Abstract
Purpose
Anti-obesity therapy can reduce body weight; however, it is not clear whether it can reduce major adverse cardiovascular events (MACEs). We conducted a systematic review and meta-analysis to assess the effect of long-term anti-obesity drugs on MACEs in individuals with overweight or obesity.
Methods
The MEDLINE, Embase, and Cochrane Library databases and clinical trial registries (https://clinicaltrials.gov) were searched up to 3 May 2021 for randomized controlled trials (RCT) that compared anti-obesity drugs with controls and reported cardiovascular events in subjects with overweight or obesity. Heterogeneity was described by the I2 value. The Mantel–Haenszel randomized effects model was adopted to calculate risk ratios (RR) and weighted mean differences (WMD). Sensitivity analysis was used to assess the stability of the effects. Publication bias was assessed by Begg's funnel plot and Egger's test. The Cochrane Collaboration risk-of-bias tool was used to evaluate the bias of each included RCT.
Results
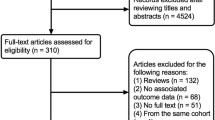
Twelve articles were included; 21,391 and 17,618 subjects were in the anti-obesity drug and placebo groups, respectively. There was no difference in MACEs between the anti-obesity drug and placebo groups (RR 0.99; 95% CI: 0.88–1.12). Compared with placebo, anti-obesity interventions reduced body weight (WMD: − 3.96 kg; 95% CI: − 4.89, − 3.03) and improved lipid and blood glucose profiles. The intervention also did not increase the incidence of depression or anxiety or the risk of suicidal ideation.
Conclusion
Long-term anti-obesity drugs did not show a benefit in lowering MACEs in overweight or obese subjects, although the drugs resulted in a decrease in body weight and improved cardiometabolic parameters.



Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
World Health Organization.Obesity and Overweight Fact Sheet. https://www.who.int/en/news-room/fact-sheets/detail/obesity-and-overweight. Accessed January 1
Bogers RP, Bemelmans WJ, Hoogenveen RT, Boshuizen HC, Woodward M, Knekt P, van Dam RM, Hu FB, Visscher TL, Menotti A, Thorpe RJ Jr, Jamrozik K, Calling S, Strand BH, Shipley MJ, Investigators B-CC (2007) Association of overweight with increased risk of coronary heart disease partly independent of blood pressure and cholesterol levels: a meta-analysis of 21 cohort studies including more than 300 000 persons. Arch Intern Med 167(16):1720–1728. https://doi.org/10.1001/archinte.167.16.1720
Piche ME, Poirier P, Lemieux I, Despres JP (2018) Overview of Epidemiology and Contribution of Obesity and Body Fat Distribution to Cardiovascular Disease: An Update. Prog Cardiovasc Dis 61(2):103–113. https://doi.org/10.1016/j.pcad.2018.06.004
Koliaki C, Liatis S, Kokkinos A (2019) Obesity and cardiovascular disease: revisiting an old relationship. Metabolism 92:98–107. https://doi.org/10.1016/j.metabol.2018.10.011
