Abstract
Background
Platelet-rich plasma (PRP), a cytokine therapy, concentrates the growth factors in platelets and is considered independent of platelet function. We compared the effectiveness of cell-free PRP cytokine (PRP-C) and ordinary PRP therapies on skin rejuvenation.
Methods
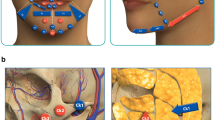
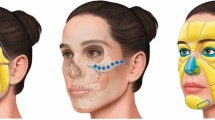
We selected 1340 patients (125 men and 1215 women) who received facial treatment from February 2020 to June 2022. PRP (n = 705) or PRP-C (n = 635) therapies were chosen by the patient; 6 ml of the substance was administered intradermally or subcutaneously. PRP was prepared from peripheral blood using sodium citrate solution and centrifugation and was used directly, or further frozen and centrifuged and the lysate was used as PRP-C.
Results
Patient satisfaction improved significantly after 4 and 8 weeks of treatment in both the PRP and PRP-C therapy groups (p < 0.0001 for all four values). No significant difference was reported in the therapeutic effect between the two treatment groups after 4 and 8 weeks (p = 0.119 and p = 0.6686, respectively).
Doctor evaluation efficacy of both therapies improved at both time points (p < 0.0001 for all four values). However, at 4 weeks, doctors estimated a more significant improvement in the PRP therapy group than in the PRP-C group; 8 weeks later, no significant differences were observed.
Conclusions
Both therapies improved skin texture and elasticity. The efficacy rate was greater than the improvement for wrinkles. The effectiveness of nasolabial lines and facial lift was not significant. PRP-C therapy can be used as cell-free therapy.
Level of evidence: level III, therapeutic study






Similar content being viewed by others
References
Uitto J, Matsuoka LY, Kornberg RL (1986) Elastic fibers in cutaneous elastoses. In: Rudolph R (ed) Problems in Aesthetic Surgery: Biological Causes and Clinical Solutions. Mosby, Mosby, St Louis MO, pp 307–338
Scharffetter-Kochanek K, Brenneisen P, Wenk J et al (2000) Photoaging of the skin from phenotype to mechanisms. Exp Gerontol 35:307–316
Avadhani KS, Manikkath J, Tiwari M, Chandrasekhar M, Godavarthi A, Vidya SM, Hariharapura RC, Kalthur G, Udupa N, Mutalik S (2017) Skin delivery of epigallocatechin-3-gallate [EGCG] and hyaluronic acid loaded nano-transfersomes for antioxidant and anti-aging effects in UV radiation induced skin damage. Drug Deliv 21:64–71. https://doi.org/10.1080/10717544.2016.1228718
Amable PR, Carias RBV, Teixeira MVT, da Cruz Pacheco I, do Amaral RJFC, Granjeiro JM, Borojevic R (2013) Platelet-rich plasma preparation for regenerative medicine: optimization and quantification of cytokines and growth factors. Stem Cell Res Ther 4:1–3. https://doi.org/10.1186/scrt218
Crovetti G, Martinelli G, Issi M, Barone M, Guizzardi M, Campanati B, Moroni M, Carabelli A (2004) Platelet gel for healing cutaneous chronic wounds. Transfus Apher Sci 30:145–151. https://doi.org/10.1016/j.transci.2004.01.004
Philippart P, Brasseur M, Hoyaux D, Pochet R (2003) Human recombinant tissue factor, platelet-rich plasma, and tetracycline induce a high-quality human bone graft: a 5-year survey. Int J Oral Maxillofac Implants 18:411–416
Anitua E (1999) Plasma rich in growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants 14:529–535
Moake JL, Turner NA, Stathopoulos NA, Nolasco L, Hellumus JD (1988) Shear-induced @latelet aggregation can be mediated by vWF released from platelets, as well as by exogenous large or unusually large vWF multimers, requires adenosine diphosphate, and is resistant to aspirin. Blood 71:1366–1374
Mody NA, King MR (2008) Platelet adhesive dynamics. Part II Biophys J 95:2556–2574
Chan CHH, Inoue M, Ki KK, Murashige T, Fraser JF, Simmonds MJ, Tansley GD, Watanabe N (2020) Shear-dependent platelet aggregation size. Artific Orgam 44:1286–1295
