Abstract
Aims/hypothesis
The angiotensin II receptor type 2 (AT2R) may be a potential therapeutic target for the treatment of hypertension and chronic kidney disease (CKD). The expression and function of AT2R in the vasculature and kidney appear sexually dimorphic. We hypothesised that Agtr2 knockout dams (AT2RKO) with gestational diabetes would program their offspring for subsequent hypertension and CKD in a sex-dependent manner.
Methods
Age- and sex-matched offspring of non-diabetic and diabetic dams of wild-type (WT) and AT2RKO mice were followed from 4 to 20 weeks of age and were monitored for development of hypertension and nephropathy; a mouse podocyte cell line (mPOD) was also studied.
Results
Body weight was progressively lower in female compared with male offspring throughout the lifespan. Female but not male offspring from diabetic AT2RKO dams developed insulin resistance. Compared with the offspring of non-diabetic dams, the progeny of diabetic dams had developed more hypertension and nephropathy (apparent glomerulosclerosis with podocyte loss) at 20 weeks of age; this programming was more pronounced in the offspring of AT2RKO diabetic dams, particularly female AT2RKO progeny. Female AT2RKO offspring had lower basal ACE2 glomerular expression, resulting in podocyte loss. The aberrant ACE2/ACE ratio was far more diminished in glomeruli of female progeny of diabetic AT2RKO dams than in male progeny. Knock-down of Agtr2 in mPODs confirmed the in vivo data.
Conclusions/interpretation
AT2R deficiency accelerated kidney programming in female progeny of diabetic dams, possibly due to loss of protective effects of ACE2 expression in the kidney.
Graphical abstract

Similar content being viewed by others

Introduction
Diabetes during pregnancy (maternal diabetes) in both humans and experimental animal models, whether gestational or pre-gestational (type 1 diabetes mellitus or type 2 diabetes mellitus) is associated with congenital abnormalities of the kidney and urinary tract (CAKUT) [1,2,3,4,5,6]. CAKUT occurs in 3–6 per 1000 live births and is responsible for 34–59% of chronic kidney disease (CKD) in childhood and for 31% of paediatric end-stage renal failure in the USA and Canada [7, 8]. It has been estimated that 4% of CAKUT cases may be associated with maternal diabetes [4, 5].
Maternal diabetes also results in offspring with a two- to fivefold greater risk for various debilitating diseases in adulthood, for example diabetes, obesity, cardiovascular disease, hypertension and CKD [3,4,5,6]. The dysmetabolic features of maternal diabetes and their impact vary with the sex of the offspring. The gene expression and molecular basis of these variations are poorly understood.
The angiotensin II receptor type 2 (AT2R) is highly associated with CAKUT in both humans and mice [9,10,11]. However, the underlying mechanisms that cause kidney malformations related to AT2R variants remain unclear, particularly with respect to the possible molecular and in utero environmental interactions, such as maternal diabetes, which lead to observed kidney abnormalities [7, 8, 12]. The AT2R is expressed in multiple kidney compartments and cells [13, 14]. We [15,16,17] and others [18, 19] have reported aberrant features in the kidney in young Agtr2 knockout (KO) mice.
The intrarenal renin–angiotensin system (RAS) is a key regulator of blood pressure and fluid/electrolyte homeostasis [20,21,22]. In particular, the AT2R via the ACE2–Mas1 receptor (MAS1) pathway counteracts the generally detrimental actions of angiotensin II receptor type 1 (AT1R) such as vasoconstriction, inflammation and proliferation [20,21,22]. Importantly, compelling evidence suggests that AT2R activation is cardio- and renoprotective. Thus, the AT2R may be a potential therapeutic target for the treatment of hypertension, cardiovascular disease and CKD [20,21,22]. Further, the actions of the AT2R in the vasculature and kidneys appear to be sexually dimorphic [23,24,25,26].
Given the rising incidence of diabetes in pregnancy, we speculated that AT2R deficiency in dams that have diabetes mellitus could result in offspring with heightened risks for hypertension and CKD across their lifespan. Previously, we have reported that loss of AT2R results in podocyte loss (mean, 30% fewer) without affecting total nephron number [17]. Here, we studied age- and sex-matched offspring of non-diabetic and diabetic dams, hypothesising that AT2R deficiency resulting in podocyte loss accelerates adverse kidney programming (hypertension and nephropathy) in the progeny of dams with diabetes in a sex-dependent manner, mechanistically mediated by loss of the protective effects of ACE2 expression in the kidney.
Methods
Animal models
Agtr2 KO (AT2RKO) mice (C57BL/6) [9, 10] were generated and kindly provided by T. Inagami (Vanderbilt University School of Medicine, Nashville, TN, USA) as we reported elsewhere [17, 27]. Our murine maternal diabetes model [28,29,30,31], which is induced by a single intraperitoneal streptozotocin (STZ, 150 mg/kg) injection on gestational day E13 is designed to mimic human gestational diabetes with onset late in the second trimester and avoids overt teratogenicity in the offspring [32]. We have documented that STZ administration per se had no toxic effect on kidney development [30] but that the offspring of diabetic dams had a phenotype of low birthweight and low nephron number [28,29,30,31]. Diabetic dams with blood glucose over 16.6 mmol/l (299 mg/dl) post STZ injection were included in the present study.
Age- and sex-matched offspring (male, M and female, F) from the different litters of non-diabetic and diabetic dams of wild-type (WT, C57BL/6) (Charles River, Montreal, QC, Canada) and AT2RKO mice were studied from of 4 weeks until 20 weeks of age. Eight subgroups of mice were included: the offspring of non-diabetic and diabetic WT dams, respectively abbreviated as WT-Con (M/F) and WT-Dia (M/F); and the offspring of non-diabetic and diabetic AT2RKO dams, as KO-Con (M/F) and KO-Dia (M/F), respectively.
All animals were euthanised at 20 weeks (75 mg/kg sodium pentobarbital i.p.) and the kidneys were removed immediately. The biological samples were processed, collected and stored for analysis. Kidneys were either quickly frozen in optimal cutting temperature (OCT) compound or fixed overnight in 4% paraformaldehyde at 4°C before paraffin-embedding.
Animal care and experimental procedures were approved by the Animal Care Committee at the Centre de recherche du centre hospitalier de l’Université de Montréal (CRCHUM). The animals were housed in ventilated cages in specific pathogen-free (SPF) conditions under a 12 h, light–dark cycle with free access to chow and water at the CRCHUM’s animal facility.