Collaborators GBDO, Afshin A, Forouzanfar MH, Reitsma MB, Sur P, Estep K, Lee A, Marczak L, Mokdad AH, Moradi-Lakeh M, Naghavi M, Salama JS, Vos T, Abate KH, Abbafati C, Ahmed MB, Al-Aly Z, Alkerwi A, Al-Raddadi R, Amare AT, Amberbir A, Amegah AK, Amini E, Amrock SM, Anjana RM, Arnlov J, Asayesh H, Banerjee A, Barac A, Baye E, Bennett DA, Beyene AS, Biadgilign S, Biryukov S, Bjertness E, Boneya DJ, Campos-Nonato I, Carrero JJ, Cecilio P, Cercy K, Ciobanu LG, Cornaby L, Damtew SA, Dandona L, Dandona R, Dharmaratne SD, Duncan BB, Eshrati B, Esteghamati A, Feigin VL, Fernandes JC, Furst T, Gebrehiwot TT, Gold A, Gona PN, Goto A, Habtewold TD, Hadush KT, Hafezi-Nejad N, Hay SI, Horino M, Islami F, Kamal R, Kasaeian A, Katikireddi SV, Kengne AP, Kesavachandran CN, Khader YS, Khang YH, Khubchandani J, Kim D, Kim YJ, Kinfu Y, Kosen S, Ku T, Defo BK, Kumar GA, Larson HJ, Leinsalu M, Liang X, Lim SS, Liu P, Lopez AD, Lozano R, Majeed A, Malekzadeh R, Malta DC, Mazidi M, McAlinden C, McGarvey ST, Mengistu DT, Mensah GA, Mensink GBM, Mezgebe HB, Mirrakhimov EM, Mueller UO, Noubiap JJ, Obermeyer CM, Ogbo FA, Owolabi MO, Patton GC, Pourmalek F, Qorbani M, Rafay A, Rai RK, Ranabhat CL, Reinig N, Safiri S, Salomon JA, Sanabria JR, Santos IS, Sartorius B, Sawhney M, Schmidhuber J, Schutte AE, Schmidt MI, Sepanlou SG, Shamsizadeh M, Sheikhbahaei S, Shin MJ, Shiri R, Shiue I, Roba HS, Silva DAS, Silverberg JI, Singh JA, Stranges S, Swaminathan S, Tabares-Seisdedos R, Tadese F, Tedla BA, Tegegne BS, Terkawi AS, Thakur JS, Tonelli M, Topor-Madry R, Tyrovolas S, Ukwaja KN, Uthman OA, Vaezghasemi M, Vasankari T, Vlassov VV, Vollset SE, Weiderpass E, Werdecker A, Wesana J, Westerman R, Yano Y, Yonemoto N, Yonga G, Zaidi Z, Zenebe ZM, Zipkin B, Murray CJL (2017) Health Effects of Overweight and Obesity in 195 Countries over 25 Years. N Engl J Med 377(1):13–27. https://doi.org/10.1056/NEJMoa1614362
Baranowski T, O’Connor T, Johnston C, Hughes S, Moreno J, Chen TA, Meltzer L, Baranowski J (2014) School year versus summer differences in child weight gain: a narrative review. Child Obes 10(1):18–24. https://doi.org/10.1089/chi.2013.0116
Vafa M, Heshmati J, Sadeghi H, Shidfar F, Namazi N, Baradaran H, Heydarpour B, Jalili Z (2016) Is exclusive breastfeeding and its duration related to cardio respiratory fitness in childhood? J Matern Fetal Neonatal Med 29(3):461–465. https://doi.org/10.3109/14767058.2015.1004052
Bonaccio M, Di Castelnuovo A, Costanzo S, De Curtis A, Persichillo M, Sofi F, Cerletti C, Donati MB, de Gaetano G, Iacoviello L (2021) Ultra-processed food consumption is associated with increased risk of all-cause and cardiovascular mortality in the Moli-sani Study. Am J Clin Nutr 113(2):446–455. https://doi.org/10.1093/ajcn/nqaa299
Juul F, Vaidean G, Lin Y, Deierlein AL, Parekh N (2021) Ultra-processed foods and incident cardiovascular disease in the framingham offspring study. J Am Coll Cardiol 77(12):1520–1531. https://doi.org/10.1016/j.jacc.2021.01.047
Askari M, Heshmati J, Shahinfar H, Tripathi N, Daneshzad E (2020) Ultra-processed food and the risk of overweight and obesity: a systematic review and meta-analysis of observational studies. Int J Obes (Lond) 44(10):2080–2091. https://doi.org/10.1038/s41366-020-00650-z
Garvey WT, Mechanick JI, Brett EM, Garber AJ, Hurley DL, Jastreboff AM, Nadolsky K, Pessah-Pollack R, Plodkowski R, Reviewers of the AACEOCPG (2016) American Association of Clinical Endocrinologists and American College of Endocrinology Comprehensive Clinical Practice Guidelines for Medical Care of Patients with Obesity. Endocr Pract 22(Suppl 3):1–203. https://doi.org/10.4158/EP161365.GL