Menitove JE, Frenzke M, Aster RH (1986) Use of PGE1 for preparation of platelet concentrates. Transfusion 26:346–350. https://doi.org/10.1046/j.1537-2995.1986.26486262742.x
Kamakura T, Kataoka J, Maeda K, Teramachi H, Mihara H, Miyata K, Ooi K, Sasaki N, Kobayashi M, Ito K (2015) Platelet-rich plasma with basic fibroblast growth factor for treatment of wrinkles and depressed areas of the skin. Plast Reconstr Surg 136:931–939. https://doi.org/10.1097/PRS.0000000000001705
Juncan AM, Moisă DG, Santini A, Morgovan C, Rus LL, Vonica-Tincu AL, Loghin F (2021) Advantages of hyaluronic acid and its combination with other bioactive ingredients in cosmeceuticals molecules. Molecules 26:4429. https://doi.org/10.3390/molecules26154429
Tonnard P, Verpaele A, Carvas M (2020) Fat grafting for facial rejuvenation with nanofat grafts. Clin Plast Surg 47:43–62. https://doi.org/10.1016/j.cps.2019.08.006
Borges J, Araújo L, Cuzzi T, Martinez L, Gonzales Y, Manela-Azulay M (2020) Fractional laser resurfacing treats photoaging by promoting neocollegenesis and cutaneous edema. J Clin Aesthet Dermatol 13:22–27
Banihashemi M, Zabolinejad N, Salehi M, Hamidi Alamdari D, Nakhaizadeh S (2021) Platelet-rich Plasma use for facial rejuvenation: a clinical trial and review of current literature. Acta Biomed 92:e2021187. https://doi.org/10.23750/abm.v92i2.9687
Charles-de-Sá L, Gontijo-de-Amorim NF, Takiya CM, Borojevic R, Benati D, Bernardi P, Sbarbati A, Rigotti G (2018) Effect of use of platelet-rich plasma (PRP) in skin with intrinsic aging process. Aesthet Surg J 38:321–338. https://doi.org/10.1093/asj/sjx137
Zhao L, Hu M, Xiao Q, Zhou R, Li Y, Xiong L, Li L (2021) Efficacy and safety of platelet-rich plasma in melasma: a systematic review and meta-analysis. Dermatol Ther 11:1587–1597. https://doi.org/10.1007/s13555-021-00575-z
da Silva LQ, Cancela RBB, de Lima Montalvão SA, Huber SC, Vieira-Damiani G, Triglia RM, Annichino-Bizzacchi JM (2021) The effect of lyophilized platelet rich-plasma on skin aging: a non-randomized, controlled, pilot trial. Arch Dermatol Res 313:863–871. https://doi.org/10.1007/s00403-021-02186-2
Noh TK, Choi SJ, Chung BY, Kang JS, Lee JH, Lee MW, Chang SE (2014) Inflammatory features of melasma lesions in Asian skin. J Dermatol 41:788–794. https://doi.org/10.1111/1346-8138.12573
Okazaki M, Yoshimura K, Uchida G, Harii K (2005) Correlation between age and the secretions of melanocyte-stimulating cytokines in cultured keratinocytes and fibroblasts. Br J Dermatol 153(Suppl 2):23–29. https://doi.org/10.1111/j.1365-2133.2005.06966.x
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was reviewed by The Technical Advisor Group of the Extraordinary Certified Committee for Regenerative Medicine of Yukeikai (Ref. No. NA8200002) recognized by the Safety of Regenerative Medicine Act regulated by the Ministry of Health, Labour, and Welfare based on, and then approved (Approval Nos. PC3200287, PC3200288, PC3200289, PC3200290, PC3200271, PC3210061, PC3210213).
Consent to participate
Informed consent was obtained from all patients for the inclusion of their data (clinical and patient-reported outcomes) for the purpose of publication.
Consent for publication
The authors affirm that the human research participants provided informed consent for the publication of the images in Figs. 1, 2, and 3.
Competing interests
Hirose Yoshie, Fujita Chiharu, Aoki Akira, and Inoue Hajime declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hirose, Y., Fujita, C., Aoki, A. et al. A comparative study on the influences of platelet-rich plasma vs its derived cytokines on skin rejuvenation. Eur J Plast Surg 46, 725–732 (2023). https://doi.org/10.1007/s00238-023-02063-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-023-02063-3