Physiological studies
Body weight (g) was measured weekly. Kidney weight (KW, g) and tibia length (TL, mm) were recorded when the animals were euthanised. Longitudinal systolic blood pressure (SBP) (from 14 until 20 weeks of age following 1 week of pre-training) was monitored by the tail-cuff method with a BP-2000 Blood Pressure Analysis System (Visitech Systems, Apex, NC, USA), as reported elsewhere [31, 33,34,35,36]. An IPGTT and an insulin sensitivity test (IST) were performed with 6 and 4 h fasting periods, respectively, at the age of 19 weeks [31, 37]. The GFR was measured by the FITC–inulin method [31, 33,34,35,36] before euthanising at the age of 20 weeks.
Urinary measurements
Urine samples were collected from mice individually housed in metabolic cages. Urinary albumin level was estimated by Coomassie Blue gel staining of electrophoresed urine samples, as reported previously [17]. In brief, 5 μl urine samples from individual mice were temperature denatured and separated using a 10% SDS-PAGE gel and a mouse albumin standard (mouse serum albumin; Exocell, Philadelphia, PA, USA), then stained with Coomassie Blue.
The albumin/creatinine ratio (ACR) (mg/mmol) (Albuwell and Creatinine Companion, Exocell, Philadelphia, PA, USA), urinary angiotensin II (Ang II)/creatinine ratio (pmol/μmol) (Immuno-Biological Laboratories, IBL America, Minneapolis, MN, USA), and angiotensin 1–7 (Ang 1–7)/creatinine ratio (pmol/μmol) (Immuno-Biological Laboratories, IBL America, Minneapolis, MN, USA), were assayed by ELISA and normalised by urinary creatinine levels as described [34,35,36].
Kidney morphology and podocyte number
Kidney morphology was assessed with periodic acid Schiff (PAS) and Masson trichrome staining [17, 31, 33,34,35,36]. Two major features of nephropathy—glomerulosclerosis (based on PAS images, semi-quantitative scale from 0 to 4) and glomerular fibrosis (based on Masson staining)—were scored by a person blinded to the experimental group [17, 31]. Relative immunohistochemistry (IHC)/immunofluorescence (IF) staining intensity and area were quantified using the 2-D staining images (n = 8~ 15 per animal, 6–11 mice/group) were analysed and quantified in a blinded fashion [17, 31, 33,34,35,36]. Brightness and contrast were adjusted on displayed images (identically for compared image sets) and quantified (identical threshold settings for compared image sets) using NIH Image J software (Bethesda, MD, USA) [17, 31, 38, 39]. Podocytes were identified by IF staining of podocyte markers including synaptopodin (Synpo), Wilms tumour 1 (WT1) and p57 in mouse kidney sections [17]. Podocyte density per glomerular area (number per μm2) was performed in a blinded fashion by counting both WT1- and p57-positive nuclear stained cells in glomerular-cross sections, 30–35 glomeruli/mouse, n = 6) [17, 40].
Real-time quantitative PCR
Real-time quantitative PCR (qPCR) (The Fast SYBR green master mix kit and the 7500 Fast real-time PCR system, Applied Biosystems, Life Technologies, Foster City, CA, USA) was performed in the isolated glomeruli [17] by using iron oxide beads (2.5 mg/ml) with the aid of a magnet concentrator [17, 41]. mRNA change in each gene was determined and normalised to its own Actb mRNA, and the percentage change was compared with the expression of the corresponding gene in male WT-Con (1 in fold change) (vs the rest of the subgroups) by using the \( {2}^{-\Delta \Delta {\mathrm{C}}_{\mathrm{t}}} \) method. The primers used are shown in electronic supplementary material (ESM) Table 1.
Immunohistochemical studies and reagents
Both IHC and IF staining were performed using standard protocols [17, 31, 33,34,35,36]. The antibodies used included: anti-β-actin antibody (1:20000) (Sigma-Aldrich, Oakville, ON, Canada); anti-Ang II antibody (1:200) (Phoenix Pharmaceuticals, Burlingame, CA, USA); antibodies to AT1R (1:100), Synpo (P-19) (1:100) and cyclin-dependent kinase inhibitor p57 (H-91) (1:100) (Santa Cruz Biotechnology, Santa Cruz, CA, USA); antibodies to ACE2 (1:400), WT1 (C-19) (1:100); 8-hydroxy-2-deoxyguanosine (8-OHdG) (1:400) (Abcam, Toronto, ON, Canada); anti-ACE antibody (1:200) (Invitrogen, Burlington, ON, Canada); and anti-MAS1 antibody (1:200) (Novus Biologicals, Toronto, ON, Canada).
Podocyte cell line
An immortalised mouse podocyte cell line (mPOD) was kindly donated by S. J. Shankland (University of Washington, WA, USA) [42] as we previously reported [17]. Briefly, mPODs were grown on collagen I-coated plates in a DMEM medium (5 mmol/l glucose) supplemented with 10% FBS (Invitrogen, Burlington, ON, Canada), 100 U/ml penicillin–streptomycin (Invitrogen), and 10 U/ml recombinant mouse IFN-γ (Sigma) at 33°C (defined as a permissive condition). The differentiated mPODs were then cultured under non-permissive conditions; i.e., without IFN-γ at 37°C for 10 days before the specific experiments.
Statistical analysis
For the animal studies, groups of 7 to 18 mice were used (the precise number of animals used for each specific experiment is either labelled in the figures or as individual data points on column scatter graphs). Statistical significance between the experimental groups was analysed by using Prism 6.0 software (GraphPad, San Diego, CA). Statistical significance between the experimental groups was analysed by Student’s t test (in vitro studies) or one-way ANOVA and/or two-way ANOVA, followed by the Bonferroni’s post hoc test (in vivo studies), whenever appropriate. A probability level of p ≤ 0.05 was considered to be statistically significant [17, 31, 33,34,35,36,37].
Results
Offspring growth curves
We compared the growth pattern of age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) from the age of 4 to 20 weeks (Fig. 1a, body weight). During follow-up, mean body weight in the age-matched WT vs KO progeny from non-diabetic and diabetic dams did not differ significantly. Compared with control offspring, the offspring from diabetic dams had lower body weight throughout life (Fig. 1a).