Wadden TA, Hollander P, Klein S, Niswender K, Woo V, Hale PM, Aronne L, Investigators NN (2013) Weight maintenance and additional weight loss with liraglutide after low-calorie-diet-induced weight loss: the SCALE Maintenance randomized study. Int J Obes (Lond) 37(11):1443–1451. https://doi.org/10.1038/ijo.2013.120
Sweeting AN, Tabet E, Caterson ID, Markovic TP (2014) Management of obesity and cardiometabolic risk - role of phentermine/extended release topiramate. Diabetes Metab Syndr Obes 7:35–44. https://doi.org/10.2147/DMSO.S38979
Crawford AR, Alamuddin N, Amaro A (2018) Cardiometabolic Effects of Anti-obesity Pharmacotherapy. Curr Atheroscler Rep 20(4):18. https://doi.org/10.1007/s11883-018-0719-9
Khera R, Pandey A, Chandar AK, Murad MH, Prokop LJ, Neeland IJ, Berry JD, Camilleri M, Singh S (2018) Effects of Weight-Loss Medications on Cardiometabolic Risk Profiles: A Systematic Review and Network Meta-analysis. Gastroenterology 154 (5): 1309–1319 e1307. https://doi.org/10.1053/j.gastro.2017.12.024
Allison DB, Gadde KM, Garvey WT, Peterson CA, Schwiers ML, Najarian T, Tam PY, Troupin B, Day WW (2012) Controlled-release phentermine/topiramate in severely obese adults: a randomized controlled trial (EQUIP). Obesity (Silver Spring) 20(2):330–342. https://doi.org/10.1038/oby.2011.330
Apovian CM, Aronne L, Rubino D, Still C, Wyatt H, Burns C, Kim D, Dunayevich E, Group C-IS (2013) A randomized, phase 3 trial of naltrexone SR/bupropion SR on weight and obesity-related risk factors (COR-II). Obesity (Silver Spring) 21(5):935–943. https://doi.org/10.1002/oby.20309
Bakris G, Calhoun D, Egan B, Hellmann C, Dolker M, Kingma I, orlistat, resistant hypertension i (2002) Orlistat improves blood pressure control in obese subjects with treated but inadequately controlled hypertension. J Hypertens 20(11):2257–2267. https://doi.org/10.1097/00004872-200211000-00026
Bohula EA, Wiviott SD, McGuire DK, Inzucchi SE, Kuder J, Im K, Fanola CL, Qamar A, Brown C, Budaj A, Garcia-Castillo A, Gupta M, Leiter LA, Weissman NJ, White HD, Patel T, Francis B, Miao W, Perdomo C, Dhadda S, Bonaca MP, Ruff CT, Keech AC, Smith SR, Sabatine MS, Scirica BM, Committee C-TS, Investigators (2018) Cardiovascular Safety of Lorcaserin in Overweight or Obese Patients. N Engl J Med 379(12):1107–1117. https://doi.org/10.1056/NEJMoa1808721
Davies MJ, Bergenstal R, Bode B, Kushner RF, Lewin A, Skjoth TV, Andreasen AH, Jensen CB, DeFronzo RA, Group NNS (2015) Efficacy of liraglutide for weight loss among patients with type 2 diabetes: the SCALE diabetes randomized clinical trial. JAMA 314(7):687–699. https://doi.org/10.1001/jama.2015.9676
Fidler MC, Sanchez M, Raether B, Weissman NJ, Smith SR, Shanahan WR, Anderson CM, Group BCT (2011) A one-year randomized trial of lorcaserin for weight loss in obese and overweight adults: the BLOSSOM trial. J Clin Endocrinol Metab 96(10):3067–3077. https://doi.org/10.1210/jc.2011-1256
Gadde KM, Allison DB, Ryan DH, Peterson CA, Troupin B, Schwiers ML, Day WW (2011) Effects of low-dose, controlled-release, phentermine plus topiramate combination on weight and associated comorbidities in overweight and obese adults (CONQUER): a randomised, placebo-controlled, phase 3 trial. Lancet 377(9774):1341–1352. https://doi.org/10.1016/S0140-6736(11)60205-5
