial Transplant. 2012;27(7):2788–94.
Ogna A, Ogna VF, Mihalache A, Pruijm M, Halabi G, Phan O, et al. Obstructive sleep apnea severity and overnight body fluid shift before and after hemodialysis. Clin J Am Soc Nephrol. 2015;10(6):1002–10.
Roumelioti ME, Brown LK, Unruh ML. The relationship between volume overload in end-stage renal disease and obstructive sleep apnea. Semin Dial. 2015;28(5):508–13.
Ikeda H, Kashihara K, Ono M, Ochiai M, Hamaguchi N, Fujikura J, et al. Calculation of estimated nutrition intake based on clinical laboratory tests in hemodialysis patients. J Kagawa Nutr Univ (Joshi Eiyo Daigaku Kiyou). 2005;36:27–35 ((in Japanese)).
Krikken JA, Laverman GD, Navis G. Benefits of dietary sodium restriction in the management of chronic kidney disease. Curr Opin Nephrol Hypertens. 2009;18(6):531–8.
Welch JL, Bennett SJ, Delp RL, Agarwal R. Benefits of and barriers to dietary sodium adherence. West J Nurs Res. 2006;28(2):162–80.
Ng K, Woo J, Kwan M, Sea M, Wang A, Lo R, et al. Effect of age and disease on taste perception. J Pain Symptom Manage. 2004;28(1):28–34.
Ozkahya M, Ok E, Toz H, Asci G, Duman S, Basci A, et al. Long-term survival rates in haemodialysis patients treated with strict volume control. Nephrol Dial Transplant. 2006;21(12):3506–13.
Hecking M, Moissl U, Genser B, Rayner H, Dasgupta I, Stuard S, et al. Greater fluid overload and lower interdialytic weight gain are independently associated with mortality in a large international hemodialysis population. Nephrol Dial Transplant. 2018;33(10):1832–42.
Mirrakhimov AE. Supine fluid redistribution: should we consider this as an important risk factor for obstructive sleep apnea? Sleep Breath. 2013;17(2):511–23.
Gaddam K, Pimenta E, Thomas SJ, Cofield SS, Oparil S, Harding SM, et al. Spironolactone reduces severity of obstructive sleep apnoea in patients with resistant hypertension: a preliminary report. J Hum Hypertens. 2010;24(8):532–7.
Kasai T, Arcand J, Allard JP, Mak S, Azevedo ER, Newton GE, et al. Relationship between sodium intake and sleep apnea in patients with heart failure. J Am Coll Cardiol. 2011;58(19):1970–4.
Bucca CB, Brussino L, Battisti A, Mutani R, Rolla G, Mangiardi L, et al. Diuretics in obstructive sleep apnea with diastolic heart failure. Chest. 2007;132(2):440–6.
Ling IT, James AL, Hillman DR. Interrelationships between body mass, oxygen desaturation, and apnea-hypopnea indices in a sleep clinic population. Sleep. 2012;35(1):89–96.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no conflict of interest exists.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee at which the studies were conducted (IRB approval number 17-No.1) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Ohta, Y., Yamaguchi, M., Yoshimoto, M. et al. Relationship between salt intake and sleep disordered breathing in dialysis patients. Clin Exp Nephrol 25, 1354–1359 (2021). https://doi.org/10.1007/s10157-021-02106-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-021-02106-8