(a) Body weight progression in age-matched offspring 4–19 weeks of age (male + female; WT vs AT2RKO mice; non-diabetic vs diabetic dams). Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001, WT-Dia vs WT-Con; § p ≤ 0.05, §§p ≤ 0.01, §§§p ≤ 0.001, KO-Dia vs KO-Con. (b, c) Body weight in the offspring at 4 (b) and 19 (c) weeks of age. Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (−M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001. (d–f) Longitudinal SBP measurement (d, in total; e, male; f, female) in mice 14–20 weeks of age. Data shown as mean ± SEM; one-way ANOVA followed by Bonferroni’s post hoc test. *p ≤ 0.05, **p ≤ 0.01, WT-Dia vs WT-Con; †p ≤ 0.05, †† p ≤ 0.01, †††p ≤ 0.001, WT-Con vs KO-Con; ǂ p ≤ 0.05, ǂǂ p ≤ 0.01, WT-Dia vs KO-Dia
The body weight progression in the offspring of both WT and KO dams showed a sexually dimorphic pattern (Fig. 1b,c). At 4 weeks of age (Fig. 1b), both sexes of control offspring (WT and AT2RKO) had similar body weights. By contrast, females clearly weighed less than male offspring from diabetic dams (mean body weight: WT-Dia-M vs WT-Dia-F, p < 0.01; KO-Dia-M vs KO-Con-F, p < 0.01). Moreover, female offspring from both non-diabetic and diabetic dams weighed less than male offspring throughout life, for example, mean body weight at 19 weeks (Fig. 1c) was lower (WT-Con-M vs WT-Con-F, p < 0.001; KO-Con-M vs KO-Con-F, p< 0.001; WT-Dia-M vs WT-Dia-F, p < 0.001; KO-Dia-M vs KO-Con-F, p < 0.001).
Physiological measurements and biomarkers
Blood pressure
Longitudinal measurement of SBP (mmHg) was carried out in the offspring (WT vs AT2RKO; non-diabetic vs diabetic dams) from 14 to 20 weeks of age (Fig. 1d; ESM Table 2). Compared with WT-Con, the WT-Dia and AT2RKO offspring (both the KO-Con and KO-Dia) had significantly increased SBP over the follow-up period (Fig. 1d, in total; Fig. 1e, male; Fig. 1f, female). Compared with the sex-matched WT-Con offspring, the increased SBP in WT-Dia offspring is mainly driven by the SBP of male WT-Dia over time (p ≤ 0.05), while female WT-Dia remained normotensive (Fig. 1e,f). Strikingly, when compared with the WT-Dia progeny, female KO-Dia developed significant hypertension (p ≤ 0.05), while male KO-Dia had similar SBP to male WT-Dia (Fig. 1e,f).
IPGTT and IST
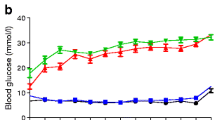
At 19 weeks, an IPGTT (Fig. 2a, in total; Fig. 2b, male; Fig. 2c, female) and an IST (Fig. 3a, in total; Fig. 3b, male; Fig. 3c, female) were conducted. Both WT-Con and KO-Con mice showed the similar baseline of fasting glucose levels (Fig. 2a). Male offspring had higher AUC values than female offspring within the same subgroup (Fig. 2a). Regardless of sex, WT-Dia progeny had significantly impaired glucose tolerance compared with WT-Con mice; however, IPGTTs were the same in KO-Con and KO-Dia mice (Fig. 2b,c). Only KO-Dia, but not WT-Dia, mice showed insulin resistance compared with WT-Con offspring (Fig. 3a). Notably, WT-Dia offspring showed a sexual dimorphic IST response—e.g., male WT-Dia mice developed insulin resistance but female WT-Dia mice had a normal insulin sensitivity (Fig. 3b,c). In contrast, the IST on female KO-Dia mice revealed clear insulin impairment while male KO-Dia mice had normal insulin responses (Fig. 3b,c).
IPGTT and IPGTT AUC (% of WT-Con) quantification (0–120 min) in age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 19 weeks. (a) The offspring in total; data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001. (b) Male offspring. (c) Female offspring. (b, c) Data shown as mean ± SEM; one-way ANOVA followed by Bonferroni’s post hoc test; *p ≤ 0.05, ***p ≤ 0.001
IST and IST AUC (% of WT-Con) quantification (0–90 min) in age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 19 weeks. (a) The offspring in total; data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]. *p ≤ 0.05, **p ≤ 0.01. (b) Male offspring. (c) Female offspring. (b, c) Data shown as mean ± SEM; one-way ANOVA followed by Bonferroni’s post hoc test; *p ≤ 0.05, **p ≤ 0.01
Kidney variables
Both WT-Con and KO-Con offspring had similar basal GFR at the age of 20 weeks (Fig. 4a), regardless of sex. Consistently, GFR levels in the offspring of diabetic dams (both WT-Dia and KO-Dia) increased significantly in both sexes, profoundly so in KO-Dia offspring (vs WT-Dia, p < 0.01), especially in the female KO-Dia progeny (vs KO-Dia-M, p < 0.05).
Physiological measurements (a, b) and urine measurements (c–f) in age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 20 weeks. (a) GFR measurement. (b) KW/TL (mg/mm) ratio. (c) Coomassie Blue gel staining. Mouse serum albumin (MSA, μg) was used as a standard. (d) Urinary ACR. (e) Urinary Ang II/creatinine (pmol/μmol) levels; (f) Urinary Ang 1–7/creatinine (pmol/μmol) levels. (a, b; d–f) Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]; *p ≤ 0.05, ** p ≤ 0.01, *** p ≤ 0.001
The KW/TL ratio was higher in AT2RKO offspring than in WT offspring (p < 0.01); and in male offspring than in female offspring (Fig. 4b) (WT-Con-M vs WT-Con-F, p < 0.05; KO-Con-M vs KO-Con-F, p < 0.05; WT-Dia-M vs WT-Dia-F, p < 0.001; KO-Dia-M vs KO-Dia-F, p < 0.001). There was no apparent difference in the offspring from non-diabetic or diabetic dams. KW and glomerular numbers per kidney cortex area among all the subgroups are shown in ESM Fig. 1 and ESM Fig. 2, respectively.
Urinary measurements
Compared with respective control offspring from non-diabetic dams, both WT-Dia and KO-Dia offspring had detectable albuminuria by Coomassie Blue staining of urine, regardless of sex (Fig. 4c). However, we did not detect any significant differences in the urinary ACR (Fig. 4d) in any of the subgroups. In addition, only KO-Dia offspring had increased urinary Ang II/creatinine (pmol/μmol) ratio, which was mainly contributed by female KO-Dia offspring (KO-Con-F vs KO-Con-M, p < 0.05) (Fig. 4e). Urinary Ang 1–7/creatinine ratios (pmol/μmol) were similar in all the subgroups (Fig. 4f).