Greenway FL, Fujioka K, Plodkowski RA, Mudaliar S, Guttadauria M, Erickson J, Kim DD, Dunayevich E, Group C-IS (2010) Effect of naltrexone plus bupropion on weight loss in overweight and obese adults (COR-I): a multicentre, randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 376(9741):595–605. https://doi.org/10.1016/S0140-6736(10)60888-4
Hollander P, Gupta AK, Plodkowski R, Greenway F, Bays H, Burns C, Klassen P, Fujioka K, Group CO-DS (2013) Effects of naltrexone sustained-release/bupropion sustained-release combination therapy on body weight and glycemic parameters in overweight and obese patients with type 2 diabetes. Diabetes Care 36(12):4022–4029. https://doi.org/10.2337/dc13-0234
le Roux CW, Astrup A, Fujioka K, Greenway F, Lau DCW, Van Gaal L, Ortiz RV, Wilding JPH, Skjoth TV, Manning LS, Pi-Sunyer X, Group SOPN-S (2017) 3 years of liraglutide versus placebo for type 2 diabetes risk reduction and weight management in individuals with prediabetes: a randomised, double-blind trial. Lancet 389(10077):1399–1409. https://doi.org/10.1016/S0140-6736(17)30069-7
Nissen SE, Wolski KE, Prcela L, Wadden T, Buse JB, Bakris G, Perez A, Smith SR (2016) Effect of naltrexone-bupropion on major adverse cardiovascular events in overweight and obese patients with cardiovascular risk factors: a randomized clinical trial. JAMA 315(10):990–1004. https://doi.org/10.1001/jama.2016.1558
Smith SR, Weissman NJ, Anderson CM, Sanchez M, Chuang E, Stubbe S, Bays H, Shanahan WR, Behavioral M, Lorcaserin for O, Obesity Management Study G (2010) Multicenter, placebo-controlled trial of lorcaserin for weight management. N Engl J Med 363(3):245–256. https://doi.org/10.1056/NEJMoa0909809
Schmidt M, Johannesdottir SA, Lemeshow S, Lash TL, Ulrichsen SP, Botker HE, Sorensen HT (2013) Obesity in young men, and individual and combined risks of type 2 diabetes, cardiovascular morbidity and death before 55 years of age: a Danish 33-year follow-up study. BMJ Open 3(4). https://doi.org/10.1136/bmjopen-2013-002698
Caterson ID, Finer N, Coutinho W, Van Gaal LF, Maggioni AP, Torp-Pedersen C, Sharma AM, Legler UF, Shepherd GM, Rode RA, Perdok RJ, Renz CL, James WP, Investigators S (2012) Maintained intentional weight loss reduces cardiovascular outcomes: results from the Sibutramine Cardiovascular OUTcomes (SCOUT) trial. Diabetes Obes Metab 14(6):523–530. https://doi.org/10.1111/j.1463-1326.2011.01554.x
Kushner RF, Ryan DH (2014) Assessment and lifestyle management of patients with obesity: clinical recommendations from systematic reviews. JAMA 312(9):943–952. https://doi.org/10.1001/jama.2014.10432
Ryan DH, Espeland MA, Foster GD, Haffner SM, Hubbard VS, Johnson KC, Kahn SE, Knowler WC, Yanovski SZ, Look ARG (2003) Look AHEAD (Action for Health in Diabetes): design and methods for a clinical trial of weight loss for the prevention of cardiovascular disease in type 2 diabetes. Control Clin Trials 24(5):610–628. https://doi.org/10.1016/s0197-2456(03)00064-3
Hamman RF, Wing RR, Edelstein SL, Lachin JM, Bray GA, Delahanty L, Hoskin M, Kriska AM, Mayer-Davis EJ, Pi-Sunyer X, Regensteiner J, Venditti B, Wylie-Rosett J (2006) Effect of weight loss with lifestyle intervention on risk of diabetes. Diabetes Care 29(9):2102–2107. https://doi.org/10.2337/dc06-0560
Strelitz J, Ahern AL, Long GH, Hare MJL, Irving G, Boothby CE, Wareham NJ, Griffin SJ (2019) Moderate weight change following diabetes diagnosis and 10 year incidence of cardiovascular disease and mortality. Diabetologia 62(8):1391–1402. https://doi.org/10.1007/s00125-019-4886-1