Kidney pathology and intrarenal biomarker expression
Kidney morphology
Kidney morphology was examined on sections stained with PAS (Fig. 5a,b) and Masson trichrome (Fig. 5a,c). Compared with the respective WT-Con offspring, the progeny (WT-Dia and KO-Dia) of both diabetic WT and AT2RKO dams displayed more evidence of nephropathy (apparent glomerulosclerosis in combined with glomerular extracellular matrix protein accumulation) at 20 weeks. Those kidney changes were more pronounced in KO-Dia offspring, female KO-Dia offspring in particular (Fig. 5a–c). The kidney fibrosis among all the subgroups was further confirmed by Tgfb1 mRNA expression (ESM Fig. 3) as well. 8-OHdG staining (Fig. 5a,d) showed an oxidative stress pattern in the glomeruli, similar to changes revealed in the kidney morphologic staining discussed above (Fig. 5a–c), but without sexual differences in KO-Dia offspring.
Kidney morphology in age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 20 weeks. (a) Kidney morphologic images of PAS, Masson’s trichrome and 8-OHdG IHC staining in male and female mice; scale bar, 50 μm. (b–d) Semi-quantification of staining. (b) Glomerulosclerosis injury score based on PAS staining (scale from 0 to 4: Grade 0, normal glomeruli; Grade 1, presence of mesangial expansion/thickening of the basement membrane; Grade 2, mild/moderate segmental hyalinosis/sclerosis involving less than 50% total glomerular area; Grades 3 and 4, glomeruli are solidified and smaller than Grade 0 glomeruli [Grade 3 as 50% to 75% sclerosis; and Grade 4 as 76% to 100% sclerosis]. (c) Glomerular fibrosis per glomerulus based on Masson staining, expressed as % of WT-Con-Male, set at 100%; (d) 8-OHdG IHC-positive nuclei per glomerulus, expressed as % of WT-Con-Male, set at 100%;. Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]; *p ≤ 0.05; ** p ≤ 0.01. *** p ≤ 0.001
Ang II and intrarenal RAS gene expression in the kidney
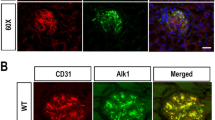
We examined Ang II (Fig. 6a,b) and several intrarenal RAS components including AT1R (Fig. 6a,c), ACE (Fig. 6a,d), ACE2 (Fig. 6a,e) and MAS1 (Fig. 6a,f) IF/IHC-protein expression in the kidneys of these animal subgroups. Compared with the control offspring, the offspring of diabetic dams had heightened Ang II-IF protein expression, but this was pronounced in female progeny from diabetic dams (male vs female, p < 0.001), while there was no apparent difference between WT and AT2RKO mice. Compared with WT-Con, AT1R-IF, ACE-IF and MAS1-IHC protein expression were increased, while ACE2-IF protein expression was not affected in the kidney of WT-Dia offspring. By contrast, AT2RKO offspring (KO-Con vs KO-Dia; male vs female) had similar levels of AT1R-IF, ACE-IF and MAS1- IHC protein expression in their kidneys.
Intrarenal RAS protein expression in the kidney of age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 20 weeks. (a) IHC and IF images in male and female mice: Ang II-IHC, AT1R-IF, ACE-IF, ACE2-IF and MAS1-IHC staining; scale bar, 50 μm. (b–f) Semi-quantification of IHC/IF staining. (b) Ang II-IHC; (c) AT1R-IF; (d) ACE-IF; (e) ACE2-IF; and (f) MAS1-IHC. Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]; *p ≤ 0.05, ** p ≤ 0.01, *** p ≤ 0.001
Notably, the increased AT1R-IF protein was mainly driven by male WT-Dia offspring (WT-Dia-M vs WT-Dia-F, p < 0.001), while the similar MAS1-IHC protein expression was seen in both sexes of mice within the same subgroup. Strikingly, ACE2-IF protein expression was consistently lower in the kidneys of female but not male WT-Dia and KO-Dia offspring (WT-Dia-M vs WT-Dia-F, p < 0.01; KO-Dia-M vs KO-Dia-F, p < 0.001).
Podocyte morphology/numbers
We examined several podocyte markers (Synpo, Nephrin, WT1, and p57) and their gene expression in these animal subgroups (Fig. 7). Synpo (Fig. 7a) and Nphs1 (encoding nephrin) (Fig. 7b) mRNA expression in the glomeruli were decreased in KO-Con compared with WT-Con mice, and the levels were much lower in female than in male KO-Con offspring. In the presence of maternal diabetes, the expression of these genes was further decreased in the glomeruli of KO-Dia offspring (vs WT-Dia), more so in female offspring. These results were confirmed by podocyte loss estimated by Synpo (Fig. 7c,d), p57 (Fig. 7c,e) and WT1 IF staining (Fig. 7c,f).
Podocyte studies in age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 20 weeks. (a, b) qPCR in isolated glomeruli. (a) Synpo and (b) Nphs1 mRNA expression. (c) IF staining images in male and female mice: Synpo-IF (Synpo, green); p57-IF (p57, red; DAPI, blue); WT1-IF (WT1, red; DAPI, blue); scale bar, 50 μm; dashed circle, glomerulus. (d–f) Semi-quantification of IF staining. (d) Synpo; (e) p57; and (f) WT1. (a, b; d–f) Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in a sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]; *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Intrarenal RAS gene expression in the glomeruli
We further examined intraglomerular mRNA levels of Agtr1a, Agtr2, Ace, Ace2 and Mas1 in isolated glomeruli of all animal subgroups (qPCR of Agtr1a [Fig. 8a], Agtr2 [Fig. 8b] and Mas1 [Fig. 8c]) genes as well as the Ace2/Ace ratio [Fig. 8d]; ESM Fig. 4, qPCR of Ace and Ace2 genes). Compared with WT-Con offspring, the increased mRNA expression of Agtr1a and Mas1 genes, the decreased Agtr2 mRNA expression and the unaffected Ace2/Ace ratio were shown in glomeruli of both sexes of WT-Dia offspring. Notably, lower Agtr1a and higher Agtr2 mRNA expression were evident in the glomeruli of female compared with male offspring within the same WT subgroup. In contrast, the mRNA levels of Agtr1a and Mas1 genes were completely unaffected in glomeruli of AT2RKO mice, regardless of sex. Most importantly, both sexes of KO-Dia offspring had a significantly lower expression of the Ace2/Ace ratio compared with WT-Dia and KO-Con, more pronounced in female KO-Dia progeny.
In vivo (a–d) and in vitro (e–h) studies. (a–d) qPCR in isolated glomeruli from the age- and sex-matched offspring of non-diabetic and diabetic dams (WT vs AT2RKO mice) at 20 weeks. mRNA expression of (a) Agtr1a; (b) Agtr2; (c) Mas1; and (d) the Ace2/Ace ratio. Data shown as mean ± SEM; one-way ANOVA, followed by Bonferroni’s post hoc test in comparison of four subgroups in total (WT-Con, KO-Con, WT-Dia and KO-Dia); two-way ANOVA, followed by Bonferroni’s post hoc test in comparison of eight subgroups in sex-specific manner [WT-Con (-M/F), KO-Con (-M/F), WT-Dia (-M/F) and KO-Dia (-M/F)]. *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001. (e–h) The in vitro study of mPODs treated with 50 nmol/l scrambled (Scr.; blue bars) or 50 nmol/l Agtr2 siRNA (pink bars). (e) Synpo-IF staining and its semi-quantification (scale bar, 50 μm); (f) DHE staining and its semi-quantification (scale bar, 50 μm). (g) qPCR of Agtr1a, Agtr2, Ace, Ace2 and Mas1 mRNA. (h) IF staining of AT1R, ACE, ACE2 and MAS1 as well as its corresponding semi-quantification (scale bar, 50 μm). (e–h) Three to four separate experiments; data shown as mean ± SEM; an unpaired Student’s t test; *p ≤ 0.05, ***p ≤ 0.001 vs mPODs cultured with scrambled siRNA (set at 100%)
Studies in cultured mouse podocytes
We further validated several of our in vivo findings by knocking-down Agtr2 using Agtr2 siRNA in mouse podocytes (mPODs: Fig. 8e–h). Compared with scrambled siRNA (50 nmol/l), treatment with Agtr2 siRNA (50 nmol/l) inhibited Synpo protein expression and disoriented podocyte integrity (Fig. 8e, IF). It also increased oxidative stress revealed by dihydroethidium (DHE) staining (a cell-permeable fluorescent dye, redox indicator) in mPODs (Fig. 8f). In addition, Agtr2 siRNA decreased gene expression of Ace and Ace2 whereas Agtr1a gene expression was unaffected (Fig. 8g, qPCR; Fig. 8h, IF). Although Mas1 mRNA was significantly decreased by Agtr2 siRNA, podocyte morphology remained relatively normal compared with mPODs treated with scrambled RNA.
Discussion
In the present study, we demonstrated that AT2R deficiency led to more pronounced nephropathy in the progeny of diabetic dams. These changes were more pronounced in female offspring; we postulate this was possibly due to loss of the protective effects of ACE2 expression in their kidneys.
During the follow-up period, overall, AT2RKO offspring had similar weights to WT offspring; the body weight of the offspring of diabetic dams was lower compared with that of the offspring of non-diabetic dams, and female offspring were significantly lighter than male offspring. This disparity in body weight led us to speculate that kidney programming might be a factor in the low-birthweight offspring in a sex-dependent manner given that low birthweight is associated with a higher risk of CKD in both experimental data [28, 29] and in humans [4, 43].
Body weight has been associated with additional sexually dimorphic variations, such as later metabolic changes [44]. Consistent with a previous report [29], both sexes of WT-Dia progeny showed significantly impaired glucose tolerance. Intriguingly, IPGTT results were unaltered in both sexes of KO-Dia offspring. KO-Dia mice developed significant insulin resistance that appeared driven by female KO-Dia mice, since male KO-Dia mice had a normal insulin response. These data are in agreement with the studies of Quiroga et al. [45], who reported unaltered IPGTT and impaired IST in female AT2RKO mice. Since WT and AT2RKO offspring had similar body weights, a key distinguishing factor might be related to sex hormones, which play a contributing role in AT2R action. It has been known that AT2R stimulation has had more pronounced effects in females [23,24,25,26]. While oestrogen upregulates AT2R expression [26, 46], testosterone, via androgen receptor-mediated extracellular signal-regulated protein kinase (ERK)1/2/mitogen-activated protein (MAP) kinase-dependent mechanisms, could downregulate AT2R expression [47].
Both WT and AT2RKO offspring from non-diabetic and diabetic dams have similar kidney weight and glomerular numbers; however, the obvious kidney hypertrophy (revealed by KW/TL ratio) and higher GFR in KO-Dia offspring may lead to a higher risk of subsequent hypertension and injury [27, 48], compared with the mild hypertension phenotype in KO-Con animals [9, 13, 27]. Sex-specific differences in blood pressure levels related to maternal diabetes are known in both experimental and human studies [29, 49, 50]. For example, human studies have suggested that offspring of diabetic mothers seem to be at higher risk of developing hypertension than the offspring of non-diabetic mothers, and that this difference is more clearly evident in male than female offspring [49, 50]. While confirming that WT-Dia offspring are prone to developing hypertension in adulthood [29], we found that female KO-Dia offspring developed more pronounced SBP elevation with higher incidence of hyperfiltration compared with both male WT-Dia and male KO-Dia offspring over time. Although albuminuria is present, as is revealed by Coomassie Blue gel staining in both WT-Dia and KO-Dia offspring, the ACR was not statistically different among the subgroups, suggesting an adaptive capacity of mature C57BL/6 mice during an early stage of nephropathy.
In addition, both sexes of progeny of diabetic AT2RKO dams (KO-Dia, M/F) develop greater nephropathy and elevated oxidative stress. Such kidney damage is far more evident in female KO-Dia offspring. The mechanisms underlying sexual dimorphism seen here in the progeny of diabetic dams remain poorly understood. The presence of intrarenal RAS dysfunction and activation of oxidative stress has been suggested [28, 29, 51, 52]. Here, we confirmed evidence of elevated oxidative stress in the kidneys of the offspring of diabetic dams [28, 29] and found that the level of Ang II was also increased. However, only female KO-Dia offspring had elevated Ang II (but not Ang 1–7) excretion in urine, hinting at a disturbance of intrarenal RAS.