Iguchi A, Yamakage H, Tochiya M, Muranaka K, Sasaki Y, Kono S, Shimatsu A, Satoh-Asahara N (2013) Effects of weight reduction therapy on obstructive sleep apnea syndrome and arterial stiffness in patients with obesity and metabolic syndrome. J Atheroscler Thromb 20(11):807–820. https://doi.org/10.5551/jat.17632
Ryan D, Heaner M (2014) Guidelines (2013) for managing overweight and obesity in adults. Preface to the full report Obesity (Silver Spring) 22(Suppl 2):S1-3. https://doi.org/10.1002/oby.20819
Kritchevsky SB, Beavers KM, Miller ME, Shea MK, Houston DK, Kitzman DW, Nicklas BJ (2015) Intentional weight loss and all-cause mortality: a meta-analysis of randomized clinical trials. PLoS One 10(3):e0121993. https://doi.org/10.1371/journal.pone.0121993
Ma C, Avenell A, Bolland M, Hudson J, Stewart F, Robertson C, Sharma P, Fraser C, MacLennan G (2017) Effects of weight loss interventions for adults who are obese on mortality, cardiovascular disease, and cancer: systematic review and meta-analysis. BMJ 359:j4849. https://doi.org/10.1136/bmj.j4849
Singh N, Stewart RAH, Benatar JR (2019) Intensity and duration of lifestyle interventions for long-term weight loss and association with mortality: a meta-analysis of randomised trials. BMJ Open 9(8):e029966. https://doi.org/10.1136/bmjopen-2019-029966
Kane JA, Mehmood T, Munir I, Kamran H, Kariyanna PT, Zhyvotovska A, Yusupov D, Suleman UJ, Gustafson DR, McFarlane SI (2019) Cardiovascular Risk Reduction Associated with Pharmacological Weight Loss: A Meta-Analysis. Int J Clin Res Trials 4(1). https://doi.org/10.15344/2456-8007/2019/131
Wilding JPH, Jacob S (2021) Cardiovascular outcome trials in obesity: A review. Obes Rev 22(1):e13112. https://doi.org/10.1111/obr.13112
ClinicalTrials.gov. Semaglutide Effects on Heart Disease and Stroke in Patients With Overweight or Obesity (SELECT) (2018) Available from: https://clinicaltrials.gov/ct2/show/NCT03574597. Accessed May 2021.
EU Clinical Trials Register. A Qsymia™ CardiovascuLAr morbIdity and Mortality (AQCLAIM) Study in subjects with documented cardiovascular disease (2013) Available from: https://www.clinicaltrialsregister.eu/ctr-search/search?query=AQCLAIM. Accessed May 2021
Verma S, Bain SC, Buse JB, Idorn T, Rasmussen S, Orsted DD, Nauck MA (2019) Occurence of first and recurrent major adverse cardiovascular events with liraglutide treatment among patients with type 2 diabetes and high risk of cardiovascular events: a post hoc analysis of a randomized clinical trial. JAMA Cardiol 4(12):1214–1220. https://doi.org/10.1001/jamacardio.2019.3080
Srivastava G, Apovian CM (2018) Current pharmacotherapy for obesity. Nat Rev Endocrinol 14(1):12–24. https://doi.org/10.1038/nrendo.2017.122
Khera R, Murad MH, Chandar AK, Dulai PS, Wang Z, Prokop LJ, Loomba R, Camilleri M, Singh S (2016) Association of Pharmacological Treatments for Obesity With Weight Loss and Adverse Events: A Systematic Review and Meta-analysis. JAMA 315(22):2424–2434. https://doi.org/10.1001/jama.2016.7602
Cardiometabolic risk management guidelines in primary care (2011) Available from: https://www.guidelinecentral.com/summaries/cardiometabolic-risk-management-guidelines-in-primary-care. Accessed May 2021.