Although AT2R expression decreases significantly within days after birth [22, 53], notably, the decline in renal AT2R expression is greater in males [53]. Moreover, the axis of renal Agtr2/Ace2/Ang 1–7/Mas1 gene expression has been reported as greater in female (both adult [24, 26, 53] and ageing [24, 54]) rodents, suggesting the shift of depressor RAS pathways in females, which protects female rodents from hypertension and kidney injury. Consistent with previous reports [28, 29], compared with WT-Con offspring, AT1R-IF, ACE-IF and MAS1-IHC expression were increased, while ACE2-IF expression was not affected in the kidney of WT-Dia offspring (WT-Con vs WT-Dia; male vs female). Notably, ACE2-IF expression was consistently lower in the kidneys of female but not male WT-Dia and KO-Dia offspring, while AT1R-IF, ACE-IF and MAS1-IHC expression remained unchanged in AT2RKO offspring (KO-Con vs KO-Dia; male vs female). Together, these data suggest that loss of ACE2 expression in the kidney might implicate the pronounced kidney programming in female KO-Dia offspring.
Podocytes express AT2R and play a key role in maintaining the integrity and function of the glomerular filtration barrier [14, 17]. Consistent with our previous findings that AT2R deficiency has more impact on podocyte integrity than on nephron numbers [17], we found that AT2R deficiency resulted in podocyte loss in diabetic progeny in a sex-dependent manner, more pronounced in female KO-Dia offspring. We examined several podocyte markers (Synpo, Nephrin, WT1 and p57) and observed that their gene expression was further decreased in the glomeruli of KO-Dia offspring (vs WT-Dia), and more so in female KO-Dia offspring. Mechanistically, the Ace2/Ace ratio further declined in isolated glomeruli, which was more pronounced in female KO-Dia progeny, while Agtr1a and Mas1 mRNA was not affected. Finally, we have validated podocyte morphology/integrity (Synpo-IF staining), oxidative stress (DHE staining) and the gene expression of these RAS components (qPCR and IF staining) in vitro by using Agtr2 siRNA (vs scrambled siRNA) in mPODs to confirm our in vivo findings.
Our present studies have certain limitations. The level of intrarenal ACE2 activity requires further validation in the current model. Moreover, ACE2 is primarily expressed in the brush border of the renal proximal tubule [27, 33,34,35]. We have reported that basal Ace2 mRNA and protein in isolated proximal tubules is decreased in AT2RKO mice [27]; and ACE2, through decreasing renal oxidative stress-mediated signalling, protects diabetes-related glomerular and tubular injury and prevents the development of hypertension [27, 33,34,35]. Therefore, a contribution through ACE2 downregulation in the proximal tubule seems likely. To date, little is known about how AT2R knockout leads to a diminution in ACE2 in the renal proximal tubule and how that influences kidney programming and related sexual dimorphism.
In conclusion, our data suggest that loss of AT2R protective effects may lead to a higher risk of hypertension and kidney damage in the progeny of diabetic dams, particularly among female offspring. We propose that the dysfunction of intrarenal RAS and/or activation of oxidative stress mediate sexual dimorphism in KO-Dia offspring with pronounced kidney programming. Prospectively, novel therapeutic strategies to prevent AT2R loss may provide a means to decrease the heightened risks for adverse kidney programming in the offspring of diabetic mothers.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- ACR:
-
Albumin/creatinine ratio
- Ang II:
-
Angiotensin II
- AT1R:
-
Angiotensin II receptor type 1
- AT2R:
-
Angiotensin II receptor type 2
- AT2RKO:
-
Agtr2 knockout (mice)
- CAKUT:
-
Congenital abnormalities of the kidney and urinary tract
- CKD:
-
Chronic kidney disease
- DHE:
-
Dihydroethidium
- IF:
-
Immunofluorescence
- IHC:
-
Immunohistochemistry
- IST:
-
Insulin sensitivity test
- KO:
-
Knockout
- KO-Con (-M/F):
-
Knockout control offspring from non-diabetic dams (male/female)
- KO-Dia (-M/F):
-
Knockout offspring from diabetic dams (male/female)
- KW:
-
Kidney weight
- MAS1:
-
Mas1 receptor
- mPOD:
-
Mouse podocyte cell line
- 8-OHdG:
-
8-Hydroxy-2-deoxyguanosine
- PAS:
-
Periodic acid Schiff
- qPCR:
-
Real-time quantitative PCR
- RAS:
-
Renin–angiotensin system
- SBP:
-
Systolic blood pressure
- STZ:
-
Streptozotocin
- Synpo:
-
Synaptopodin
- TL:
-
Tibia length
- WT:
-
Wild-type
- WT-Con (-M/F):
-
Wild-type control offspring from non-diabetic dams (male/female)
- WT-Dia (-M/F):
-
Wild-type offspring from diabetic dams (male/female)
- WT1:
-
Wilms tumour 1
References
Balsells M, Garcia-Patterson A, Gich I, Corcoy R (2009) Maternal and fetal outcome in women with type 2 versus type 1 diabetes mellitus: a systematic review and metaanalysis. J Clin Endocrinol Metab 94:4284–4291. https://doi.org/10.1210/jc.2009-1231
Balsells M, Garcia-Patterson A, Gich I, Corcoy R (2012) Major congenital malformations in women with gestational diabetes mellitus: a systematic review and meta-analysis. Diabetes Metab Res Rev 28:252–257
Marshall SM (2019) A life course perspective on diabetes: developmental origins and beyond. Diabetologia 62:1737–1739. https://doi.org/10.1007/s00125-019-4954-6
Dart AB, Ruth CA, Sellers EA, Au W, Dean HJ (2015) Maternal diabetes mellitus and congenital anomalies of the kidney and urinary tract (CAKUT) in the child. Am J Kidney Dis 65:684–691. https://doi.org/10.1053/j.ajkd.2014.11.017
Parimi M, Nitsch D (2020) A systematic review and meta-analysis of diabetes during pregnancy and congenital genitourinary abnormalities. Kidney Int Rep 5:678–693. https://doi.org/10.1016/j.ekir.2020.02.1027
Plagemann A (2011) Maternal diabetes and perinatal programming. Early Hum Dev 87:743–747. https://doi.org/10.1016/j.earlhumdev.2011.08.018