Seven E, Husemoen LL, Wachtell K, Ibsen H, Linneberg A, Jeppesen JL (2014) Five-year weight changes associate with blood pressure alterations independent of changes in serum insulin. J Hypertens 32 (11): 2231–2237; discussion 2237. https://doi.org/10.1097/HJH.0000000000000317
Bazzano LA, Hu T, Reynolds K, Yao L, Bunol C, Liu Y, Chen CS, Klag MJ, Whelton PK, He J (2014) Effects of low-carbohydrate and low-fat diets: a randomized trial. Ann Intern Med 161(5):309–318. https://doi.org/10.7326/M14-0180
Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, Hu FB, Hubbard VS, Jakicic JM, Kushner RF, Loria CM, Millen BE, Nonas CA, Pi-Sunyer FX, Stevens J, Stevens VJ, Wadden TA, Wolfe BM, Yanovski SZ, Jordan HS, Kendall KA, Lux LJ, Mentor-Marcel R, Morgan LC, Trisolini MG, Wnek J, Anderson JL, Halperin JL, Albert NM, Bozkurt B, Brindis RG, Curtis LH, DeMets D, Hochman JS, Kovacs RJ, Ohman EM, Pressler SJ, Sellke FW, Shen WK, Smith SC Jr, Tomaselli GF, American College of Cardiology/American Heart Association Task Force on Practice G, Obesity S (2014) 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation 129(25 Suppl 2):S102-138. https://doi.org/10.1161/01.cir.0000437739.71477.ee
Heshmati J, Sepidarkish M, Namazi N, Shokri F, Yavari M, Fazelian S, Khorshidi M, Shidfar F (2019) Impact of dietary calcium supplement on circulating lipoprotein concentrations and atherogenic indices in overweight and obese individuals: a systematic review. J Diet Suppl 16(3):357–367. https://doi.org/10.1080/19390211.2018.1440685
Sepidarkish M, Morvaridzadeh M, Akbari-Fakhrabadi M, Almasi-Hashiani A, Rezaeinejad M, Heshmati J (2019) Effect of omega-3 fatty acid plus vitamin E Co-Supplementation on lipid profile: A systematic review and meta-analysis. Diabetes Metab Syndr 13(2):1649–1656. https://doi.org/10.1016/j.dsx.2019.03.018
Tuccinardi D, Farr OM, Upadhyay J, Oussaada SM, Mathew H, Paschou SA, Perakakis N, Koniaris A, Kelesidis T, Mantzoros CS (2019) Lorcaserin treatment decreases body weight and reduces cardiometabolic risk factors in obese adults: A six-month, randomized, placebo-controlled, double-blind clinical trial. Diabetes Obes Metab 21(6):1487–1492. https://doi.org/10.1111/dom.13655
He Q, Sha S, Sun L, Zhang J, Dong M (2016) GLP-1 analogue improves hepatic lipid accumulation by inducing autophagy via AMPK/mTOR pathway. Biochem Biophys Res Commun 476(4):196–203. https://doi.org/10.1016/j.bbrc.2016.05.086
Hare DL, Toukhsati SR, Johansson P, Jaarsma T (2014) Depression and cardiovascular disease: a clinical review. Eur Heart J 35(21):1365–1372. https://doi.org/10.1093/eurheartj/eht462
Seldenrijk A, Vogelzangs N, Batelaan NM, Wieman I, van Schaik DJ, Penninx BJ (2015) Depression, anxiety and 6-year risk of cardiovascular disease. J Psychosom Res 78(2):123–129. https://doi.org/10.1016/j.jpsychores.2014.10.007
Daray FM, Goldmann E, Gutierrez L, Ponzo J, Lanas F, Mores N, Calandrelli M, Poggio R, Watkins BX, Irazola V (2019) Suicidal ideation is associated with cardiovascular disease in a large, urban cohort of adults in the Southern Cone of Latin America. Gen Hosp Psychiatry 57:34–40. https://doi.org/10.1016/j.genhosppsych.2018.12.006
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8(5):336–341. https://doi.org/10.1016/j.ijsu.2010.02.007
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA, Cochrane Bias Methods G, Cochrane Statistical Methods G (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928. https://doi.org/10.1136/bmj.d5928
Funding
This work was supported by grants from the National Natural Science Foundation of China [81673803].
Author information
Authors and Affiliations
Contributions
L.Z. searched the library and wrote the manuscript text. Z.L and S.L.L extracted data and reviewed all articles. H.H and M.Z evaluated the bias. M.Z designed the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, L., Liu, Z., Liao, S. et al. Cardiovascular safety of long-term anti-obesity drugs in subjects with overweight or obesity: a systematic review and meta-analysis. Eur J Clin Pharmacol 77, 1611–1621 (2021). https://doi.org/10.1007/s00228-021-03160-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-021-03160-7