Yosypiv IV (2011) Renin-angiotensin system in ureteric bud branching morphogenesis: insights into the mechanisms. Pediatr Nephrol 26:1499–1512. https://doi.org/10.1007/s00467-011-1820-2
Yosypiv IV (2012) Congenital anomalies of the kidney and urinary tract: a genetic disorder? Int J Nephrol 2012:909083. https://doi.org/10.1155/2012/909083
Ichiki T, Labosky PA, Shiota C et al (1995) Effects on blood pressure and exploratory behaviour of mice lacking angiotensin II type-2 receptor. Nature 377:748–750. https://doi.org/10.1038/377748a0
Nishimura H, Yerkes E, Hohenfellner K et al (1999) Role of the angiotensin type 2 receptor gene in congenital anomalies of the kidney and urinary tract, CAKUT, of mice and men. Mol Cell 3:1–10. https://doi.org/10.1016/S1097-2765(00)80169-0
Schedl A (2007) Renal abnormalities and their developmental origin. Nat Rev Genet 8:791–802. https://doi.org/10.1038/nrg2205
Mitanchez D, Yzydorczyk C, Siddeek B, Boubred F, Benahmed M, Simeoni U (2015) The offspring of the diabetic mother--short- and long-term implications. Best Pract Res Clin Obstet Gynaecol 29:256–269. https://doi.org/10.1016/j.bpobgyn.2014.08.004
Ozono R, Wang ZQ, Moore AF, Inagami T, Siragy HM, Carey RM (1997) Expression of the subtype 2 angiotensin (AT2) receptor protein in rat kidney. Hypertension 30:1238–1246. https://doi.org/10.1161/01.HYP.30.5.1238
Suzuki K, Han GD, Miyauchi N et al (2007) Angiotensin II type 1 and type 2 receptors play opposite roles in regulating the barrier function of kidney glomerular capillary wall. Am J Pathol 170:1841–1853. https://doi.org/10.2353/ajpath.2007.060484
Chen YW, Tran S, Chenier I et al (2008) Deficiency of intrarenal angiotensin II type 2 receptor impairs paired homeo box-2 and N-myc expression during nephrogenesis. Pediatr Nephrol 23:1769–1777. https://doi.org/10.1007/s00467-008-0854-6
Zhang SL, Chen YW, Tran S et al (2007) Pax-2 and N-myc regulate epithelial cell proliferation and apoptosis in a positive autocrine feedback loop. Pediatr Nephrol 22:813–824. https://doi.org/10.1007/s00467-007-0444-z
Liao MC, Zhao XP, Chang SY et al (2017) AT2 R deficiency mediated podocyte loss via activation of ectopic hedgehog interacting protein (Hhip) gene expression. J Pathol 243:279–293. https://doi.org/10.1002/path.4946
Oshima K, Miyazaki Y, Brock JW III, Adams MC, Ichikawa I, Pope JC (2001) Angiotensin type II receptor expression and ureteral budding. J Urol 166:1848–1852. https://doi.org/10.1016/S0022-5347(05)65703-5
Song R, Spera M, Garrett C, El-Dahr SS, Yosypiv IV (2010) Angiotensin II AT2 receptor regulates ureteric bud morphogenesis. Am J Physiol Renal Physiol 298:F807–F817. https://doi.org/10.1152/ajprenal.00147.2009
Carey RM (2017) Update on angiotensin AT2 receptors. Curr Opin Nephrol Hypertens 26:91–96. https://doi.org/10.1097/MNH.0000000000000304
Chow BS, Allen TJ (2016) Angiotensin II type 2 receptor (AT2R) in renal and cardiovascular disease. Clin Sci (Lond) 130:1307–1326. https://doi.org/10.1042/CS20160243
Colafella KM, Hilliard LM, Denton KM (2016) Epochs in the depressor/pressor balance of the renin-angiotensin system. Clin Sci (Lond) 130:761–771. https://doi.org/10.1042/CS20150939
Hilliard LM, Jones ES, Steckelings UM, Unger T, Widdop RE, Denton KM (2012) Sex-specific influence of angiotensin type 2 receptor stimulation on renal function: a novel therapeutic target for hypertension. Hypertension 59:409–414. https://doi.org/10.1161/HYPERTENSIONAHA.111.184986
Mirabito KM, Hilliard LM, Kett MM et al (2014) Sex- and age-related differences in the chronic pressure-natriuresis relationship: role of the angiotensin type 2 receptor. Am J Physiol Ren Physiol 307:F901–F907. https://doi.org/10.1152/ajprenal.00288.2014
Maleki M, Nematbakhsh M (2016) Gender difference in renal blood flow response to angiotensin II administration after ischemia/reperfusion in rats: the role of AT2 receptor. Adv Pharmacol Sci 2016:7294942. https://doi.org/10.1155/2016/7294942
Lee SH, Lee YH, Jung SW et al (2019) Sex-related differences in the intratubular renin-angiotensin system in two-kidney, one-clip hypertensive rats. Am J Physiol Ren Physiol 317:F670–f682. https://doi.org/10.1152/ajprenal.00451.2018
Chang SY, Chen YW, Chenier I, Tran Sle M, Zhang SL (2011) Angiotensin II type II receptor deficiency accelerates the development of nephropathy in type I diabetes via oxidative stress and ACE2. Exp Diabetes Res 2011:521076. https://doi.org/10.1155/2011/521076
Chang SY, Chen YW, Zhao XP et al (2012) Catalase prevents maternal diabetes-induced perinatal programming via the Nrf2-HO-1 defense system. Diabetes 61:2565–2574. https://doi.org/10.2337/db12-0248
Chen YW, Chenier I, Tran S, Scotcher M, Chang SY, Zhang SL (2010) Maternal diabetes programs hypertension and kidney injury in offspring. Pediatr Nephrol 25:1319–1329. https://doi.org/10.1007/s00467-010-1506-1
Tran S, Chen YW, Chenier I et al (2008) Maternal diabetes modulates renal morphogenesis in offspring. J Am Soc Nephrol 19:943–952. https://doi.org/10.1681/ASN.2007080864
Aliou Y, Liao MC, Zhao XP et al (2016) Post-weaning high-fat diet accelerates kidney injury, but not hypertension programmed by maternal diabetes. Pediatr Res 79:416–424. https://doi.org/10.1038/pr.2015.236
Ornoy A (2007) Embryonic oxidative stress as a mechanism of teratogenesis with special emphasis on diabetic embryopathy. Reprod Toxicol 24:31–41. https://doi.org/10.1016/j.reprotox.2007.04.004
Lo CS, Liu F, Shi Y et al (2012) Dual RAS blockade normalizes angiotensin-converting enzyme-2 expression and prevents hypertension and tubular apoptosis in Akita angiotensinogen-transgenic mice. Am J Physiol Renal Physiol 302:F840–F852. https://doi.org/10.1152/ajprenal.00340.2011
Lo CS, Shi Y, Chang SY et al (2015) Overexpression of heterogeneous nuclear ribonucleoprotein F stimulates renal Ace-2 gene expression and prevents TGF-β1-induced kidney injury in a mouse model of diabetes. Diabetologia 58:2443–2454. https://doi.org/10.1007/s00125-015-3700-y
Shi Y, Lo CS, Padda R et al (2015) Angiotensin-(1-7) prevents systemic hypertension, attenuates oxidative stress and tubulointerstitial fibrosis, and normalizes renal angiotensin-converting enzyme 2 and Mas receptor expression in diabetic mice. Clin Sci (Lond) 128:649–663. https://doi.org/10.1042/CS20140329
Zhao S, Ghosh A, Lo CS et al (2018) Nrf2 deficiency upregulates intrarenal angiotensin-converting enzyme-2 and angiotensin 1-7 receptor expression and attenuates hypertension and nephropathy in diabetic mice. Endocrinology 159:836–852. https://doi.org/10.1210/en.2017-00752
Nchienzia H, Liao MC, Zhao XP et al (2019) Hedgehog interacting protein (Hhip) regulates insulin secretion in mice fed high fat diets. Sci Rep 9:11183
Rangan GK, Tesch GH (2007) Quantification of renal pathology by image analysis. Nephrology (Carlton, Vic) 12:553–558. https://doi.org/10.1111/j.1440-1797.2007.00855.x
Crowe AR, Yue W (2019) Semi-quantitative determination of protein expression using immunohistochemistry staining and analysis: an integrated protocol. Bio-protocol 9(24):e3465
Zhang J, Pippin JW, Vaughan MR et al (2012) Retinoids augment the expression of podocyte proteins by glomerular parietal epithelial cells in experimental glomerular disease. Nephron Exp Nephrol 121:e23–e37. https://doi.org/10.1159/000342808
Zhong F, Wang W, Lee K, He JC, Chen N (2016) Role of C/EBP-alpha in adriamycin-induced podocyte injury. Sci Rep 6:33520
Mundel P, Reiser J, Zuniga Mejia BA et al (1997) Rearrangements of the cytoskeleton and cell contacts induce process formation during differentiation of conditionally immortalized mouse podocyte cell lines. Exp Cell Res 236:248–258. https://doi.org/10.1006/excr.1997.3739
Gjerde A, Reisæter AV, Skrunes R, Marti HP, Vikse BE (2020) Intrauterine growth restriction and risk of diverse forms of kidney disease during the first 50 years of life. Clin J Am Soc Nephrol CJASN. https://doi.org/10.2215/CJN.04080320
Ingvorsen C, Karp NA, Lelliott CJ (2017) The role of sex and body weight on the metabolic effects of high-fat diet in C57BL/6N mice. Nutr Diabetes 7:e261. https://doi.org/10.1038/nutd.2017.6
Quiroga DT, Miquet JG, Gonzalez L et al (2019) Mice lacking angiotensin type 2 receptor exhibit a sex-specific attenuation of insulin sensitivity. Mol Cell Endocrinol 498:110587. https://doi.org/10.1016/j.mce.2019.110587
Sampson AK, Hilliard LM, Moritz KM et al (2012) The arterial depressor response to chronic low-dose angiotensin II infusion in female rats is estrogen dependent. Am J Physiol Regul Integr Comp Physiol 302:R159–R165. https://doi.org/10.1152/ajpregu.00256.2011
Mishra JS, Hankins GD, Kumar S (2016) Testosterone downregulates angiotensin II type-2 receptor via androgen receptor-mediated ERK1/2 MAP kinase pathway in rat aorta. J Renin-Angiotensin-Aldosterone System JRAAS 17
Brenner BM, Garcia DL, Anderson S (1988) Glomeruli and blood pressure. Less of one, more the other? Am J Hypertens 1:335–347. https://doi.org/10.1093/ajh/1.4.335
Aceti A, Santhakumaran S, Logan KM et al (2012) The diabetic pregnancy and offspring blood pressure in childhood: a systematic review and meta-analysis. Diabetologia 55:3114–3127. https://doi.org/10.1007/s00125-012-2689-8
Miranda JO, Cerqueira RJ, Barros H, Areias JC (2019) Maternal diabetes mellitus as a risk factor for high blood pressure in late childhood. Hypertension 73:e1–e7
Colafella KMM, Denton KM (2018) Sex-specific differences in hypertension and associated cardiovascular disease. Nat Rev Nephrol 14:185–201. https://doi.org/10.1038/nrneph.2017.189
Yan J, Li X, Su R, Zhang K, Yang H (2014) Long-term effects of maternal diabetes on blood pressure and renal function in rat male offspring. PLoS One 9:e88269. https://doi.org/10.1371/journal.pone.0088269
Sampson AK, Moritz KM, Denton KM (2012) Postnatal ontogeny of angiotensin receptors and ACE2 in male and female rats. Gend Med 9:21–32. https://doi.org/10.1016/j.genm.2011.12.003
Mirabito KM, Hilliard LM, Head GA, Widdop RE, Denton KM (2014) Pressor responsiveness to angiotensin II in female mice is enhanced with age: role of the angiotensin type 2 receptor. Biol Sex Differ 5:13
Acknowledgements
Some of the data were presented as abstracts at the Organization for the Study of Sex Differences (OSSD) meeting in 2019 and the 14e Journée Scientifique Annuelle du Centre de Recherche du Diabète de Montréal (MDRC) in 2020. We thank a professional editor (Montreal, Canada) for editing our manuscript.
Authors’ relationships and activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Funding
This project was supported by grants to SLZ from the Canadian Institutes of Health Research (CIHR)-Catalyst Grant (SVB 158606).
Author information
Authors and Affiliations
Contributions
SLZ is the guarantor of this work, had full access to all study data, and takes responsibility for data integrity and the accuracy of data analysis. JSDC and SLZ were principal investigators and were responsible for the study conception and design. SLZ drafted/reviewed/edited the manuscript. MCL, YCP, SYC, XPZ, IC and SLZ contributed to the experiments and data collection. JRI contributed to data discussion and reviewed/edited the manuscript. All authors were involved in the analysis and interpretation of data and contributed to the critical revision of the manuscript. All authors provided final approval of the version to be published.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM
(PDF 191 kb)
Rights and permissions
About this article
Cite this article
Liao, MC., Pang, YC., Chang, SY. et al. AT2R deficiency in mice accelerates podocyte dysfunction in diabetic progeny in a sex-dependent manner. Diabetologia 64, 2108–2121 (2021). https://doi.org/10.1007/s00125-021-05483-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-021-05483-7